Types of Arthritis: Causes, Symptoms, Testing and Treatment
 By: by Amino Science
By: by Amino Science

While arthritis often comes with age (as is the case with osteoarthritis), sometimes it can be caused by an autoimmune disorder or other disease-causing pathogens inside the body. Rheumatoid arthritis, for example, is the result of immune system dysfunction. It can attack a person early in life.
What is the immune system doing to cause arthritis? The immune system begins to produce antibodies to fight off what it perceives as disease. In doing so, it attacks the rubbery cushion around a person’s joints. This cushion is known as cartilage.
In more common types of arthritis such as osteoarthritis, cartilage simply becomes worn out due to normal wear and tear and aging.
In some cases, osteoarthritis and rheumatoid arthritis both can be present in the same joint. Athletes who have sustained injuries often deal with multiple forms of arthritis. Infection from an injury can complicate arthritis.
Just the thought of bone-on-bone can be painful to many. Bone-on-bone causes joints to swell and even become deformed. Often, people with arthritis lose mobility and suffer from greatly diminished quality of life. Sometimes surgery becomes necessary.
But there are ways to manage arthritis pain once you understand the different types of arthritis, of which there are more than 100. In this article, we cover the most common.
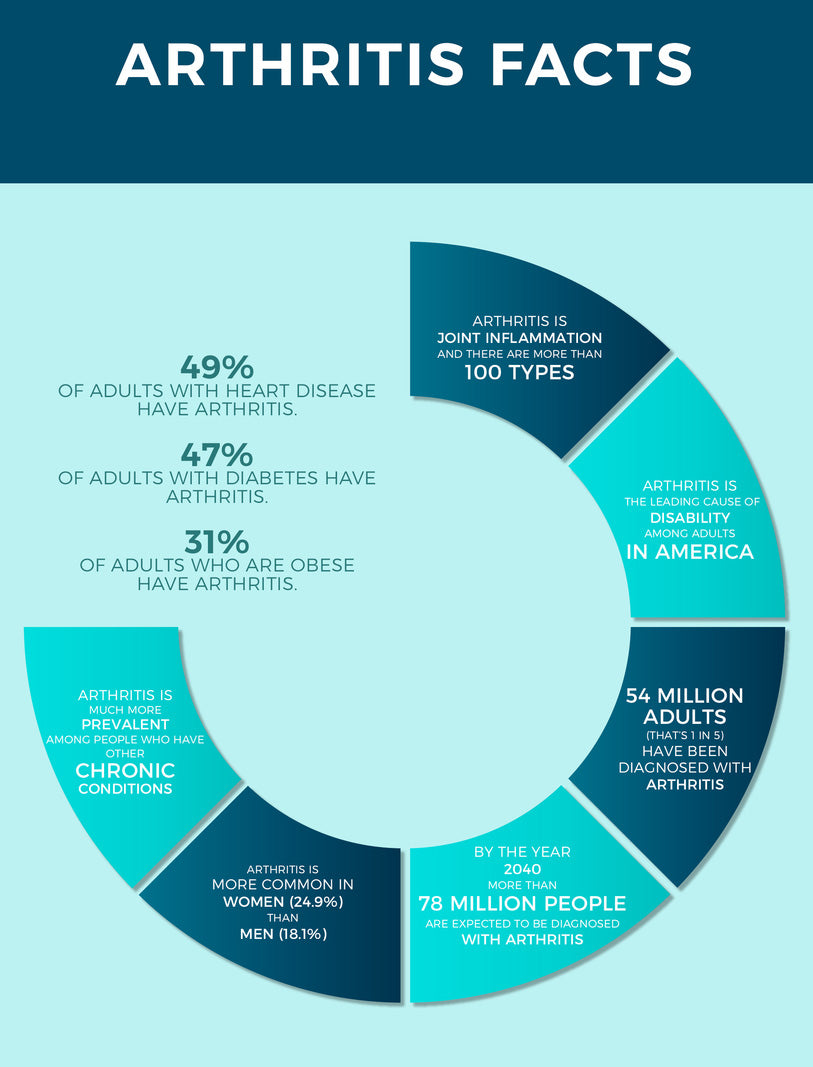
Osteoarthritis
Osteoarthritis affects almost 30 million Americans. It is the most common form of arthritis, occurring naturally in people as they age. Certain jobs also may result in people developing osteoarthritis in certain joints.
Osteoarthritis is the result of cartilage deteriorating through wear and tear. A world-class runner may develop osteoarthritis in the knees, for example. Any job or activity that involves doing the same thing over and over can result in wear and tear on cartilage that protects a specific joint or joints.
Testing and Treatment for Osteoarthritis
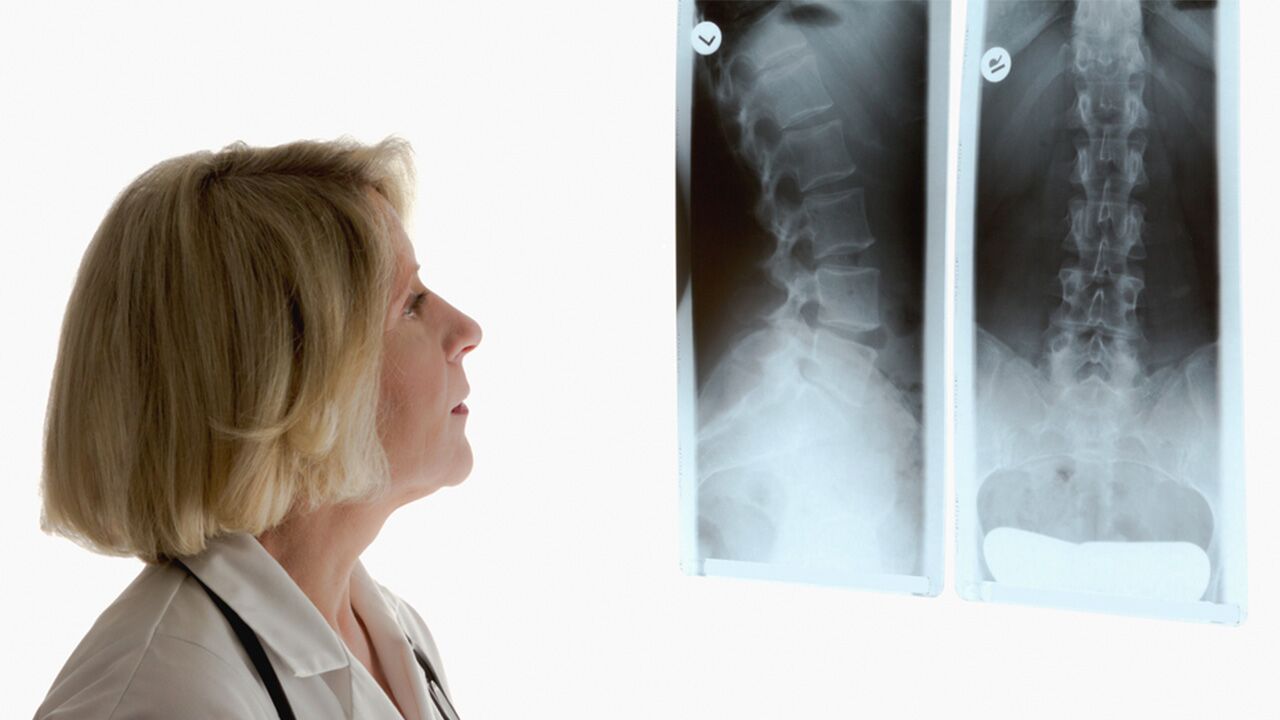
Pain and swelling in the joints, as well as decreased range of motion, make arthritis pretty easy to spot. Doctors can confirm a diagnosis with X-rays or, in rare circumstances, MRI scans.
Besides taking nonsteroidal anti-inflammatory drugs (NSAIDS such as aspirin and ibuprofen) to help combat joint inflammation, many people living active lives with arthritis use nutritional supplements. Glucosamine and chondroitin are especially popular (these are compounds that make up bone cartilage). Doctors and clinical studies disagree though on whether these compounds actually work. They have been determined safe and well tolerated.
A large, 2010 multi-site study called GAIT showed that people taking glucosamine and chondroitin alone or in combination with prescription medication fared about the same as those taking prescription medication alone. However, in the same study, people with knee pain specifically tended to fare a bit better on glucosamine and chondroitin than those without.
Fish oil supplements are a popular choice for people suffering from osteoarthritis. A 2010 meta-analysis “found that fish oil significantly decreased joint tenderness and stiffness in (rheumatoid arthritis) patients and reduced or eliminated NSAID use,”according to The Arthritis Foundation. “Preliminary studies indicate it may have a similar effect on osteoarthritis.”
Over-the-counter topicals and creams also provide fast and easy pain relief.
Inflammatory Arthritis
Rheumatoid arthritis and psoriatic arthritis are the most common types of arthritis caused by inflammation. In addition to autoimmune disorders and genetics playing a role, researchers believe “infectious agents, stress, cigarette smoke and hormones” may also contribute to symptoms.
Other types of inflammatory arthritis include juvenile arthritis, of which the most common type is juvenile idiopathic arthritis (JIA), and spondylarthropathies. All are discussed in more detail below.
The Arthritis Foundation stresses the importance of self-care for people who live with types of inflammatory arthritis.
“Self-management involves understanding and following the treatment prescribed by doctors and other health care providers,” the foundation explains on its website. “But it also involves making lifestyle choices and addressing both the physical and emotional effects of having a rheumatic disease like inflammatory arthritis. Self-management encompasses the choices made each day to live well and stay healthy.”
These choices may include the foods you eat, where you live and how much you exercise, and other best practices for wellness while living with a chronic condition.
Rheumatoid Arthritis
Rheumatoid arthritis (RA), like some other forms of arthritis, tends to target a specific gender. Three-fourths of the 1.3 million Americans with rheumatoid arthritis are women.
Unlike osteoarthritis, rheumatoid arthritis and other forms of arthritis caused by autoimmune disorders affect young people. Rheumatoid arthritis can begin at any age, but often women are around 40 at the onset.
Rheumatoid arthritis can be debilitating when not properly managed. This is the type of arthritis known for causing “stiff joints” in the morning. Some people have a very difficult time getting moving each day.
Rheumatoid arthritis tends to target multiple joints. Morning stiffness doesn’t go away after half an hour or so. Weight loss, fever, fatigue, and weakness also are symptoms of rheumatoid arthritis.
Scientists still don’t know why the immune system attacks healthy cartilage in people with rheumatoid arthritis. The damaging antibodies can cause long-term damage, but treatment options have come a long way.
Rheumatoid arthritis actually can be coaxed into “remission,”according to the American College of Rheumatology. “No single treatment works for all patients. Many people with RA must change their treatment at least once during their lifetime.”
Damage caused by arthritis is irreversible, and there is no cure, so it’s important to catch chronic conditions like rheumatoid arthritis early.
Testing and Treatment for Rheumatoid Arthritis
Doctors can check you for rheumatoid arthritis by taking blood tests or X-rays, though X-rays do not always catch early rheumatoid arthritis. They look for anemia, a “rheumatoid factor” or antibody, protein, or other biomarker (clues in your blood that show you have the disease).
Expensive treatments known as “biologics” have been created to treat debilitating forms of arthritis not caused by normal wear and tear. These revolutionary new medications actually are proteins that are made from genes. This genetic material convinces the immune system to leave your healthy cartilage alone and to stop creating painful and damaging inflammation.
A class of drugs known as DMARDs (disease-modifying anti-rheumatic drugs) also can be used. These are given by pill or by injection into a muscle. These drugs reduce pain and help prevent joint damage.
For people who suffer from rheumatoid arthritis, it is important to understand signs of a flare-up. Over time, patients learn what foods or activities aggravate their disease and cause a flare-up.
Carefully choosing which foods you eat when living with a chronic condition like rheumatoid arthritis is essential. Making healthy lifestyle choices, keeping stress to a minimum, and getting plenty of sleep also is important.
Psoriatic Arthritis
Psoriatic arthritis is characterized by painful swelling of the joints in the hands and feet. It often follows an outbreak of psoriasis, a skin condition. Enthesitis occurs when the connective tissue where ligaments and tendons connect to bones become inflamed, and typically accompanies psoriatic arthritis, as well as ankylosing spondylitis and juvenile idiopathic arthritis.
Until the beginning of the new millennium, few therapies existed for people suffering from psoriatic arthritis. That has changed with the development of biologics.
Testing and Treatment for Psoriatic Arthritis
“Early diagnosis is important, since people who present late do not fare as well,” Italian researchers wrote in the journal F1000 Research. “There are a number of clinical, laboratory, and ultrasound features that can help identify patients destined to develop (psoriatic arthritis), and several screening tools have been developed.
“It is recognized that genetic and epigenetic factors, as well as T cells and cytokines, play a role in the pathogenesis of (psoriatic arthritis), and several targets have been identified for therapeutic interventions.”
It also is important to keep conditions that can exacerbate psoriatic arthritis at bay. These conditions include obesity, diabetes, depression, osteoporosis, and many others. These comorbid conditions often can be managed effectively with diet and exercise.
“The expectation is that, in the future, (psoriatic arthritis) patients will be treated early and more aggressively and that there will not be significant progression of joint damage,” the researchers reported.
Systemic lupus erythematosus
Lupus is a chronic inflammatory disease that occurs when your body mistakes its own tissues and organs as invaders and begins attacking them. This autoimmune disease causes pain, fatigue, skin rashes, inflammation and its associated redness and swelling, and can severely harm internal organs including the lungs, heart, joints, kidneys, and nervous system.
Testing and Treatment for Lupus
Because lupus mimics the symptoms of several other chronic illnesses, it can be difficult to diagnose. Your health care provider will likely order a combination of blood and urine tests, as well as imaging tests and possibly a biopsy.
The most common medications used to treat lupus include:
- NSAIDs
- Antimalarial drugs
- Corticosteroids
- Immunosuppressants
- Biologics
Gout
Gout is a type of inflammatory arthritis that occurs when uric acid crystals build up in the synovial tissues, such as the hands, feet, big toe, or elbows. It's characterized by a sudden, sharp pain in the affected joint that can decrease mobility and accompany redness and swelling. Left untreated, gout can have serious ramifications on your lungs and kidneys.
Testing and Treatment for Gout
Apart from conducting a medical exam and history intake, the doctor will test your uric acid levels with a blood test. X-rays and MRI scans can check for bone, joint, and tissue damage, which will determine treatment protocol.
The aim of treatment is to reduce uric acid levels with medications such as colchicine and allopurniol, and to reduce inflammation with anti-inflammatory over-the-counter or prescription drugs.
To help prevent future gout attacks, reduce consumption of foods high in purine, such as red meat, organ meat, seafood, and alcohol.
Spondylarthropathies
Think of spondyloarthritis as “spider arthritis.” It may be a fitting reminder because like a spider, spondyloarthritis is a bit menacing. It also has many ways of attacking the body. This rare form of arthritis usually affects young men and boys in their teens and twenties.
Spondyloarthritis comes in different forms, or spondylorarthopathies. The most common is ankylosing spondyloarthritis. This type is hereditary, and researchers have begun to map which genes are involved. HLA-B27 is one.
The geographic distribution of ankylosing spondylitis is distinct. You find it most often in Alaska, but also among Native Americans in the Western United States.
Many people who suffer from spondyloarthritis report low back pain. Some have problems with hands or feet. Ankylosing spondylitis is particularly brutal and can result in deformities. Bones are chiseled away, making movement of the shoulders and hips difficult. Ankylosing spondyloarthritis often results in the need for spinal fusion surgery or joint replacement.
Another form of spondyloarthritis, enteropathic, is associated with autoimmune diseases of the bowel.
Testing and Treatment for Spondyloarthritis
Tests exist to find known genes causing spondyloarthritis. However, presence of a gene does not mean a person will develop the disease.
X-rays and other tests can be used to determine if there are changes in the spine. An MRI can pick up more subtle nuances that could result in earlier detection.
Like other forms of arthritis caused by autoimmune disease, biologics often are used to treat spondyloarthritis when over-the-counter pain relievers don’t do the trick.
Juvenile Arthritis
Juvenile arthritis simply refers to arthritis in children. Children usually have arthritis because of autoimmune disorders.
It is important especially for children to remain active to stave off joint pain and inflammation. Children also need to be encouraged to stay active, so they can maintain lives that are as normal as possible.
Testing and Treatment for Juvenile Arthritis
Juvenile arthritis can be confirmed by blood tests and imaging scans. Treatments include the same medications as those available to adults, including DMARDs, biologics, NSAIDs, and corticosteroids.
In addition to the specific treatment recommendations for the different types of arthritis covered, physical therapy and physical activity can help reduce associated arthritis pain by strengthening joints, increasing mobility, reducing joint stiffness, and increasing range of motion. To find out how amino acids can help treat arthritis and its symptoms, read this article.

Up to 25% off Amino
Shop NowTAGS: conditions
Join the Community
Comments (0)
Most Craveable Recipes


 833-264-6620
833-264-6620



















