What Is Psoriasis? Learn About Causes, Symptoms and Treatments
 By: by Amino Science
By: by Amino Science
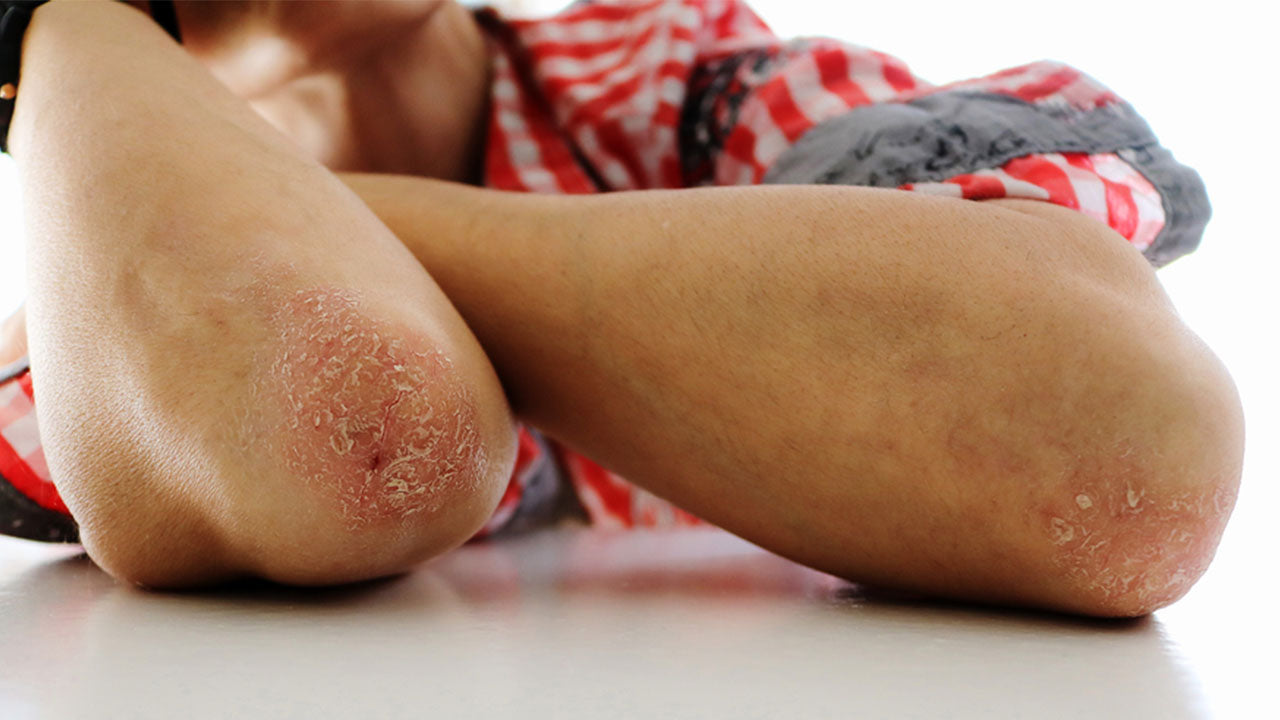
Psoriasis, a chronic autoimmune disease, affects up to 2.2% of Americans. Still, many people know next to nothing about this debilitating illness. So, what is psoriasis, anyway?
Psoriasis accelerates the life cycle of skin cells, causing a rapid buildup that results in scaling on the skin's surface. According to the American Academy of Dermatology, approximately 7.5 million people living in the United States, mostly between the ages of 15 and 30, must deal with this potentially uncomfortable and stigmatized condition.
Understanding what factors can lead to psoriasis outbreaks, as well as the most effective ways to alleviate symptoms, can minimize the effect this condition can have on a person's physical well-being, self-esteem, and overall quality of life.
What Is Psoriasis?
Before delving into the specifics of psoriasis causes, symptoms, and treatments, it's important to understand the biological mechanisms that drive this skin condition.
Psoriasis, in essence, results in a sped-up production of skin cells. Under normal circumstances, the body generates skin cells within the deepest layers of the skin. Those skin cells then slowly rise to the surface of the skin, and just as slowly, they fall away to reveal new skin cells. Typically, it takes a skin cell about one month to progress through this life cycle.
For people with psoriasis, the production process of skin cells happens much, much faster. New skin cells rise to the surface in just a few days. The pace of skin cell shedding does not match the pace of production, resulting in a buildup of skin cells that form psoriatic scales.
Psoriatic scales develop in thick, red patches. Often, the area surrounding psoriatic scales also becomes red and inflamed. Sometimes, the patches will crack and bleed. Understandably, it's not uncommon for patients with psoriasis to experience itching and pain as a result of the condition. In some cases, however, the psoriatic scales cause little physical discomfort and the primary goal of treatment is to resolve the emotional distress associated with psoriasis flares.
Although the red skin and scaling associated with psoriasis tends to develop at the joints, such as the elbows and knees, they can be found on any part of the body, including:
- Hands
- Feet
- Lower back
- Neck
- Scalp
- Face
While it's less common, certain types of psoriasis can affect the mouth, genitals, and even the nails.
Differentiating Between the 5 Types of Psoriasis
While all forms of psoriasis result from the overproduction of skin cells, the symptoms of psoriasis vary from type to type in terms of severity, location of psoriatic outbreaks, and more. Some types of psoriasis cause mild patches while others lead to severe lesions that cover more than 5% of the total surface of the skin. It's also possible to have more than one form of psoriasis, and getting a correct diagnosis is a key part of finding the best treatment options for your condition.
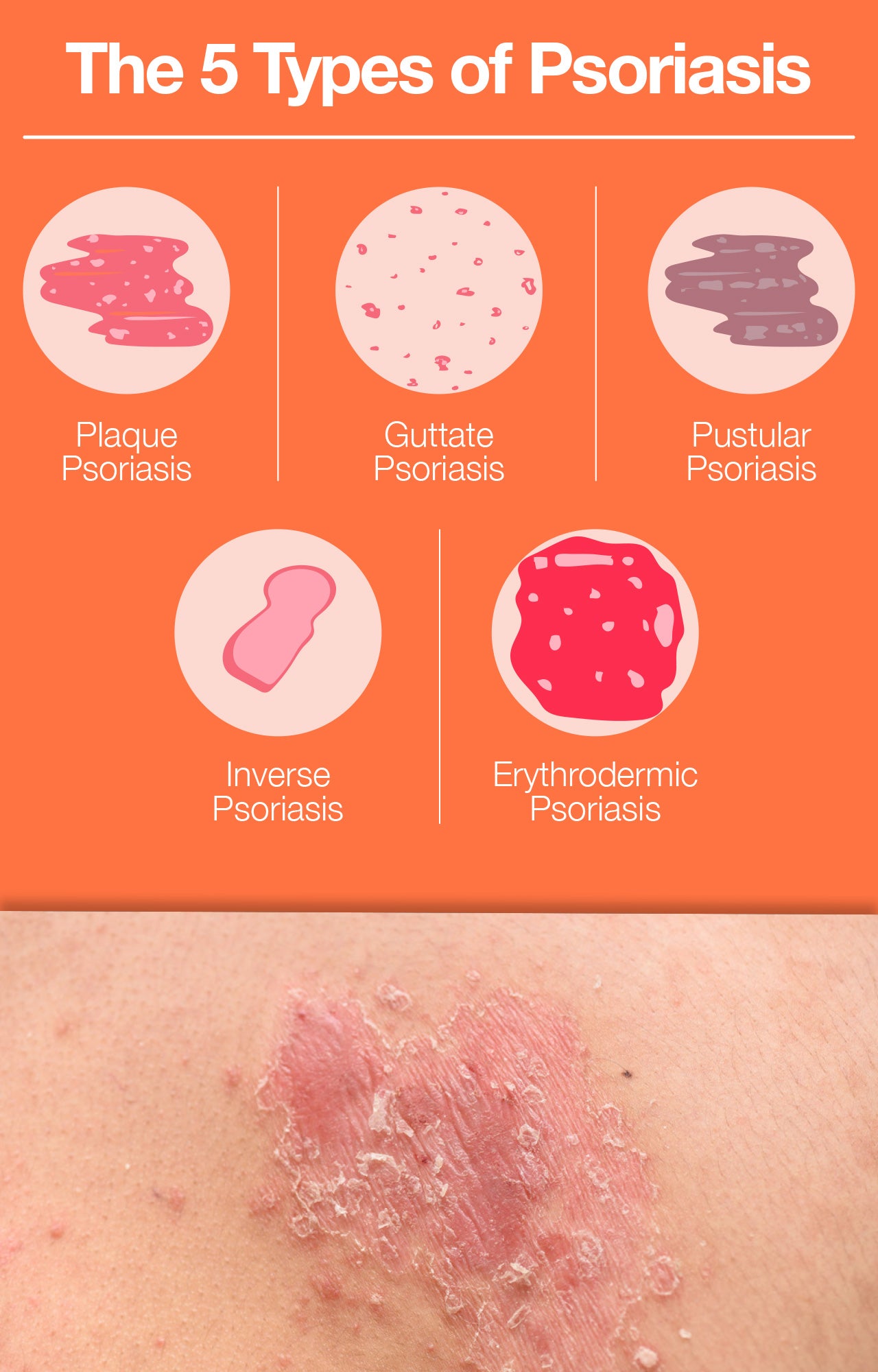
1. Plaque Psoriasis
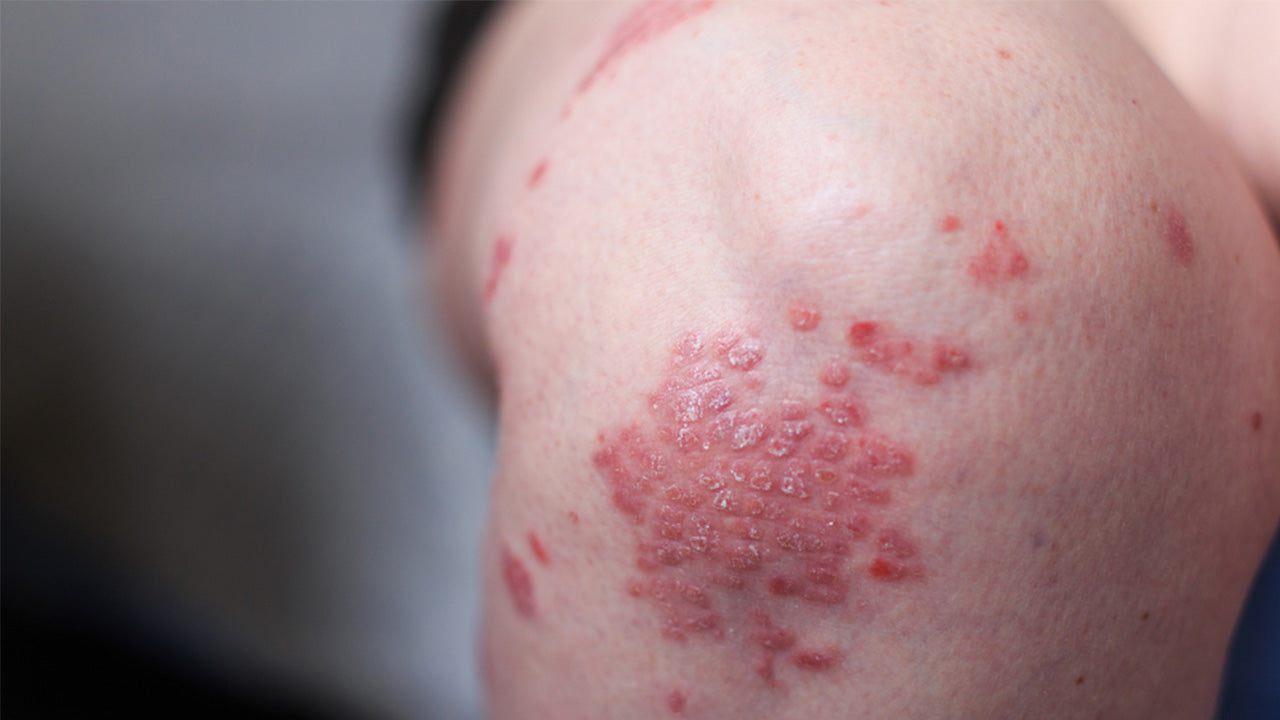
The most common type of psoriasis, plaque psoriasis typically causes dry skin and raised red lesions, often covered with scaly plaques that can be painful or itchy. The American Academy of Dermatology estimates that 80% of individuals with psoriasis have this type. Typically, plaque psoriasis affects the elbows, knees, and scalp, however, the plaques can occur anywhere on the body.
2. Guttate Psoriasis
Most common in children and young adults, guttate psoriasis often develops after the patient has suffered a bacterial infection. Guttate psoriasis typically presents as small, pink spots shaped like water drops. Though the spots tend not to be thick or raised, during a flare-up, hundreds of small lesions form. The arms, legs, and torso are the primary sites where lesions appear, followed by the face, ears, and scalp. Experts estimate that 10% of all people with psoriasis have this form.
3. Pustular Psoriasis
The opposite of guttate psoriasis, pustular psoriasis is most common in adults. This form of psoriasis presents as white pustules combined with swathes of inflamed red skin. The symptoms of pustular psoriasis tend to be cyclical: first the skin turns red, then small, pus-filled blisters appear, and finally, scales form. In most cases, pustular psoriasis develops on smaller areas of the body, like the hands and feet.
There are three forms of pustular psoriasis: von Zumbusch pustular psoriasis, characterized by its abrupt appearance and sometimes accompanied by fever, chills, and dehydration; palmoplantar pustulosis, which develops on the soles of the feet and on the hands; and acropustolosis, the rarest form and one in which outbreaks are limited to the ends of the fingers and toes.
5. Inverse Psoriasis
This type of psoriasis presents as patches of smooth, shiny, inflamed red skin in the armpits, beneath the breasts, in the skinfolds around the groin, and other areas where skin-on-skin friction occurs. Because inverse psoriasis flare-ups occur selectively in areas of the body prone to sweating and rubbing, it can be particularly uncomfortable. It can also be especially challenging to treat.
5. Erythrodermic Psoriasis
This very rare and severe psoriasis type often covers large portions of the body at the same time. Flare-ups cause skin to appear almost burned. The large, sheet-like lesions tend to be incredibly itchy and painful, and to slough off in large sections. A flare-up can lead to swelling, infections, increased heart rate, and fever. This type of psoriasis can be life-threatening and requires immediate treatment. In some instances, hospitalization may be necessary.
As mentioned in the preceding section, psoriasis sometimes affects the nails rather than (or in addition to) the skin. Nail psoriasis can appear on the fingernails and toenails and can result in symptoms ranging from minor discoloration to abnormal growth, pitting, nail separation, and even crumbling.
Understanding the Cause of Psoriasis
Doctors don’t know exactly why certain individuals develop psoriasis, but years of research have shown that there are two primary psoriasis causes: genetics and the immune system.
Individuals with a family history of the disease are more likely to develop psoriasis, especially if a parent suffers from the condition. People who are overweight also have an elevated risk for psoriasis and plaques that develop in skin folds.
Studies have shown that roughly 10% of the population inherits at least 1 of 25 or more genetic mutations that can cause you to develop psoriasis. However, according to the National Psoriasis Foundation, only 2% to 3% of the population actually develops the disease. This has led experts to conclude psoriasis only develops when a certain combination of genes become activated after exposure to a psoriasis trigger.
Common psoriasis triggers include:
- Infections such as strep throat
- Skin injuries like cuts, insect bites, and sunburn
- HIV or other immune disorders
- Stress
- Smoking cigarettes
- Overindulging in alcohol
- Cold, dry weather
- Sunburns
- A vitamin D deficiency
- Certain medications, including blood pressure drugs and lithium
Psoriasis kicks T cell-production into overdrive, eventually causing inflammation and faster-than-usual growth of skin cells, leading to psoriasis symptoms.
When someone with a genetic predisposition to psoriasis gets exposed to a trigger, the immune system responds by producing T cells, a kind of white blood cell that defends the body against infections and diseases. In patients with psoriasis, the T-cell production goes haywire and attacks healthy skin cells rather than simply targeting foreign invaders. The body responds to this attack by generating more skin cells, as well as T cells and white blood cells. The end result is skin redness, dilated blood vessels, and lesions.
10 Common Psoriasis Symptoms
Psoriasis symptoms vary from one person to the next, depending on both the type and whether it's mild, moderate, or severe psoriasis. Most psoriasis sufferers cycle through flare-ups, in which signs of the condition are worse, as well as remission periods, in which symptoms subside.
Some of the most common symptoms of psoriasis include:
- Raised, inflamed red patches of skin
- Thick, silvery, scaly plaques
- Soreness around patches
- Cracked or dry skin
- Skin itching, burning, or discomfort
- White pustules
- Shiny, smooth, red lesions
- Numerous small, teardrop-shaped red spots
- Thickened, pitted, or discolored nails
- Swollen and stiff joints
Depending on the type, or types, of psoriasis a person has, they may experience all these symptoms, or only a few. While some patients experience relatively mild psoriasis with just a few patches of redness, others have a more serious form of the disease that regularly interferes with quality of life. Even those with severe psoriasis may experience periods of remission in which symptoms of psoriasis disappear altogether. This doesn't mean that their psoriasis has been cured, however, and it's still important to avoid potential triggers.
An Overview of 8 Effective Psoriasis Treatments
Treating psoriasis is a challenge, as not all patients respond to the same medications. It’s not uncommon for psoriasis sufferers to try multiple treatments before they find one that’s effective.
At this time, it is not possible to cure psoriasis, though researchers are making strides in terms of uncovering what triggers psoriasis lesions on a cellular level and how to modulate the immune system's response to prevent flare-ups.
The current goals of psoriasis treatments are to reduce inflammation and scaling, slow the production of skin cells, and clear away plaques from the surface of the skin. With the right medication, therapy, or combination of medications and therapies, it's possible to dramatically reduce symptoms, and in some cases, to completely eliminate them.
Psoriasis treatment options typically fall into two categories: topical treatments and systemic medications. The outliers are light therapy and alternative and complementary therapies. Here's a brief overview of how 8 treatment options alleviate psoriasis symptoms and reduce flare-ups.
- Salicylic acid: A peeling agent, salicylic acid works by causing a shedding of the outer layer of skin. This over-the-counter topical treatment, one of the first-line options for mild to moderate psoriasis, is available in ointments, liquids, gels, and even shampoos. A downside is that it can result in mild skin irritation.
- Coal tar: Another over-the-counter, first-line topical treatment option, coal tar can be used to alleviate the itching and discomfort associated with psoriasis. Coal tar also helps the skin shed dead cells.
- Steroid creams: One of the principle psoriasis treatments, topical corticosterioids can reduce itching and inflammation while blocking excess cell production.
- Nonsteroidal topical treatments: Doctors may prescribe cacipotriene, a form of vitamin D, and tazarotene, a retinoid, to address persistent psoriasis that does not respond to other topical treatments. In some cases, they may also recommend anthralin cream, one of the original psoriasis treatments.
- Light therapy: By exposing the skin to ultraviolet light, it may be possible to kill the immune cells that contribute to the development of psoriasis outbreaks. The treatment can use UVB rays, a combination of UVA and UVB rays, or UVA rays in combination with an oral or topical medication called psoralen (PUVA). Also called phototherapy, this treatment must be administered by a doctor, in a psoriasis clinic, or with a specialized phototherapy unit, which can make it cost-prohibitive.
- Systemic medications: For individuals with psoriasis that fails to respond to topical treatments or light therapy, or those with moderate to severe psoriasis, doctors may opt to use systemics, prescription drugs that can be taken orally or by injection. These drugs affect the entire body and can come with intense side effects. Doctors usually prescribe them for short-term use. Popular drugs in this category include: cyclosporine (an immunosuppressant that slows skin cell growth), acitretin (an oral retinoid that slows the rate of skin cell growth and shedding), and methotrexate (developed to treat cancer and able to slow the growth of skin cells).
- Biologic drugs: Administered by injection or IV infusion, biologics contain human or animal proteins and work by blocking immune cells implicated in the development of psoriasis. At this time, all three types of biologics used to treat psoriasis shut down immune system chemical messengers called cytokines that promote inflammation. The cytokines they block are tumor necrosis factor alpha (TNF-alpha), interleukin 12 (IL-12), interleukin 23(IL-23), and interleukin 17-A (IL-17A).
- Complementary therapies: Evidence indicates that modalities such as acupuncture, massage, and Reiki can help relieve symptoms of psoriasis such as pain, as well as control environmental factors like stress that are known to trigger psoriasis flare-ups. Meditation, yoga, and tai chi also fall into this category. Complementary nutritional aids, especially essential amino acids, can also help reduce symptoms of psoriasis.
Some patients see results by treating psoriasis naturally. Herbal remedies for this skin disease include apple cider vinegar, turmeric, tea tree oil, and aloe vera, among others.
Psoriasis symptoms can also be eased with a psoriasis diet. Find out what foods you can and can’t eat on the psoriasis diet in this article.
In many cases, particularly for individuals with moderate to severe psoriasis, the best results will come from a combination of treatments. Once a person finds an effective treatment regimen, they may be able to use it for life. In some cases, symptoms may stop responding to a previously effective option. It can be highly beneficial to find a trusted health care provider with experience in treating psoriasis to work with you to create a long-term plan for managing your psoriasis.


Up to 25% off Amino
Shop NowTAGS: conditions
Join the Community
Comments (0)
Most Craveable Recipes



 833-264-6620
833-264-6620



















