Breast Ultrasound: Should It Replace My Annual Mammogram?
 By: by Amino Science
By: by Amino Science
Since the American Cancer Society first recommended mammograms in 1976, they have reigned as the primary test used for breast cancer screening. Millions of women receive an annual mammogram as part of a concentrated effort to increase early detection of breast cancer. Health care practitioners agree that early detection leads to better outcomes, in part because it allows for treatment using less invasive therapies. However, a healthy debate exists over the methods used for breast cancer screening as well as the optimal frequency of screenings. While mammograms remain the most commonly recommended option, interest in the use of breast ultrasound as a screening test continues to grow.
In this article, we'll discuss the differences between the two types of imaging tests to help you understand the benefits and drawbacks of each method.
What Is a Mammogram?
Most of us have heard the word mammogram before, and know that it's a breast cancer screening test. Unless you've had a mammogram yourself, however, you may not know exactly what the procedure entails.
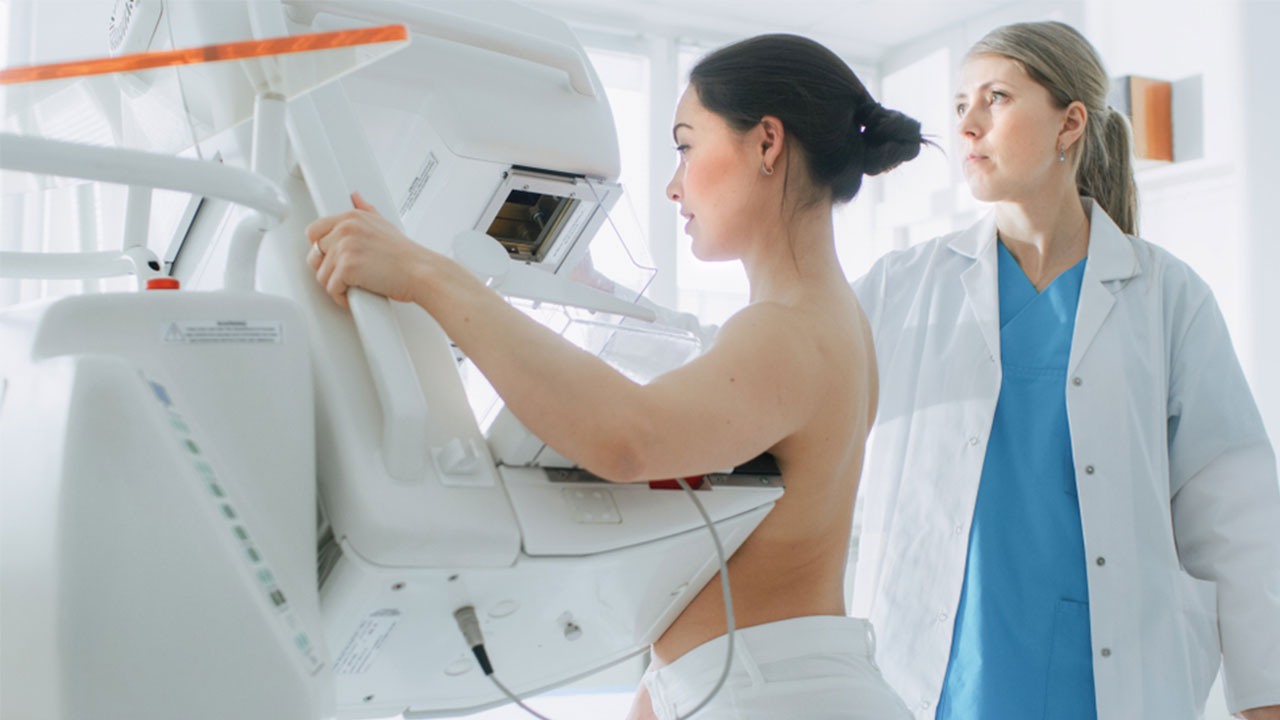
The simplest explanation of a mammogram is that it's a low-dose X-ray examination of the breasts. During a mammogram, you stand facing a special X-ray machine while a radiologic technician places each of your breasts in turn between an X-ray plate and a plastic plate. The X-ray machine then presses the plates together to flatten the breast, spreading out the tissue so a clearer image can be created when the X-ray is transmitted. The sensation is certainly not a comfortable one—many report feeling pinched or squeezed. However, this discomfort only lasts a few seconds.
Typically, two pictures will be taken of each breast, one from the side and one from above. The images—recorded either on X-ray film or on a computer—are called mammograms. A radiologist examines those images to look for changes in breast tissue that could indicate cancer. The whole mammogram process typically takes 20 minutes from the moment you enter the room until you leave.
Mammograms can be used as a part of routine screening for women who have no concerns about their breasts or for women worried about symptoms like changes to the size or shape of a breast, lumps that can be felt in breast tissue, nipple discharge, or pain. While many breast changes turn out to be benign, only a doctor can conclusively determine that.
According to the Office on Women's Health, a division of the U.S. Department of Health and Human Services, high-quality mammograms are "the most effective way to detect breast cancer early. Finding breast cancer early greatly improves a woman's chances for successful treatment."
The Limits of Mammograms
While mammograms are promoted by health institutions as the most effective method for early detection of breast cancer available at this time, they do have drawbacks.
The Office on Women's Health lists the following limitations for the efficacy and use of mammograms:
- False negatives: While this does not happen often, in some cases, mammogram images may indicate that all is well when cancer is actually present. According to the American Cancer Society, screening mammograms fail to find breast cancer in about 20% of all recorded cases. This is more common among younger women than older women, largely because of differences in breast tissue (more on that later).
- False positives: In certain instances, a mammogram result may make it appear that cancer is present when it is not. This can lead to unneeded worry and follow-up tests. Per the American Cancer Society, about 50% of women who receive annual mammograms over a 10-year period will receive at least one false positive. Having past mammogram results available for comparison dramatically decreases false positives, again, by around 50%. False positives happen at higher rates for young women, women who have had breast biopsies, women with family histories of breast cancer, and women taking estrogen.
- Exposure to radiation: As is true of dental X-rays and other routine X-rays, mammograms expose us to small doses of radiation. This carries a very low risk of harm, though the accumulation of repeated X-rays over the course of a lifetime may slightly elevate your risk of developing cancer. It's a good idea to speak with your doctor about the need for any type of X-ray, how to shield parts of your body not in the X-ray picture, and any possibility that you might be pregnant.
- Increased likelihood of unnecessary interventions: Because mammograms can detect small breast lumps, masses, and calcifications, they may alert you to the presence of changes in your breast tissue that do not yet require treatment or may never require treatment. However, once those changes have been spotted, many do feel the need to intervene.
How Breast Density and Breast Implants Influence Mammogram Results
There are two types of breast tissue: fatty breast tissue and dense breast tissue. Mammograms are highly reliable when it comes to detecting changes in fatty breast tissue, but less so when it comes to dense breast tissue.
Fatty breast tissue appears black or gray on a mammogram while cancerous masses or calcium buildups appear white. This makes it fairly easy for a radiologist to spot cancer in fatty breast tissue. Dense breast tissue, however, is much thicker than fatty breast tissue and appears white on a mammogram just like cancer does. As a result, a radiologist may miss cancerous masses that are surrounded by similar-looking dense breast tissue.
According to the Susan G. Komen Foundation, 40-50% of U.S. women ages 40-74 have dense breast tissue, and these women are 4 to 5 times more likely to get breast cancer than women with mostly fatty breast tissue. For these individuals, it can be extremely valuable to use other breast cancer screening tests instead of or in addition to mammograms.
Mammograms can also be less effective for those with breast implants. Individuals who had reconstructive surgery including implants after a mastectomy should consult their doctor about the necessity of mammograms. In most cases, mammograms are still considered the most effective breast cancer screening test for those with breast implants who have not had mastectomies.
If you have breast implants, you should mention this when scheduling a mammogram so you can be paired with a technician and radiologist experienced in X-raying patients with implants. The reason for this is that implants can hide some breast tissue, so the technician will need to gently lift the breast tissue away from the implant and create additional images.
General Guidelines for Mammograms
Different organizations offer varying guidelines for both the age at which routine mammogram screening should begin as well as the ideal frequency of screenings.
The latest guidelines issued by the United States Preventative Services Task Force (USPSTF) recommends that women between the ages of 50 and 74 schedule mammograms every 2 years. This recommendation mirrors those of most European countries, but differs from those of other U.S.-based organizations.
For instance, both the American College of Radiology as well as the Society of Breast Imaging currently advise that women should schedule annual mammograms beginning at the age of 40. Meanwhile, the American Cancer Society holds that women between 45 and 54 years of age should schedule annual mammograms, then space that out to a mammogram every 2 years from the age of 55 onward.
The goal behind the more conservative recommendations in terms of the age at which screening should begin as well as frequency of screening is to reduce the rate of false positives, which some evidence shows increases among younger women as well as women who receive annual screenings.
What Is Breast Ultrasound?
The American Cancer Society describes breast ultrasound as a useful method for examining some types of breast changes, particularly lumps that can be felt during a physical exam but not identified on a mammogram or changes in the breasts of women with dense breast tissue.
Breast ultrasound can also be an advantageous next step after a mammogram to gather more information about breast changes, since ultrasound can distinguish between fluid-filled cysts—which tend not to be cancerous—and solid masses—which usually require additional testing such as biopsies to determine whether or not they're cancerous.
Breast ultrasound uses high-frequency sound waves to create images of the interior of each breast. A trained ultrasound technician, typically a sonographer, first physically examines the breasts. If the purpose of the ultrasound is to gather more information about an identified change, such as a lump, they will also ask questions about when the change was first detected, whether you've noticed any other symptoms, and so on. Next, the sonographer will apply clear gel to the breast, which improves the ability of the high-frequency sound waves to move through the breast tissue, and gently move a wand-like device called a transducer over the breast.
As the sound waves emitted by the device bounce off body tissues, they create echoes that form ultrasound images on a computer screen in real time. A breast ultrasound typically lasts between 15 and 30 minutes, and while you will feel some pressure as the device moves across the surface of each breast, it will likely be painless unless your breasts themselves are tender at the time.
Because breast ultrasounds do not use radiation, they are the safest option for women who are not good candidates for screening tests that involve radiation, like mammograms. If you are pregnant or trying to become pregnant, for instance, you should avoid exposure to radiation.
Breast ultrasound can also be an advisable breast cancer screening measure for women with dense breast tissue. Because cancerous masses appear black on an ultrasound, as opposed to white on a mammogram, ultrasound can be a more reliable means of locating breast cancer in dense breast tissue.
The Limitations of Breast Ultrasound
Common consensus among health care providers at this time is that the limitations of breast ultrasound disqualify it as a screening test in most instances. Those limitations include:
- Limited imaging capacity: The hand-held devices typically used for breast ultrasounds cannot take a comprehensive image of the entire breast. They also cannot take images of areas deep inside the breast, so while they can be used to detect and evaluate superficial lumps, deeper abnormalities may be missed. Ultrasound images also fail to capture architectural distortions and asymmetries.
- Inaccurate diagnostic images: The increased specificity of ultrasound images which makes them advantageous as a screening tool for women with dense breast tissue also increases the likelihood that inaccurate diagnostic images will be produced. A great diversity exists both among ultrasound images of healthy breast tissue and pathological lesions, due to factors such as the age of the patient, hormone levels, and previous breast surgery, trauma, or radiotherapy. This can make it challenging to differentiate between benign variations and changes that indicate cancer.
- Inability to detect microcalcifications: Early detection of breast cancer often results from the discovery of microcalcifications, tiny deposits of calcium that commonly appear in the tissue surrounding a tumor. Microcalcifications do not register on breast ultrasound, meaning a diagnosis could be delayed.
- Impact of technician skill: The skill and experience of a sonographer can significantly impact the results. Human error can cause lesions to be overlooked or images to be misinterpreted.
- False positives and false negatives: While mammograms can also deliver false positives, this happens at a higher rate with ultrasounds when they are conducted along with mammograms. As discussed previously, a false positive can lead to more tests, including invasive breast biopsies. This can send health care costs and anxiety levels soaring. Ultrasounds can also turn up false negatives, though this is less of a concern.
When to Consider Automated Whole Breast Ultrasound
By this point, it has hopefully become clear that neither mammograms nor breast ultrasound using a hand-held transducer are foolproof. Automated whole breast ultrasound is an option that some believe can be more reliable.
Concerns about the dangers of inadequate breast cancer screenings led board-certified diagnostic radiologist Dr. Kevin Kelly of the Breast Ultrasound Center in Pasadena, California to patent SonoCine automated whole breast ultrasound in 1999. According to Dr. Kelly, automated whole breast ultrasound eliminates some of the disadvantages associated with conventional breast ultrasound screenings, such as the inability to create a comprehensive image of each breast and the errors introduced by sonographers.
Automated whole breast ultrasound slowly scans the entire breast, capturing images that include the underarm area, the lymph nodes, the sides of the breasts, and the areas above and below each breast. The procedure captures thousands of pictures of the breast that are then played back like a movie for the radiologist to review. As with traditional breast ultrasound screenings, automated whole breast ultrasound is typically recommended as a secondary screening measure for women with dense breast tissue or breast implants. Again, as with hand-held breast ultrasound screening, the procedure typically takes about 30 minutes to complete and, in the absence of breast tenderness, does not cause pain.
Dr. Kelly is an advocate of breast health education and wants women to understand their breast type, risk factors, and options when it comes to breast cancer screening and diagnostics. He has given a Tedx Talk in which he highlighted the dangers of inadequate breast cancer screenings and the importance of making ultrasound procedures like AWBUS the standard in care.
As of 2012, the FDA has approved the use of automated whole breast ultrasound as a secondary breast cancer screening test, but not as a replacement for an annual screening mammogram.

Breast Ultrasound vs. Mammogram: Which Is Best?
A study published in the Journal of the National Cancer Institute, a peer-reviewed journal that's internationally acclaimed as the source for the most up-to-date information from the fields of cancer research and treatment, directly compared the efficacy of breast ultrasounds and mammograms. The lead author, Dr. Wendie A. Berg, concluded that: "Where mammography is available, ultrasound should be seen as a supplemental test for women with dense breasts who do not meet high-risk criteria for screening MRI and for high-risk women with dense breasts who are unable to tolerate MRI."
Other experts agree. Sharon L. Koehler, an assistant professor of breast surgical oncology in the Department of Clinical Specialties at the New York Institute of Technology College of Osteopathic Medicine, believes mammography is the best primary screening test for most women, since the results are less dependent on the operator and the images show calcifications, architectural distortions, and asymmetries in addition to masses.
However, because hand-held ultrasounds are more portable and less expensive than the machines needed for mammograms, an emerging consensus among medical practitioners holds that they can be a crucial screening tool in developing countries. "As long as we are aware of ultrasound’s limitations, in countries where mammogram is not available, ultrasound is a good option," Dr. Lusi Tumyan, City of Hope assistant clinical professor and section chief of breast imaging in the Department of Radiology, said in an interview.
According to Dr. Kelly of the automated whole breast ultrasound, approximately 50% of American women have dense breast tissue, and 70% of all breast cancers occur in dense breasts. Dr. Kelly has stated that one of the biggest misconceptions currently surrounding breast cancer screenings is that mammograms are believed to be fully able to find cancer whenever it’s in the breast, but this is not necessarily true. Dr. Kelly has stated that 50% of cancers in dense breasts are felt before they’re seen on a mammogram. According to Dr. Kelly, mammograms work well, but unfortunately, they don’t work often.
Another common misconception about mammograms that Dr. Kelly has observed is the belief that mammograms usually find cancers when they’re small. But Dr. Kelly has stated that this is not true. The average size of breast cancer when it is detected by mammogram is 17 mm. The ideal size for treatment of cancer is between 5-10 mm. While mammograms often find cancer once it’s past the ideal treatment stage, the AWBUS can find 5 mm invasive breast cancer. The AWBUS is far more accurate in detecting breast cancer in women with dense breast tissue and implants, and in clinical trials was 300% more accurate than mammograms at detecting small invasive breast cancers. The earlier cancer is discovered, the more likely that it can be monitored and treated, eliminating extreme and traumatic treatments like chemotherapy and mastectomies and saving tens of thousands of lives in the U.S. every year.
However, Dr. Melanie Royce, an oncologist who specializes in breast cancer, finds it frustrating when people try to equate mammograms and breast ultrasound. "One is not better than the other, they are complementary" said Royce, the director of the breast cancer multidisciplinary team at the University of New Mexico Comprehensive Cancer Center. "They are complementary. They should be seen as such and used as such rather than one as a substitute for the other. At least this is the case where both are widely available."
At this time, neither breast ultrasound using a hand-held transducer nor automated whole breast ultrasound have been proven or approved as a substitute for a mammogram.
This means that while breast ultrasound may be covered by insurance, patients should be sure to verify that prior to scheduling an appointment. The out-of-pocket cost of a breast ultrasound ranges between $150-500 for an exam using a hand-held transducer and $160-400 for automated whole breast ultrasound. Routine screening of both breasts typically costs more than the use of ultrasound as a follow-up test to examine breast abnormalities in a particular area of concern.
An additional hurdle patients interested in automated whole breast ultrasound may encounter is availability. At this time, it's less common for facilities to use this technology. If you believe automated whole breast ultrasound could be the best screening test for you, it could be worthwhile to mention it to your primary care physician or OB-GYN.
It's important to note, too, that both mammograms and ultrasounds can only suggest the possibility of cancer. In order for a definitive diagnosis to be made, a biopsy that removes a tissue sample for examination under a microscope must be carried out.
Ultimately, experts agree that no single screening test can be declared superior for all women in all instances. The best option for patients would be to have a balanced discussion with a health care provider about their individual risk factors and the pros and cons of available screening technologies.
Experts also agree on the importance of eating a healthy balanced diet and protecting against chronic disease with nutritional therapies such as essential amino acids. For overall wellness support, try Life, Amino Co's Active Aging blend.

Up to 25% off Amino
Shop NowTAGS: conditions natural cures
Join the Community
Comments (0)
Most Craveable Recipes




 833-264-6620
833-264-6620



















