By: by Amino Science
By: by Amino Science
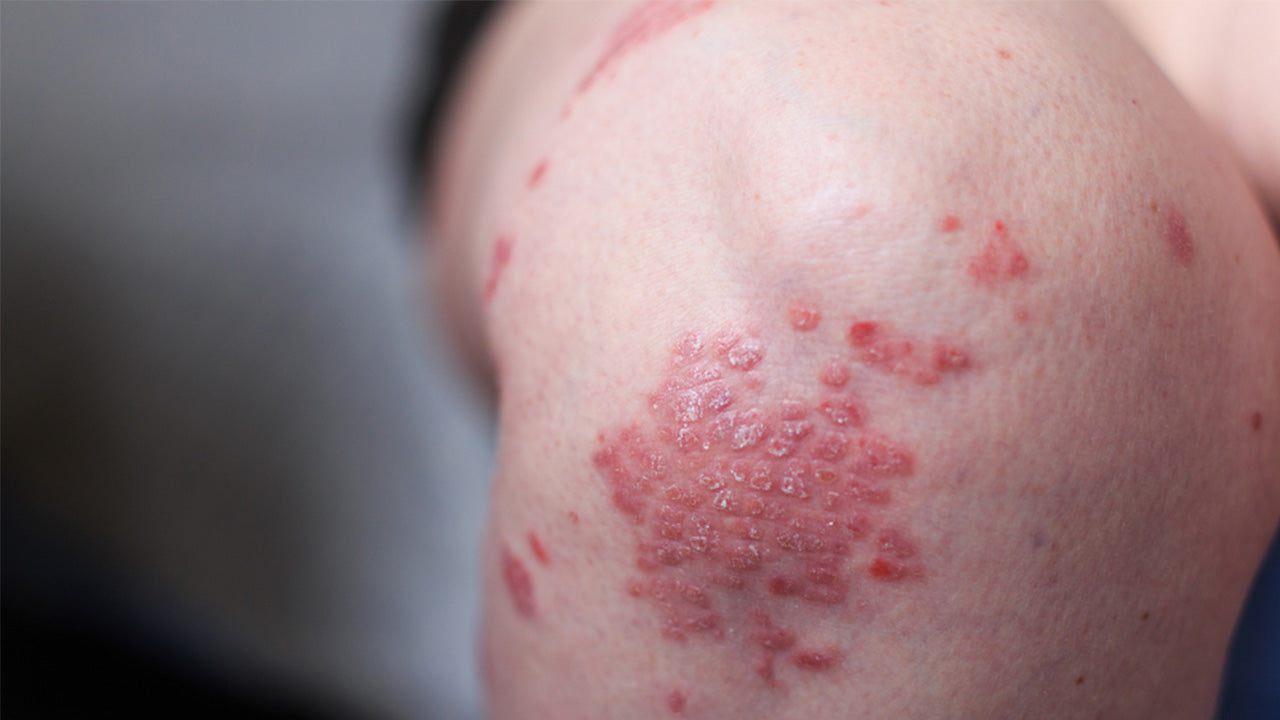
Psoriatic arthritis is a type of inflammatory arthritis that can affect a person with the skin disease psoriasis. It may target any joint in your body, and symptoms vary from person to person. In some individuals, psoriatic arthritis is mild, with just occasional flare-ups. In others, it can become a chronic condition that leads to joint damage, especially if not treated properly. Fortunately, there are treatment options available that have shown to be effective at combating the condition and providing symptom relief.
Psoriasis is a skin condition and type of autoimmune disease that causes the body’s immune system to activate and skin cells to grow extremely quickly, resulting in scaly white and red patches on the skin’s surface. Some people with psoriasis can also develop psoriatic arthritis, where inflammation appears in the joints and causes them to stiffen and swell. How it develops differs in people; it can appear in one joint or both and affect the spine, knees, ankles, hands, and even the toenails and fingernails. Psoriatic arthritis can appear in both genders and all ages, even in young children, but it most often affects people in their 30s and 40s.
Psoriatic arthritis can be divided into several different categories, and identifying your specific type of arthritis can help you and your health care practitioner develop an appropriate treatment plan that provides the best results.
The cause of psoriatic arthritis has not been pinpointed, but 40% of Americans who have the condition have arthritis in their family history, indicating the role genetics plays on the risk of development.
Psoriatic arthritis can result from an infection or illness that activates the immune system and, when combined with a predisposed genetic factor, causes the disease to develop.
Environmental factors such as exposure to chemicals or toxins, and even high stress, may cause the onset of psoriatic arthritis among people who already have a family history of the disease.

Not everyone who has psoriasis will develop psoriatic arthritis, and it is often not identified in the early stages because discussing skin issues is often the focus of a doctor’s appointment. There is a very large variety of arthritic conditions, many with similar symptoms. For many, signs of psoriatic arthritis do not develop until 5 or 10 years following the appearance of psoriasis, but there are exceptions when psoriasis and psoriatic arthritis occur at the same time.
The most common symptoms of psoriatic arthritis are stiffness and pain in the joints, specifically in the morning, fatigue, and general difficulty moving around throughout the day. Here are some other psoriatic arthritis symptoms.
The earlier psoriatic arthritis is identified, the better, because chronic inflammation can lead to serious complications and damage to joints and tissues. If you have psoriasis and begin to show signs of psoriatic arthritis, you most likely will visit a rheumatologist who specializes in these types of conditions. Your doctor will discuss your symptoms and any changes you’ve recognized in your nails, skin, and joints. Joint destruction can be seen on an X-ray, or with an MRI or CT scan, and will help with a more accurate diagnosis.
Your doctor will likely order blood tests to ensure other conditions are not to blame and to measure the inflammation present in your body. Inflammatory diseases like rheumatoid arthritis, osteoarthritis, and gout can affect similar parts of the body and cause identical symptoms, so it is important an accurate diagnosis is made to develop the most effective treatment plan.
Treatment of psoriatic arthritis will be customized to your specific symptoms and the severity of your swelling, pain, and joint inflammation. If psoriatic arthritis does not disrupt your day-to-day too greatly, simple self-care activities and exercise may be effective and medication may not be needed for an extended period of time. For others, a long-term treatment plan may be needed to deal with chronic inflammation, pain, and potential joint damage. Non-steroidal anti-inflammatory drugs including ibuprofen or naproxen may be used for the short term to provide relief.
If you do not find relief from initial methods, your doctor may prescribe disease-modifying anti-rheumatic drugs or DMARDs. These medications are meant to slow a disease from progressing, lessen inflammation and pain, and minimize further joint damage.
TNF-alpha inhibitors help ease joint pain by decreasing morning stiffness and joint swelling and tenderness. These drugs do come with potential side effects such as nausea, diarrhea, hair loss, and vulnerability to infection.
There are also drugs that can be injected directly into the area of the joint for temporary relief of symptoms.
Many people with arthritis develop joint symptoms, such as stiff joints and muscle weakness, because they become sedentary and do not move around. Incorporating exercise into your daily routine is essential when living with psoriatic arthritis because keeping joints and tendons moving reduces the inflammation, which in turn lessens the pain.
Joints can quickly stiffen when not in use. Building up your muscles minimizes the wear and tear on your joints. Exercise does not need to be strenuous or difficult. It can include walking, riding a bike, or water activities. Swimming and aerobics in the pool are great low-impact exercises that build muscle while being gentle on the joints. Physical therapy may also be very beneficial to help strengthen your muscles, improve flexibility, and protect joints from further damage.
An important step to keep in mind when living with psoriatic arthritis is to remove foods from your diet that can trigger inflammation and worsen symptoms. Cut out caffeine, sugar, processed foods, alcohol, and high-fat items from your diet and replace them with anti-inflammatory foods like green leafy vegetables, cold-water fish, broccoli, walnuts, and pineapple.
You can also supplement your diet with vitamins that specifically target arthritis and the symptoms associated with such conditions. Turmeric, a yellow spice often found in Indian food, contains curcumin, a chemical with amazing anti-inflammatory powers. According to research, curcumin can help reduce inflammation in the joints, which in turn relieves the pain and stiffness you may experience.
If you also have psoriasis along with psoriatic arthritis, over-the-counter ingredients that can be helpful in relieving symptoms include the amino acids glycine and methionine. In one study, it was found that psoriasis lesions have a significant loss of amino acids in these areas. When these parts of the body were injected with amino acids, it helped to supplement the deficiency and improve the skin’s condition.
The essential amino acid methionine is among a group of substances known for their cartilage-forming abilities. Methionine can be found in meat, fish, and dairy products and plays an important role in many of your body’s functions. The cartilage in our joints needs sulfur to form properly. If there is not enough sulfur available in the body, negative effects can arise over the long term. If you have a sulfur deficiency, especially in combination with psoriatic arthritis, damaged joints and tissues can take much longer to heal. Methionine can help supplement this lack of sulfur and build and strengthen the cartilage needed for healthy joints.
On top of stimulating cartilage formation, methionine is also packed full of power as a pain-reliever and an anti-inflammatory agent. Since it is able to form connective material, methionine can strengthen your hair and nails as well.
However, taking a single amino acid supplement, such as methionine, can deliver unnecessary side effects. Because amino acids work in concert with one another, giving elevated concentrations of just one can throw off optimal concentrations of all amino acids in the blood, and the desired benefits are lost. For this reason, it’s important to supplement with a balanced mixture of all the essential amino acids to keep amino acid concentrations in the body stable.
Other minerals and vitamins can support your joint health and help give your body what it needs to effectively combat psoriatic arthritis. Vitamin C, in particular, helps to form collagen, which is useful for lowering inflammation and helping to regenerate lost cartilage that is slowly worn away. Other important nutrients for healthy joints are magnesium and vitamin B6 since they ward off free radicals that break down cartilage in the joints and worsen symptoms.
Living with psoriatic arthritis over the long term can be challenging and exhausting, but it does not need to rob you of an active lifestyle or doing the activities you enjoy. Working with your doctor and physical therapist, as well as practicing proper self-care and exercise, can vastly improve your quality of life and keep you moving freely with much less pain.