How to Spot Measles Symptoms, Plus Understanding the Cause, Treatment and Prevention
 By: by Amino Science
By: by Amino Science
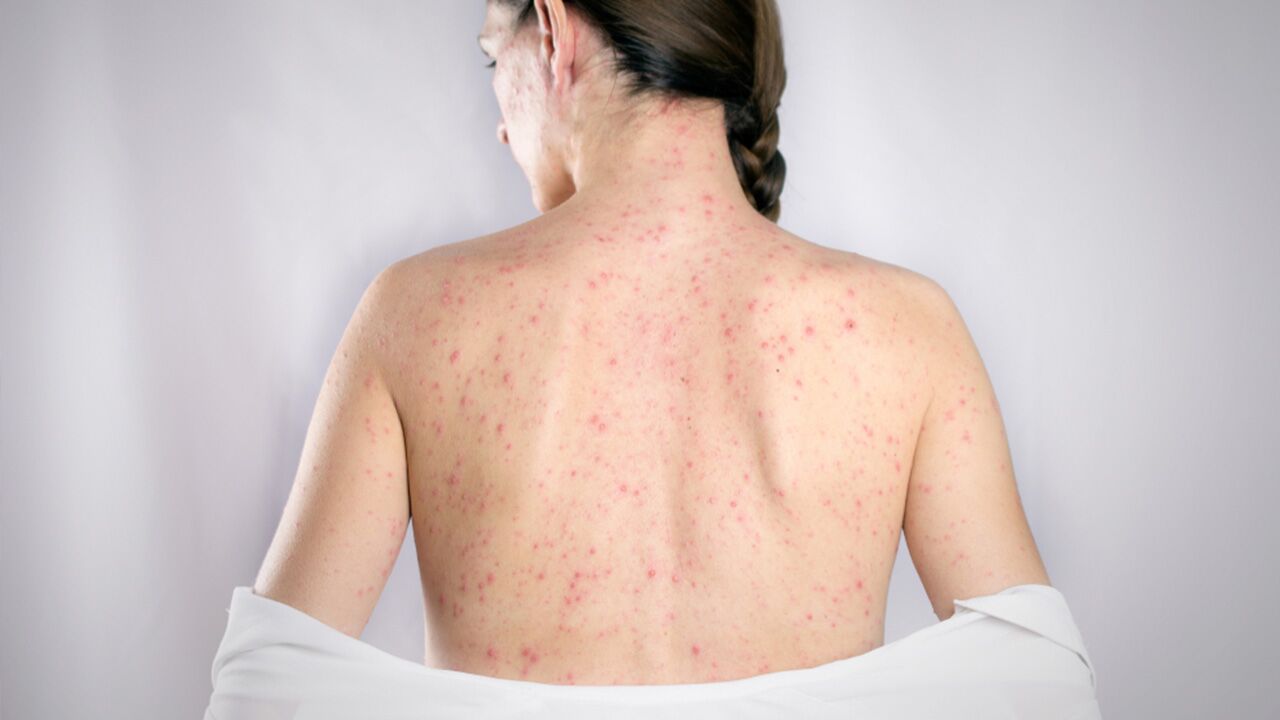
Prior to 1963, when the first measles vaccine was invented, it’s estimated that 3 to 4 million Americans were infected with the disease each year, and almost every child in the United States contracted the illness before 15 years of age. Hundreds of people with documented cases of measles died, and thousands suffered complications. However, a combination of vaccination and better control proved to be so effective that the virus was finally declared eliminated in 2000—a trend that has unfortunately begun to reverse itself, as 2019 has already seen the highest outbreak of measles cases in the United States since the virus was declared eradicated. Moreover, the Centers for Disease Control and Prevention (CDC) reports that approximately 110,000 people died globally in 2017 as a result of the disease, most of whom were children under 5 years of age.
So measles may be less common than it once was, but it certainly hasn’t disappeared. Therefore, in this article, we’re going to take a look at measles symptoms and investigate what causes this serious illness and what can be done to treat it and, most importantly, prevent it from happening in the first place.
What Causes Measles?
Measles, also known as rubeola, is an infectious disease caused by a virus belonging to the genus Morbillivirus. The measles virus replicates inside the nose and throat of an infected person and is spread via contaminated droplets in sneezes and coughs.
Measles is an incredibly contagious disease, infecting up to 90% of people who come in contact with it and are not already immune. The virus can also survive in the air and on surfaces for up to 2 hours, during which time it may be spread when a nonimmunized individual breathes infected droplets in the air or touches a contaminated surface and then puts their fingers in their eyes, nose, or mouth.
In addition, an infected person can transmit the virus from 4 days prior to the onset of the skin rash to 4 days after the rash appears.
Measles Risk Factors
While anyone can contract measles, certain people have a higher risk of getting the illness. Risk factors that increase your chances of measles include:
- Age: Children under 5 years of age and adults over the age of 20 are most at risk of contracting measles.
- Compromised immune system: People with weakened immune systems have a higher risk of getting sick. You can keep your immune system strong with supplemental amino acids.
- Pregnancy: Women who are pregnant are more at risk of contracting the disease.
- Lack of immunization: People who haven’t received a measles vaccination are most at risk of measles.
- International travel: People who’ve traveled to countries where vaccination is uncommon have a greater risk of becoming sick.
- Vitamin A deficiency: People who are deficient in vitamin A are at higher risk of complications related to measles infection.
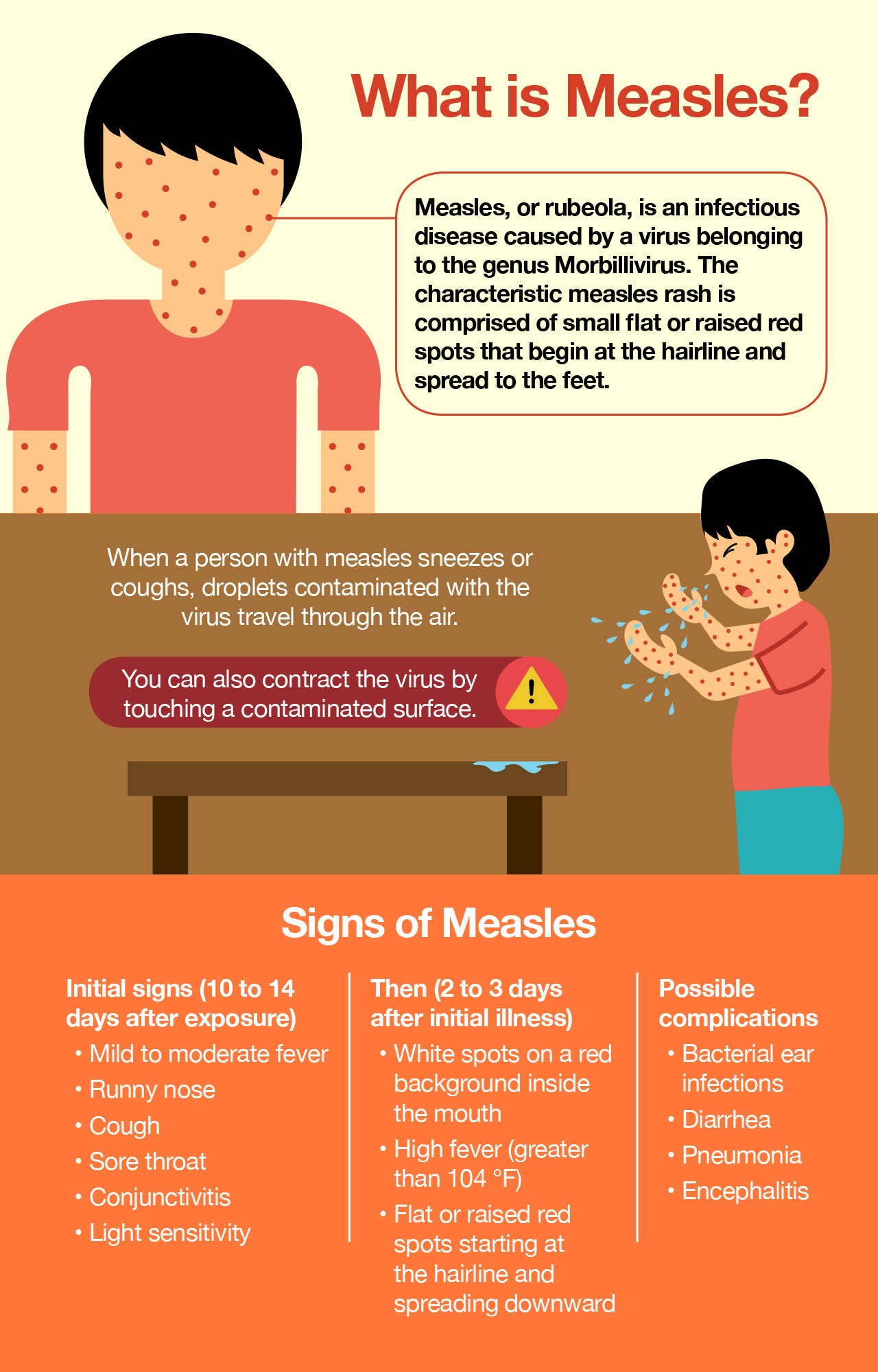
Measles Symptoms
If you’ve been exposed to measles, you can expect the virus to undergo an incubation period of approximately 10 to 14 days, after which the first signs of the illness will begin to appear.
The initial illness is usually relatively temperate and may include mild to moderate fever, runny nose, cough, sore throat, light sensitivity, and watery, red eyes (conjunctivitis, or pink eye).
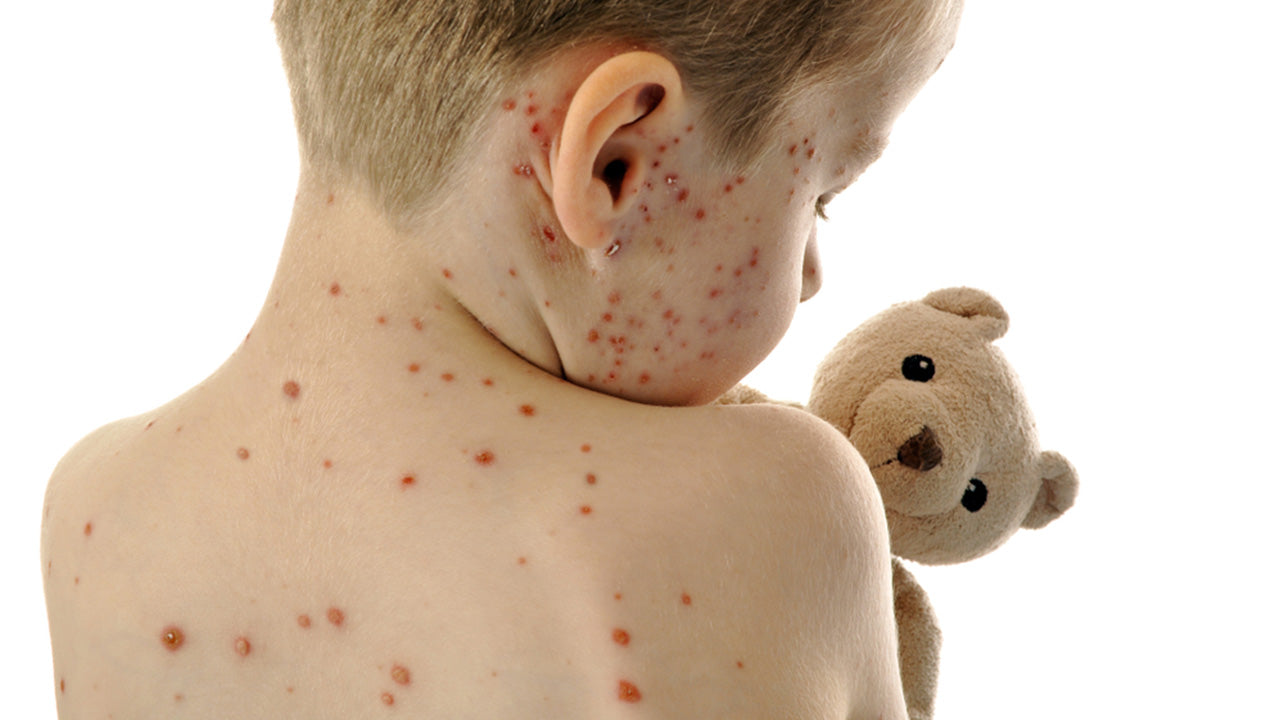
However, within two to three days of the initial illness, symptoms of measles begin to progress to include white spots with bluish-white centers (Koplik spots), seen on a red background inside the mouth, usually on the inner lining of the cheeks; small flat or raised red spots beginning at the hairline, spreading downward to the feet, and sometimes coalescing; and high fever (greater than 104 °F).
Complications of Measles
While most people who develop measles don’t experience complications, children under the age of 5, adults over the age of 20, pregnant women, and people with compromised immune systems are at greater risk.
The two most commonly seen complications of measles are diarrhea and bacterial ear infections. However, infection with the virus that causes measles can sometimes lead to serious complications like pneumonia, inflammation of the brain (encephalitis), and a rare neurological disorder called subacute sclerosing panencephalitis.
Diagnosing and Treating Measles
If you or someone you care about has signs and symptoms of measles, your health care provider can usually confirm the diagnosis by the presence of Koplik spots and the characteristic measles rash.
However, measles is now rare enough that some health care professionals may confuse the skin rash with other conditions, in which case a blood test should be performed to verify the diagnosis.
Unfortunately, no specific treatment is currently available for confirmed measles infections. However, nonimmunized individuals most at risk of complications may be given the measles vaccine within 72 hours of exposure, which may prevent symptoms or reduce the severity of the illness.
In addition, people with weakened immune systems, infants, and women who are pregnant may be given immune serum globulin. If given within six days of exposure to the measles virus, these antibodies may prevent the disease or reduce symptom severity.
Because high fevers are a common symptom of measles, if you’ve been diagnosed with the illness, your health care provider will likely recommend over-the-counter fever reducers like acetaminophen or ibuprofen. And since vitamin A deficiency is associated with a higher risk of complications, a dose of vitamin A as large as 200,000 International Units may be recommended.
Finally, people diagnosed with measles may find some relief by implementing certain comfort measures, including drinking plenty of fluids, using a humidifier in the bedroom, and getting enough rest.
Measles Prevention
Because an infected person can transmit the measles virus from 4 days prior to the onset of the skin rash to 4 days after it appears, anyone diagnosed with measles should isolate themselves during this period. This means staying home from work or school and avoiding contact with people who haven’t been vaccinated, especially infants under 6 months of age.
And for people who haven’t been infected with the measles virus, the CDC states that the best way to prevent the illness is by getting the MMR vaccine (measles, mumps, and rubella). For children, this means receiving the first dose of the vaccine between the ages of 12 and 15 months and the second between 4 and 6 years of age.
Additionally, adults traveling to countries where measles is more common, as well as individuals in high-risk settings, like college students and hospital workers, should make sure they’ve had two doses of the measles vaccine at least 28 days apart.
Unfortunately, in recent years, because of fears that vaccination may lead to autism, many parents have opted not to have their children vaccinated. Because of this, the CDC states that cases of measles are on the rise, with transmission rates doubling in recent years.
Yet multiple studies have been unable to find a link between vaccination and the development of autism. In light of this, experts continue to urge parents to have their young children immunized in the hopes of slowing measles outbreaks attributed to pockets of unvaccinated people as well as cases coming into the country as a result of travel to areas of the world where measles is more common.
Even though measles is rarely fatal, it’s important to remember that the illness can sometimes lead to serious complications. So be sure to protect yourself and your loved ones by getting the measles vaccine. And if you believe you or someone you care about has already been exposed to the virus that causes measles, don’t hesitate to seek the medical advice of a health care professional right away.

Up to 25% off Amino
Shop NowTAGS: conditions
Join the Community
Comments (0)
Most Craveable Recipes


 833-264-6620
833-264-6620



















