Eczema Remedies: The Causes, Symptoms and Best Treatments for Skin Relief
 By: by Amino Science
By: by Amino Science
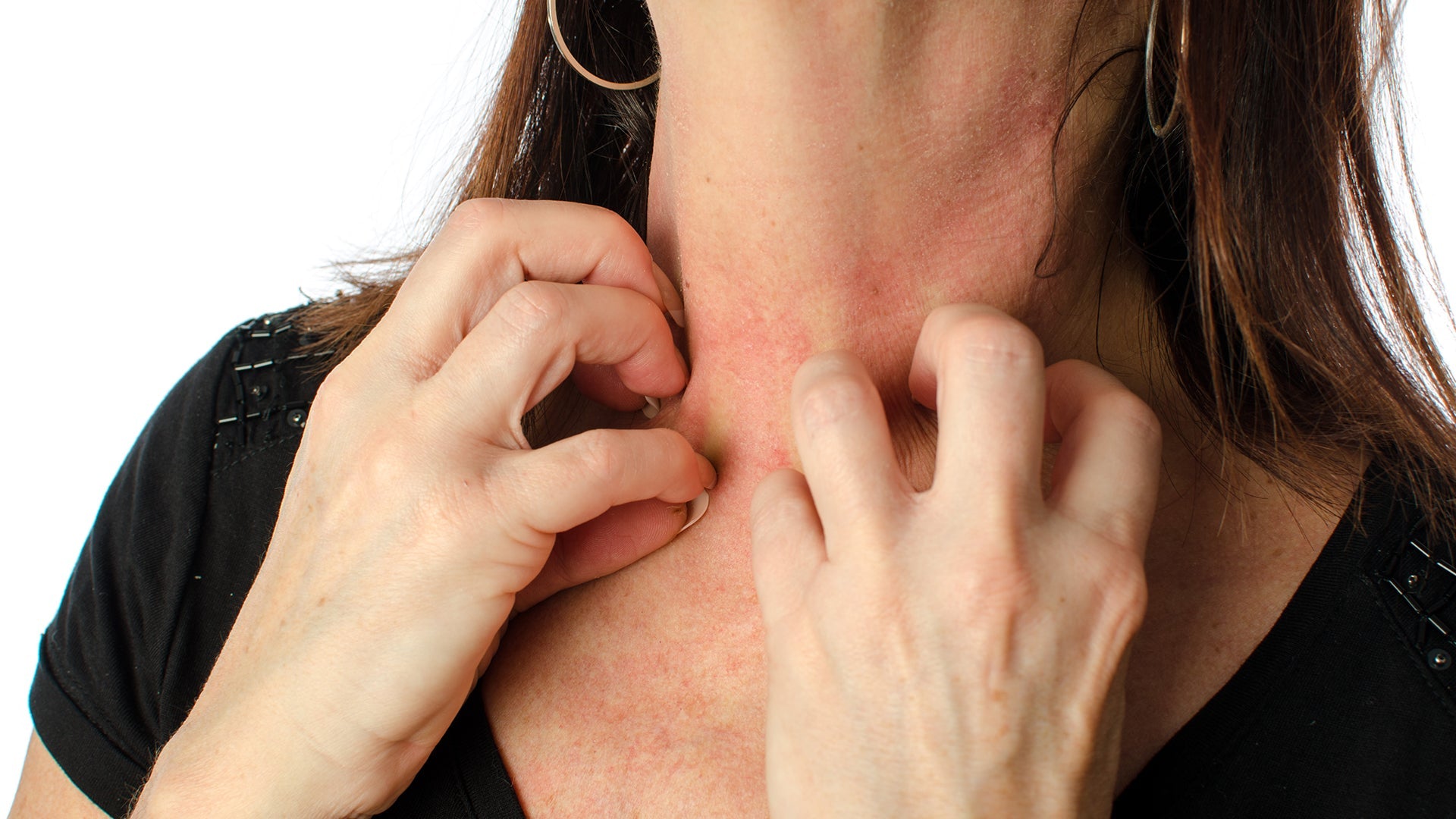
More than 30 million Americans have some form of eczema, a skin condition characterized by inflamed, red, itchy skin. Often used as an umbrella term to define a group of chronic, itchy skin rashes, eczema varies in appearance depending on the type of rash and its location. In some forms of eczema, blisters may also develop. Eczema symptoms can be intense for a period of time, calm down, and then surface again. Scratching can inflame the rash, and a clear fluid may ooze out of the affected area. In this article, we’re covering the types, the causes, the symptoms, and the eczema remedies for skin relief.
Types of Eczema
The National Eczema Association divides eczema into six types, based on their possible causes.
Atopic Dermatitis
The most common form of eczema, atopic eczema usually affects children by age 5, but adults may develop it as well. It shows up as dry, red, and itchy patches of skin usually on the face, scalp, hands, feet, inside the elbows, and behind the knees. Babies tend to develop a red rash on their cheeks and scalp. In severe eczema cases, patches may crack and become infected.
Atopic dermatitis is recurrent—it lasts for a period of time, then it goes into remission and comes back again. This type of eczema can be a lifelong condition, but in some cases, children might see improvements as they age.
Contact Dermatitis
Contact dermatitis strikes when the skin comes into contact with an allergen or irritant that sparks swelling, itchiness, redness, and a burning sensation. Blisters can ooze and crust over.
Irritant contact dermatitis occurs when in contact with everyday items such as soap, cosmetics, and wind, and typically emerges on the hands and face. Allergic contact dermatitis is rarer, and results from continual exposure to a chemical, such as in a work environment or from perfumes in toiletries. Both irritant contact dermatitis and allergic contact dermatitis can cause what's commonly called hand eczema in which scaly, dry, and itchy skin afflicts the hands.
Dyshidrotic Eczema
This type of eczema presents as itchy, fluid-filled blisters that develop under the skin on the hands or the feet. Over time, the affected patches can crack, exposing the skin to painful infection. Stress and other habits, such as frequent or long periods of contact with water and working with certain metals can aggravate or trigger an eczema flare. Dyshidrotic eczema is more common in women, and it usually occurs in spring and summer and in warmer climates.
Nummular Eczema
People with nummular eczema, or discoid eczema, have round or oval itchy and inflamed, swollen patches of skin, formed by pimples that become scaly. This type of eczema usually affects the torso, arms and legs, and it is more common in older men, but all ages and genders are susceptible. People with dry skin may be at risk of developing nummular eczema, especially in winter, and insect bites are a common cause.
Seborrheic Dermatitis
This chronic form of eczema afflicts areas of the body that contain many oil-producing glands, such as on the scalp—where it shows up as dandruff—or on the nose or upper back where it can manifest as yellow scales of reddened skin. Seborrheic dermatitis can be exacerbated by microorganisms like yeast, but isn't caused by an allergy, unlike other types of eczema.
Men have a higher likelihood of developing seborrheic dermatitis than women do, and in infants it's known as "cradle crap." Those suffering from medical conditions that compromise the immune system, such as HIV or AIDs, or the nervous system also have a greater tendency towards developing seborrheic dermatitis.
Stasis Dermatitis
Also referred to as gravitational dermatitis, venous eczema, and venous stasis dermatitis, stasis dermatitis arises when blood flow is impaired and pressure builds up, particularly in the lower legs. The buildup pushes fluid out of the veins and into the skin, resulting in symptoms of eczema such as:
- Ankle swelling
- Pain
- Redness
- Scaly skin
- Itching
- Oozing
- Cracking skin
- Infection

Eczema Causes
The specific cause of this inflammatory condition is unknown, but experts believe that eczema is related to a variation in genes that affects the skin’s ability to protect the body from bacteria. This lack of protection leaves the skin exposed to environmental factors, irritants, and allergens that can cause inflammation. In some children, food allergies may instigate eczema. Having a close relative with eczema can also be a risk factor.
Common causes of eczema flare-ups include:
- Wool
- Sweat
- Soaps
- Dust
- Laundry detergents
- Cough, cold, flu
- Contact with pet saliva
Eczema Remedies for Skin Relief
Before resorting to medications, you can try lifestyle and home remedies to prevent flares and reduce symptoms. Eczema can be persistent, and you might need to try different natural remedies to see results—but don’t get discouraged. Follow these tips for skin relief.
Moisturization
Keep your skin moisturized—choose a product that works well for you and is free of chemicals or allergens that can worsen your eczema. Apply the moisturizer at least twice a day, and after bathing while the skin is still damp.
Coconut Oil
Coconut oil is a celebrated microbial and eczema treatment that can help to decrease staph bacteria and your risk of skin infections. Replete with beneficial fatty acids, coconut oil is a supreme skin and hair moisturizer. All it takes is a twice daily application of virgin coconut oil to damp skin.
Essential Oils
Essential oils, especially lavender essential oil, can help with mood and sleep management for eczema patients, as well as heal eczema symptoms. Dilute 10 drops of lavender essential oil in 2 tablespoons of coconut oil and gently apply to skin. To promote restful sleep, diffuse lavender essential oil and chamomile essential oil in an aromatherapy diffuser and breathe in the tonic as you sleep.
Take Warm Baths
A warm bath can do wonders for healing inflamed and sensitive skin. Limit baths and showers to 10 to 15 minutes. Add a sprinkle of baking soda or uncooked oatmeal to the bath water—soak and then dry gently.
In addition to oatmeal baths, you can soak in a bleach bath for 10 minutes to reduce the bacteria on the skin. Dilute a 1/2 cup of household bleach in a 40-gallon bathtub filled with warm water. Don't use concentrated bleach and never submerge the head.
Mild Soaps
Use soaps without dyes or perfumes to avoid substances that may irritate your skin. Superfatted and non-alkaline soaps are top choices.
No Scratching
Cover the itchy area if you can’t avoid scratching it. Using bandages helps protect the skin and prevents scratching.
Smooth Clothing
Avoid rough, tight, and scratchy clothing such as wool. Also, wear clothing that can help the skin breathe in hot weather or during exercise to prevent excessive sweating.
Humidifier
Hot, dry indoor air can make the itching worse. A humidifier can help add moisture to the air inside your home to help ease the itching associated with eczema.
Manage stress
Stress and anxiety can make symptoms worse. Consider using breathing techniques and meditation to reduce stress, as well as making appropriate lifestyle changes, such as adding more anti-inflammatory foods and fruits and vegetables to your diet, getting enough sleep, and removing stress-inducing factors as much as possible. Essential amino acids, the building blocks of the proteins that make up your skin, cells, and organs, also have built-in anti-infammatory actions. You can supplement with an anti-inflammatory blend such as Heal to help ease symptoms and promote overall wellness.
When to Seek Medical Treatment
If home eczema remedies do not reduce symptoms, you can try over-the-counter steroid creams such as hydrocortisone cream. Apply it no more than twice a day to the affected area after moisturizing to help the cream penetrate the skin. You can also try non-prescription allergy medicines such as cetirizine (Zyrtec) or fexofenadine (Allegra).
Calamine lotion, a mixture of zinc oxide and ferric oxide, is a top favorite for relieving the itch and blistery rashes of eczema.
There are a variety of specific creams that your doctor may prescribe to control itching, such as corticosteroid cream or antibiotic cream if your skin has a bacterial infection. For severe cases, the doctor may prescribe oral corticosteroids, which can definitely subdue eczema symptoms but can’t be used for the long term because they can cause serious side effects.
For severe eczema, it can help to wrap the affected area with topical corticosteroids and wet bandages. Light therapy/phototherapy may also help, but it is not commonly used because of harmful effects such as premature skin aging and risk of cancer. During a light therapy session, skin is exposed to controlled amounts of natural sunlight, artificial ultraviolet A (UVA) or ultraviolet B (UVB). As with all eczema treatments, it's important to talk to your doctor about the benefits and risks of light therapy.

Up to 25% off Amino
Shop NowTAGS: conditions
Join the Community
Comments (0)
Most Craveable Recipes



 833-264-6620
833-264-6620



















