8 Causes of Ptosis and What You Can Do About It
 By: by Amino Science
By: by Amino Science
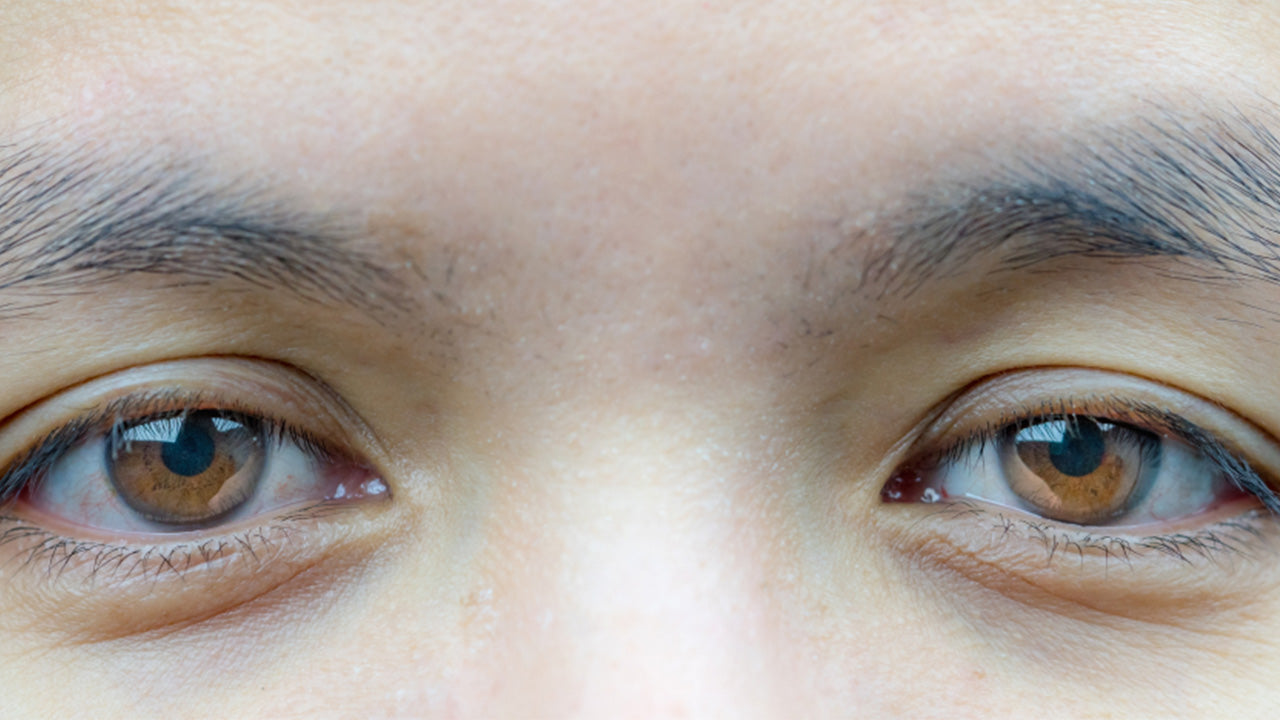
Ptosis is the term used to describe the condition in which one or both of your eyelids droop. While ptosis itself is not a disease, it can be caused by a number of underlying medical conditions, many of which are entirely treatable. So, if you’ve noticed a drooping eyelid or two, read on to learn about eight causes of ptosis and what you can do about it.
What Is Ptosis?
Ptosis, or pathologic droopy eyelid, can be the result of aging, injury, or a variety of medical conditions. But whatever its cause, you definitely know it when you see it because it results in a sagging eyelid that can make you appear tired or sleepy.
As mentioned earlier, ptosis can occur on one or both sides. When it occurs on only one side, it's referred to as unilateral, but when it occurs on both sides, it's referred to as bilateral.
Ptosis can also appear suddenly and then disappear, or the condition may never go away, especially if you’re born with it or develop it as you age. And if you have severe ptosis, your sagging eyelid may even cover your pupil, making it so difficult to see that you have to rely on your forehead muscles to lift your eyelid out of the way.
Causes of Ptosis
Of the different types of ptosis, the most common is aponeurotic. Also referred to as involutional ptosis, this form of the condition is a result of the levator palpebrae superioris, or elevating muscle of the upper eyelid, becoming overly stretched.
While most commonly seen in older adults as a natural part of the aging process, ptosis can also be caused by excessive eye rubbing or even longtime use of contact lenses.
In addition, eye surgeries, including cataract surgery, head injuries, and even diabetes may result in damage that leads to ptosis.

Ptosis may be the result of a surprising number of conditions. Some of these include:
- Horner syndrome
- Congenital ptosis
- Traumatic ptosis
- Aponeurotic ptosis
- Myopathy
- Diabetes
- Myasthenia gravis
- Cluster headaches
1. Horner Syndrome
Horner syndrome is a neurological disorder resulting from damage to the sympathetic nerves of the face. Along with a drooping eyelid, people suffering from Horner syndrome may present with decreased pupil size and decreased sweating on the affected side of the face.
Horner syndrome may be caused by a number of conditions, including lung cancer, stroke, brain or spinal cord injury, and carotid dissection.
2. Congenital Ptosis
Sometimes a child is born with a developmental problem involving the levator muscle of the upper eyelid. In approximately 70% of cases, the problem affects only one eye. However, if the ptosis is severe enough to obstruct the child’s vision, amblyopia or lazy eye can develop, and surgery is recommended to correct the problem.
3. Traumatic Ptosis
Traumatic ptosis occurs as a result of what’s known as levator disinsertion, which happens when the levator muscle is removed from its normal position. Risk factors for traumatic ptosis include surgery, chronic inflammation, excessive rubbing of the eye, chronic contact lens use, and physical trauma.
4. Aponeurotic Ptosis
Aponeurotic, or involutional, ptosis is the most common cause of ptosis in older adults. As we age, the effects of gravity and loss of muscle tone cause the levator palpebrae superioris to stretch, which causes the upper lid to droop.
5. Myopathy
Ptosis can also be seen with myopathies, or diseases of the muscles. One of these myopathies, a rare disorder known as oculopharyngeal muscular dystrophy, also affects eye motion.
Another condition called progressive external ophthalmoplegia is characterized by ptosis in both eyes and problems with eye movement due to muscle weakness.
6. Myasthenia Gravis
Myasthenia gravis is a chronic autoimmune neuromuscular disease that causes weakness in the skeletal muscles due to a breakdown in muscle and nerve communication. Interestingly, ptosis can be one of the first symptoms of this condition and may be seen in one or both eyes.
7. Diabetes
Over time, the elevated blood sugar levels that characterize diabetes can damage nerves. Sometimes the nerves that are damaged may include those that control the eye muscles. People with uncontrolled diabetes are at risk of developing ptosis due to this diabetes-related nerve damage.
8. Cluster Headaches
Cluster headaches are a type of severe, one-sided headache that occurs in cycles, or clusters. Unlike migraine headaches, cluster headaches vacillate between what’s known as cluster periods and remissions that can last months or even years.
Approximately 10% of cluster headache sufferers have been noted to exhibit a Horner-like syndrome, including ptosis on the symptomatic side.
How Is Ptosis Diagnosed?
An ophthalmologist is able to identify the specific cause of an individual’s ptosis based on their medical history and the results of an eye exam.
During the eye exam, overall eye health is assessed, with an emphasis on eye muscle function and the pupillary abnormalities sometimes seen in ptosis caused by nerve weakness.
If an underlying medical condition is suspected, blood tests, imaging, or a referral to a neurologist may be recommended.
Treatment Options
Once the type of ptosis has been determined, you and your health care provider will discuss your treatment options. If your vision is unaffected and the drooping doesn’t bother you, your doctor may recommend no treatment at all.
However, if your ptosis is making it difficult for you to see or you’re overly bothered by its appearance, your treatment will depend on whether the ptosis is a result of disease or simple levator weakness.
If an underlying medical condition is determined to be the cause, you’ll be referred to the appropriate specialist for treatment. Otherwise, surgery is generally considered your best treatment option.
Surgery
Unlike cosmetic surgery, ptosis surgery is generally performed by an oculoplastic surgeon—an ophthalmologist who specializes in plastic and reconstructive surgery.
The type of surgery chosen to correct ptosis is also determined based on the degree of weakness in the muscles around the eye. But the two most common types of ptosis surgery are levator resection and frontalis suspension.
If the levator muscle retains some of its function, a portion of it is removed, or resected, to shorten the muscle, thus making it tighter.
After this procedure is performed, your ability to blink will be affected as you get used to the tighter muscle, and eye drops or lubricating ointment may be needed to keep the eye from drying out.
If the levator muscle is very weak, shortening it won’t make it tight enough to raise the lid properly. In this case, a frontalis suspension will be performed.
To perform this procedure, small strands of either fibrous tissue from the leg (in children) or silicone (in adults) are placed between the eyelid and eyebrow and tightened.
After the surgery, it will then become the lifting and lowering of the eyebrow that opens and closes the eye.
Depending on how your eye heals after surgery, you may have to have later adjustments. If the position of your eye is noticeably too high or too low at your first follow-up visit, your incision can be reopened and the position adjusted. To help speed and optimize healing after ptosis surgery, use Heal, Amino Co's clinically proven surgical recovery blend.
However, if the tissue heals before an issue becomes apparent, a second surgery will be needed.
If you’re not a candidate for surgery or simply choose not to have it, you have another option as well. It’s an option that’s actually been around for decades, but we'd wager you’ve probably never heard of it.
Crutches
Crutches for ptosis? Believe it or not, there really is such a thing. In fact, ptosis crutches are devices that can be permanently attached to the frames of your glasses to hold your upper eyelid in place.
The most basic of these devices are really just wires attached to the rim of your glasses. They can also take some getting used to and may prevent you from closing your eyes all the way when you blink, so keeping your eyes lubricated is a must.
Magnetic crutches, or magnetic levator prostheses, are also now available. And according to a recent study, these new devices offer substantial advantages over traditional ptosis crutches, including easier eye closing.
As we've seen, ptosis is a relatively common condition, and while it may affect your appearance and ability to see clearly, it’s not in itself a major health concern. However, it’s important to remember that it may be an indication of a more serious underlying medical condition.
So, if your ptosis appeared suddenly or you’re experiencing any unexplained symptoms, be sure to discuss this with your health care provider. They’ll be able to find the root cause of your ptosis and guide you to the appropriate treatment options.

Up to 25% off Amino
Shop NowTAGS: anti-aging conditions
Join the Community
Comments (0)
Most Craveable Recipes



 833-264-6620
833-264-6620



















