Ankylosing Spondylitis: Symptoms, Causes and How It’s Treated
 By: by Amino Science
By: by Amino Science
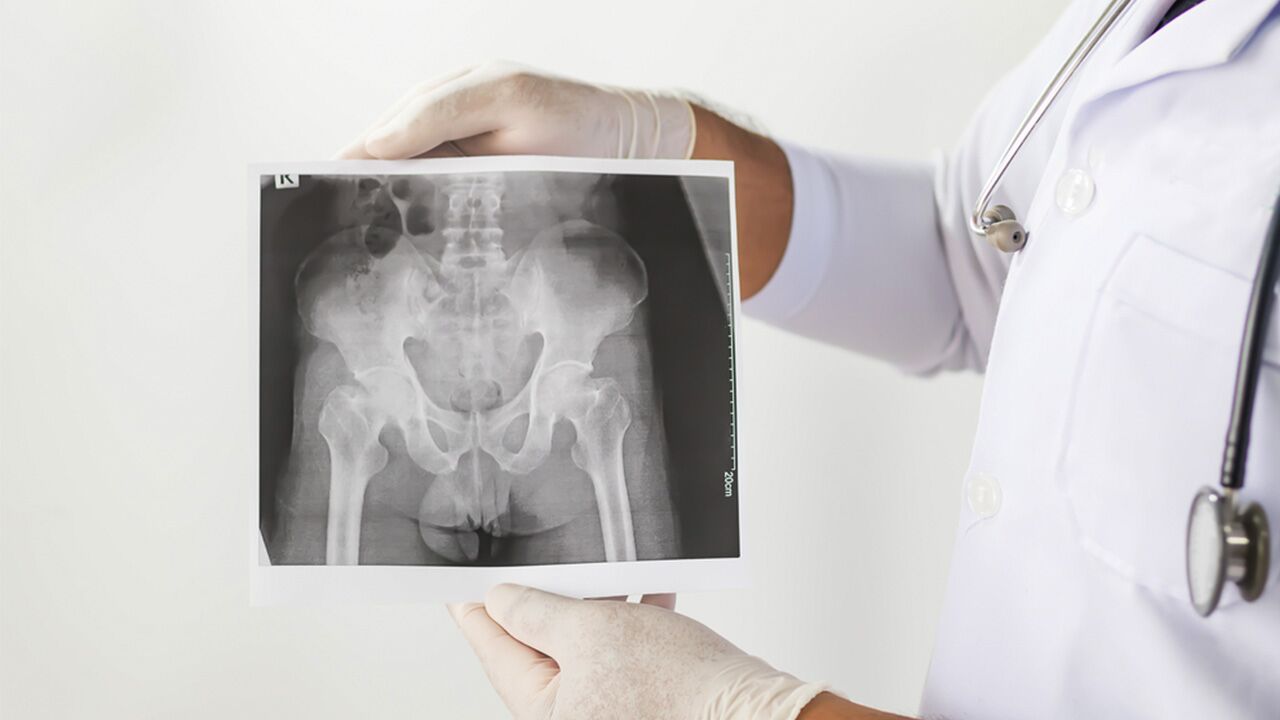
A healthy and strong spine is essential to your overall well-being, as it is the structure that holds you all together and allows you to do the activities you love. Arthritis comes in many forms and affects all parts of the body, but there is a certain type of arthritis that can affect the joints and bones within your spine. Ankylosing spondylitis (AS) is an inflammatory disease that can erode your spine or fuse parts of it, leading to loss of mobility. In advanced AS cases, this fusion can result in spinal deformity. We’ll take a closer look at this condition, the most common symptoms, who is typically affected, what causes AS, and the treatments available to help relieve the pain and stiffness associated with ankylosing spondylitis.
What Is Ankylosing Spondylitis?
Ankylosing spondylitis is a rheumatic disease under the umbrella of spondyloarthritis (or spondyloarthropathies).
Spondyloarthritis refers to a group of inflammatory rheumatological conditions that target the joints, including the spine.
Axial spondyloarthritis is a subgroup of spondyloarthritis that damages the axial joints, which are the spine, pelvis, and chest joints.
Moving further down the categorization tree, ankylosing spondylitis is a subgroup of axial spondyloarthritis, and it develops when parts of the spine and the sacroiliac joints become inflamed (a condition called sacroiliitis). Your sacroiliac joints are where your tailbone at the base of your low back meets the bones on either side of the upper buttocks of your pelvis.
When the inflammation becomes a chronic condition, you can experience pain and stiffness in and around your spine, including your neck, middle back, lower back, and buttocks. As time goes on, this inflammation of the spine (spondylitis) can lead to the development of new bone that causes a complete cementing together, or fusion, of the vertebrae (ankylosis). Ankylosis can lead to reduced range of motion and loss of mobility and flexibility of your spine.
Ankylosing spondylitis can also affect other tissues throughout your body, including joints besides the spine, as well as your organs, such as your lungs, kidneys, heart, and eyes.
What Causes Ankylosing Spondylitis?
The exact cause of this form of arthritis remains unclear, but the tendency to develop ankylosing spondylitis may have a genetic link that runs in families. Scientists have identified this genetic component and believe that people with AS carry the HLA-B27 gene. Your doctor may order a blood test as part of your diagnosis to see if you are HLA-B27 positive.
Researchers continue to investigate how and why inflammation occurs in different joints and organs in someone with ankylosing spondylitis. The illness appears in each person differently, and symptoms can vary greatly from patient to patient.
Your immune system may be activated due to an illness or environmental factor such as an infection that kicks inflammation into overdrive and sets the AS wheels in motion. In this case, your immune system is unable to switch off because it senses inflammation and continues to send out hormones and chemicals. If this persists for a long time and the inflammation becomes chronic, additional issues can arise and lead to AS and other autoimmune diseases.
What Are the Symptoms of Ankylosing Spondylitis?
Signs of ankylosing spondylitis include spine and joint inflammation, as well as inflammation in other areas of the body. If your back is the main focus of inflammation and pain, there is a probable chance you have AS. Your doctor will discuss other common symptoms to help identify the exact cause of your condition.
AS symptoms include:
- Pain that does not improve with rest
- Pain that disturbs your sleep
- Back pain (not caused by injury) that starts gradually before the age of 40
- Symptoms that continue 3 months or more
- Spinal stiffness in the mornings, which improves with exercise and motion
- Low-grade fever
- Loss of appetite
- Anemia
- Weight loss
- Fatigue
As AS begins to develop, you may notice pain and discomfort in your lower back, traveling down into your buttocks. You may also feel especially stiff upon getting out of bed in the morning and if you are sedentary for a length of time. AS can even affect parts of your feet, lower legs, and neck.
If your condition persists and turns into a chronic condition, the inflammation affecting your bones can cause ankylosis, which, as previously mentioned, is when parts of your spine begin to fuse together. Unfortunately, once this begins you start to lose flexibility and strength within your spine and movement and activities become very difficult. If allowed to progress, your upper torso can begin to curve, which is not only painful but can also affect your breathing capacity.
If AS is affecting your eyes, you may notice redness and pain or possibly experience vision issues such as uveitis/iritis, or eye inflammation, or digestive distress that could progress to inflammatory bowel disease. With the inflammation caused by AS, your risk for heart disease can increase. Symptoms include dizziness, difficulty breathing, and chest pain because parts of your heart and surrounding valves may be inflamed, making it difficult to pump blood properly.

Risk Factors for Ankylosing Spondylitis
According to the latest estimates from the Centers for Disease Control and Prevention's National Health and Nutrition Examination Survey (NHANES) program, AS and related conditions affect 2.7 million Americans.
Ankylosing spondylitis can afflict either gender, but men more commonly suffer from AS. For women, other joints in the body besides the spine are typically affected. AS is seen in all ages, including children, but the most common age of onset is 20s-30s.
Ankylosing Spondylitis Diagnosis
If you are experiencing any signs of AS, your health care provider will discuss your family history, medical history, and symptoms, conduct a physical examination, and order any necessary tests during your appointment. No blood test can confirm AS, but certain tests can help determine a diagnosis and eliminate other causes. In addition to a blood test to check for the presence of the HLA-B27 gene, your doctor may order a blood test called the erythrocyte sedimentation rate to check for inflammation.
You may also be tested for other conditions to rule out inflammatory diseases like rheumatoid arthritis, enthesitis-related idiopathic juvenile arthritis, and psoriatic arthritis that present with similar symptoms. Imaging tests, including X-rays and an MRI, can take a closer look at any changes in your spine and pelvis and identify fractures, inflammation, or other issues.
Treatment Options for Ankylosing Spondylitis
AS is not curable and the damage is unfortunately irreversible, but on a positive note, there are treatments that can help alleviate symptoms, manage progression, and maintain movement and posture. Options include physical therapy, exercises, and medications that reduce inflammation and pain. In rare cases, surgery may be necessary to correct a severe deformity.
If you are diagnosed with AS, you will routinely see a rheumatologist, since he or she specializes in inflammatory diseases and can help create a treatment plan that works for you. You will also likely meet with a range of specialists, including physical therapists, eye specialists, and gastroenterologists since AS can affect the whole body.
To ease your pain and inflammation due to AS, your doctor may prescribe nonsteroidal anti-inflammatory drugs (NSAIDs) such as:
- Ibuprofen
- Diclofenac
- Naproxen
- Indomethacin
- Meloxicam (Mobic)
- Celecoxib (Celebrex)
Other options include taking codeine and acetaminophen, especially if NSAIDs do not work for you, or directly injecting medication into the affected site.
Symptoms of AS, such as swelling, pain, and stiffness, can also be alleviated with anti-inflammatory disease-modifying antirheumatic drugs called (DMARDs). Methotrexate is a DMARD that can be administered in pill or shot form, while sulfasalazine is available in pill form.
DMARDs do, however, come with side effects that range from mild, such as bloating and mouth sores, to severe, such as liver damage. Folic acid supplements can help protect against milder side effects like nausea.
If symptoms aren't responding to NSAIDs or DMARDS, your doctor may prescribe biologics that inhibit tumor necrosis factor (TNF) , such as infliximab (Remicade), adalimumab (Humira), golimumab (Simponi), and etanercept (Enbrel). These TNF blockers act on your immune system to reduce inflammation and its associated side affects, as well as helping to mitigate further damage to the spine and other joints. Biologics have been linked to a greater risk of infections and cancer, although instances are rare.
Physical Therapy Exercises
Physical therapy and at-home exercises can help alleviate your symptoms and slow the progression of AS. Many patients work with a physical therapist to help maintain mobility, flexibility, and strength of surrounding muscles and joints.
A couple exercises you can practice daily if you suffer from ankylosing spondylitis include:
- While standing with your back against a wall, heels flush, push your head back so it is straight against the wall. Do not tilt your head back. Hold for 5 seconds, take a break and relax your head, then repeat up to 10 times.
- With your feet spread and hands on hips, stand up straight. Turn to one side, keeping your hands on your hips, hold for 5 seconds, relax, and then turn to the other side. Repeat 5 times on each side.
Diet and Supplements
Following a well-balanced diet is important when living with AS and trying to minimize the pain and discomfort brought on by the condition. Include nutrition-rich foods with your meals to reap as many body-nourishing, inflammation-fighting benefits as possible. Suggested dietary supplements include the following.
Omega-3 Fatty Acids
Helpful at reducing inflammation, particularly in your joints, these fatty acids are important for many bodily functions. Fatty acids are found in foods such as salmon and tuna, flax and chia seeds, walnuts, soybeans, and also in supplement form.
Calcium and Vitamin D
Healthy bones need calcium alongside vitamin D to help your body effectively absorb the calcium it requires to build strength. If you have AS, these vitamins can help increase bone density, leaving bones less susceptible to breaks and fractures. Since AS often affects your spine, not having enough calcium and vitamin D can leave it more brittle and subject to injury.
Foods rich in calcium and vitamin D include dairy products, spinach, okra, orange juice, soy milk, and egg yolks. You can also find calcium and vitamin D in supplement form.
Glucosamine and Chondroitin
Used to build cartilage, glucosamine and chondroitin sulfate can help supplement the loss that occurs from the joint-wearing effects of AS. Since AS causes the body’s immune system to attack the joints, taking supplements that support joint health can be very beneficial. Glucosamine can lower inflammation, reduce joint pain and tenderness, protect and repair gut lining, and help rebuild tissue and stronger bones.
Amino Acids
Known as our body’s building blocks, amino acids play a vital role in nearly everything that happens within our bodies. They are also very important for someone with an inflammatory disease such as ankylosing spondylitis.
- The amino acid methionine can help relieve pain, reduce inflammation, and boost the development of cartilage.
- Another beneficial amino acid is arginine, which helps develop bone strength and collagen production. Collagen is a protein that brings shape and structure to your connective tissues, skin, bones, and organs.
- Histidine also plays a vital role in maintaining joint health and provides potent anti-inflammatory benefits to reduce swelling in and around your joints.
- The amino acid lysine helps your body absorb calcium, which preserves your bone density and strength. If you take an amino acid supplement containing lysine along with your calcium supplement, your calcium absorption is given a greater boost. In addition, lysine works in tandem with vitamin D to build and nourish strong bones.
It’s preferable to take a complete amino acid supplement that provides the essential building blocks for enzymes, neurotransmitters, and hormones and is specially formulated to deliver a broad array of amino acids in optimal balance and form.
Ankylosing Spondylitis Outlook
How AS progresses in one person differs greatly from another. Sometimes symptoms appear and disappear, then return at a later time. Your doctor will better identify your prognosis based on how well your spine moves, the severity of inflammation, and if other areas of your body are affected. A few people can experience complications that damage the heart, digestive system, and lungs.
Overall, maintaining a healthy lifestyle, weight, and exercise program can help lessen AS symptoms and improve your day-to-day life and general well-being. If you or a loved one has ankylosing spondylitis, visit the Spondylitis Association of America website for additional educational resources and support.

Up to 25% off Amino
Shop NowTAGS: conditions
Join the Community
Comments (0)
Most Craveable Recipes



 833-264-6620
833-264-6620



















