By: by Amino Science
By: by Amino Science
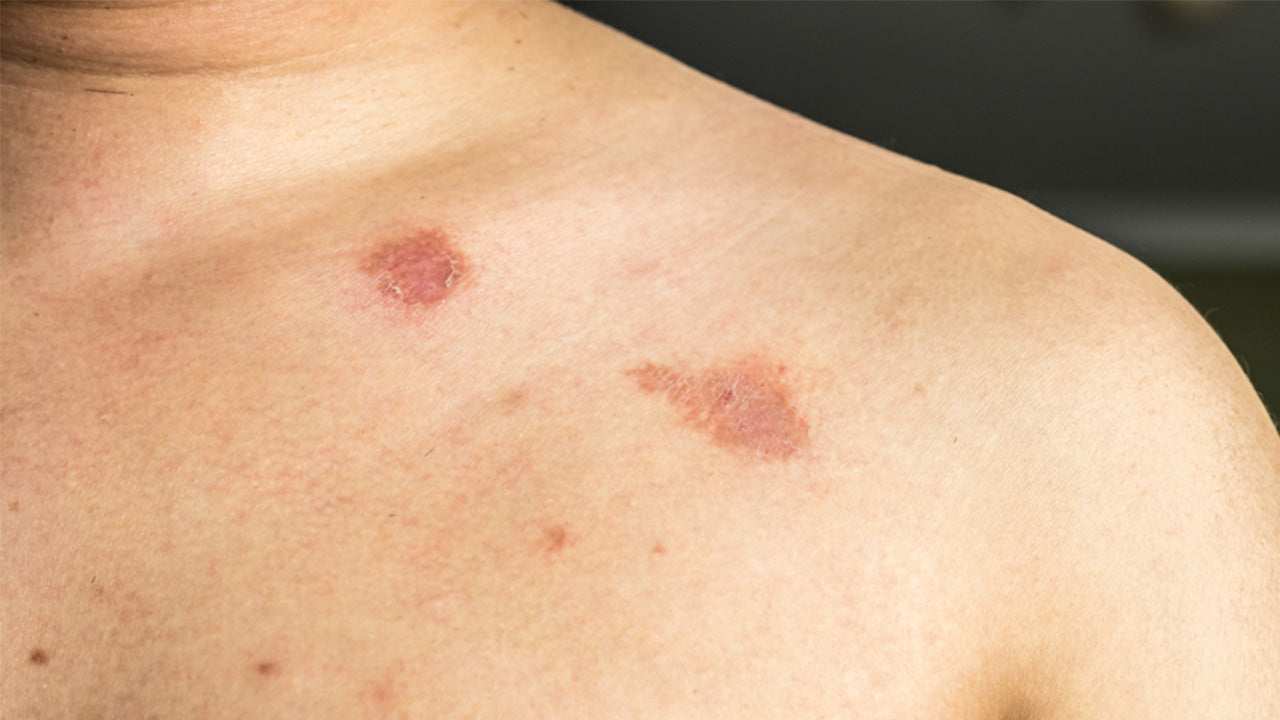
If you have ringworm, you may be wondering...is it really caused by a worm? Well, no, it’s not. But it is a common and highly contagious condition that can cause a variety of uncomfortable symptoms—and it may lead to an even more serious infection if not properly treated. So come with us as we explore all things ringworm, its causes and symptoms, and uncover everything you need to know about nipping this unpleasant infection in the bud.
Ringworm, also known as tinea or dermatophytosis, is a contagious hair, nail, or skin infection caused by mold-like fungi known as dermatophytes. These fungi, which belong to three different genera—Trichophyton, Microsporum, and Epidermophyton—live on the outer, keratinized layer of skin, hair, and nails and are referred to as “ringworm” because the rash they create often takes the form of a ring with a raised, scaly border resembling a worm.
Like most fungi, the dermatophytes that cause ringworm grow best in warm, moist areas, such as those found in swimming pools and locker rooms, where they’re spread by skin-to-skin contact with infected people or animals as well as personal items like clothing, towels, and sports equipment.
Because ringworm is so contagious, anyone who comes in contact with the fungi that cause the condition can be infected. However, certain groups are more at risk than others. These include:
Ringworm infections take different names, depending on the part of the body affected. Common types of ringworm are:
Ringworm symptoms generally appear within 4 to 14 days after exposure to the fungi, and their appearance varies depending on where on the body the infection takes place.
For example, ringworm that affects the body usually begins with a flat, red, itchy, scaly patch that develops an expanding, raised border that resembles a ring—or several overlapping rings—or wavy, worm-like line.
Jock itch, the fungal infection that occurs in the groin, may appear as red, itchy, scaly patches on the inner skin folds of the thighs.
Scalp ringworm, which is more common in children than adults, is often identified by a circular, red, itchy, scaly bald spot that can increase in size or spread if not appropriately treated. In severe cases, tinea capitis may lead to painful inflammation called kerion. The result of an allergic reaction to the dermatophytes that cause ringworm, the draining, pus-filled areas that characterize kerion can lead to permanent scarring and hair loss.
Ringworm that affects the beard may include red, itchy, scaly spots on the cheeks, chin, or upper neck that crust over or fill with pus and sometimes lead to hair loss.
Athlete’s foot generally begins between the toes, where the skin becomes red, itchy, and swollen and begins to peel or, in severe cases, blister. The skin on the sole and heel of the foot may be affected as well.
Ringworm involving the hands may resemble tinea corporis, though it typically presents with dryness, itching, and peeling on the palm of the hand. Similar to tinea pedis, tinea manuum may cause crops of blisters that itch and burn.
Ringworm that affects the finger- or toenails may cause the nails to become thickened, discolored, and misshapen. The nails may also become crumbly and split or separate from the skin. In addition, the nails may give off a slightly foul odor and become darker as debris builds up underneath.
To confirm a diagnosis of ringworm, your health care provider may simply need to look at the infected area. However, more complicated cases may require a skin, hair, or nail sample. Once diagnosed, treatment will depend on the area affected.
Ringworm involving the skin can usually be treated at home with over-the-counter antifungal creams such as clotrimazole (Lotrimin AF), miconazole (Baza), and terbinafine (Lamisil AT), while ringworm of the scalp may be treated with oral antifungal medications like griseofulvin (Grifulvin), terbinafine (Lamisil), and itraconazole (Sporanox) as well as antifungal shampoos like ketoconazole (Nizoral). Similarly, onychomycosis may be treated with over-the-counter or prescription antifungals or even oral medications.
Before opting for oral antifungal medications, it’s important to note that these drugs can cause serious side effects—including kidney, liver, and heart failure—in some people. (Always keep your liver, kidneys, and heart safe and protected with essential amino acids.)
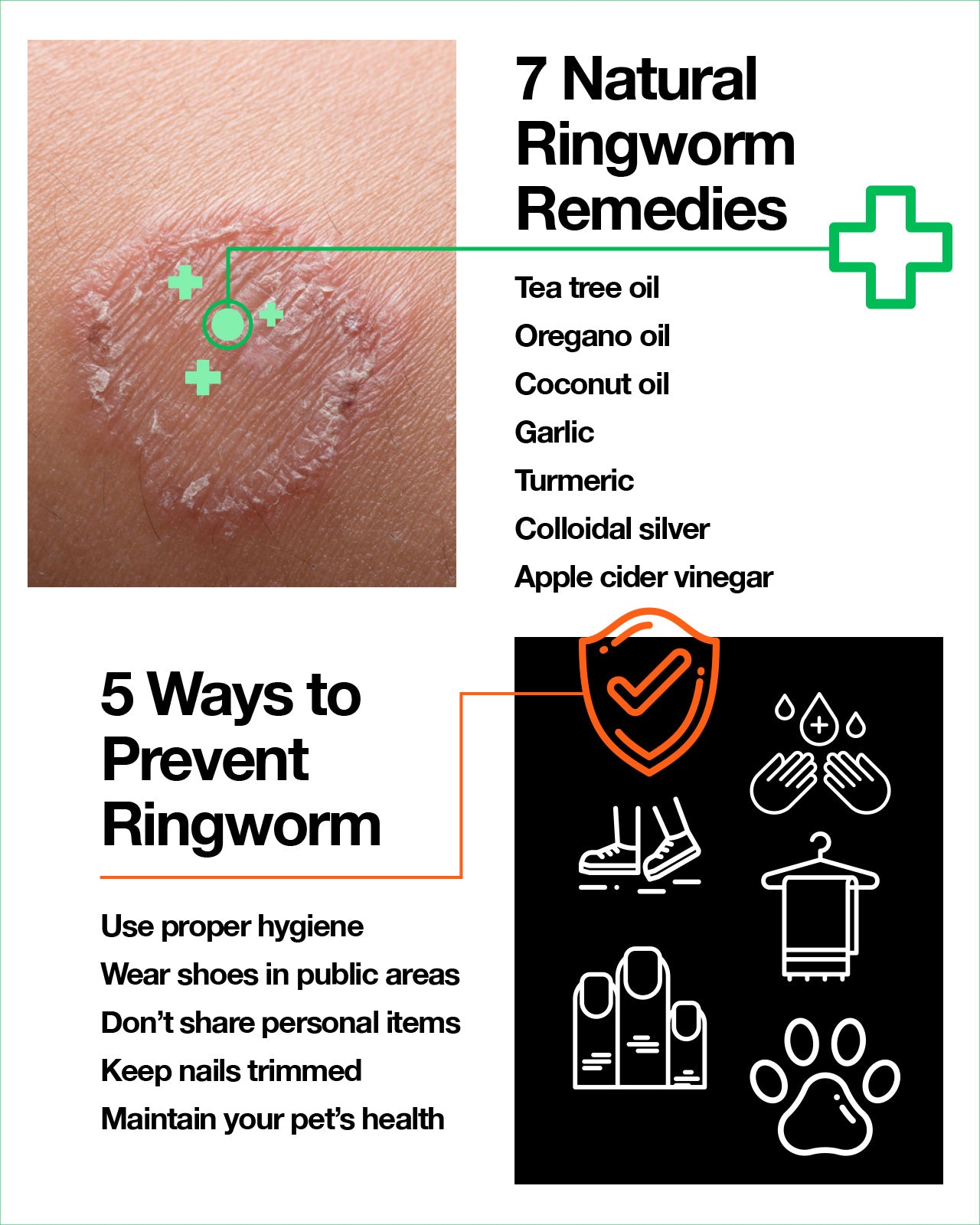
Fortunately, there are a number of natural remedies that have been shown to be both safe and effective against the fungi that cause ringworm.
The leaves of the tea tree plant, Melaleuca alternifolia, have been prized for centuries by the Aboriginal people of Australia for their antiseptic and antifungal properties—uses that have now been backed up by science. In fact, tea tree essential oil has been shown in multiple studies to be effective against the pathogens that cause ringworm in both humans and animals. To use tea tree oil for the treatment of ringworm, simply apply 1 or 2 drops of the oil directly to the infected area 3 times daily. For those with sensitive skin, the oil can also be diluted in a carrier oil like coconut or almond.
Oregano essential oil is one of the most powerful essential oils available and has been shown to possess impressive antibacterial and antifungal properties that rival the effects of even the most potent pharmaceuticals. Like tea tree oil, oregano oil can be applied to areas of ringworm 3 times a day. But because oregano oil is extremely potent and can irritate sensitive skin, it’s best to dilute it in a carrier oil like coconut or almond before applying.
Coconut oil not only makes a great carrier oil for use with essential oils but also has antimicrobial and antifungal properties of its own. In fact, studies have found that the medium-chain fatty acids found in coconut oil cause cell death in bacteria, fungi, and viruses by disrupting their cell membranes. Coconut oil is also very moisturizing and can be used for the treatment of dermatophytosis on both the skin and hair. However, not all coconut oil is created equal, so be sure to look for unrefined, or extra virgin, coconut oil.
Although garlic has not yet been extensively studied in the treatment of tinea, the effectiveness of this member of the lily family has been seen in the treatment of a number of other pathogens, including Candida, and preliminary research has shown that garlic does display therapeutic activity against the fungi that cause ringworm. To try garlic for the treatment of dermatophytosis, apply a paste of crushed garlic and olive or coconut oil to the affected area, cover with gauze, and allow to stay in place for up to 2 hours twice a day.
This ancient spice has been a valued part of Ayurvedic medicine for at least 2,500 years and has been found by science to possess significant anti-inflammatory, antioxidant, and antimicrobial properties. And studies have demonstrated that turmeric oil is effective against the dermatophytes that cause ringworm. To use turmeric in the treatment of ringworm, create a paste by mixing the spice with water and applying topically to the skin. This mixture should then be allowed to stay on until dry. Turmeric can stain skin temporarily yellow, so be forewarned if using the spice on a noticeable area.
This powerful antimicrobial is effective against a wide range of microorganisms and has been shown in studies to be useful in the treatment of fungal infections as well. To use this remedy, simply apply colloidal silver to the affected area 3 times a day until the ringworm infection is gone. Because the efficacy of colloidal silver is a product of the percentage of silver particles and the particle surface area, be sure to look for true colloidal silver.
This popular type of vinegar has been found in studies to possess antifungal properties and has even been shown to be effective against Candida. To use apple cider vinegar for treating ringworm, dab the affected area with a saturated cotton ball 3 times a day until the infection is gone. Individuals with sensitive skin may want to dilute apple cider vinegar in water before applying.
Because ringworm is quite common and highly contagious, it can be difficult to prevent. But it is possible to reduce your risk with these simple steps:
Given enough food—which, for dermatophytes, means keratin—the fungal spores that cause ringworm can survive for up to a year on just about any surface. And although many sources recommend chlorine bleach for killing fungal spores, according to the Centers for Disease Control and Prevention (CDC), they can also be killed with simple soap and water and less noxious disinfectants like detergent.
In addition, both vinegar and tea tree oil, as mentioned earlier, as well as hydrogen peroxide possess antifungal properties that can make them useful for ridding the home of dermatophytes.
While most cases of ringworm can be easily treated at home, the fungal infection can be more difficult to treat in people with weakened immune systems. So if you or someone you love has symptoms of ringworm that don’t seem to be improving with conservative care, be sure to seek the medical advice of your health care provider.