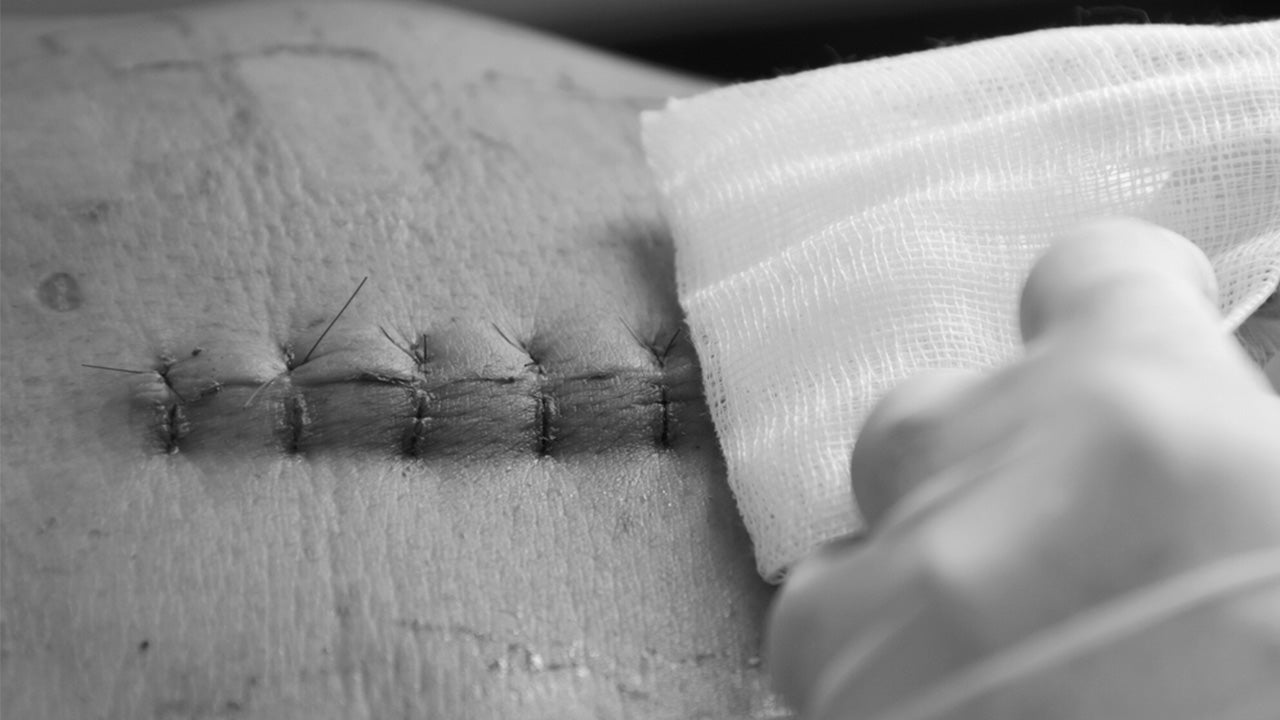
The basics of laceration repair have been more or less the same for over a century, but wherever there is room for improvement, medical professionals are ready to adapt. The development of synthetic skins and tissue adhesives, dissolvable stitches, and safe topical anesthetics have refined the process of wound management. This article is a comprehensive review of how to suture a wound and promote optimal recovery.
Wound Physiology
Proper wound care involves supporting hemostasis, minimizing scarring, and avoiding wound infection. Lacerations may afflict the dermis, epidermis, subcutaneous layer, and the deep fascia, which is why it may be necessary to irrigate deeper wounds to clean and sterilize beneath the skin edges. Here's the breakdown of these layers.
-
Dermis and epidermis: Together, these two layers constitute the skin and are clinically indistinguishable from one another (though they are microscopically distinct). Shallow cuts to the dermis may be best treated with a bandaid or steri-strip.
-
Subcutaneous layer: This is the layer beneath the skin of fat (adipose tissue), nerves, hair follicles, and blood vessels. Deeper wounds that require sutures often have a better cosmetic result if the stitches are placed in this layer.
-
Deep fascia: This is the muscle layer beneath our skin and fat that may require intensive suturing.
The Healing Process of Skin
The skin heals itself in five steps.
-
Coagulation: The first response to a wound is blood coagulation wherein platelets aggregate and clot to stop bleeding and summon an immune response.
-
Epithelialization: In the epidermis, cells begin to regenerate and reknit the skin back together.
-
New blood vessel growth: In the first 4 days following injury, new blood vessels are synthesized to replace the damaged tissue.
-
Collagen formation: Collagen regeneration helps restore tensile strength and flexibility to the skin. This process may take place for up to a full year depending on the wound's severity.
-
Contraction: In the initial 3 to 4 days after injury, wound thickness concentrates in the center in a process that is not fully understood by doctors except for the consequence of changing the appearance of scarring.
This healing process may be interrupted by infection and can also be influenced by factors such as underlying tissue trauma, denervation, body temperature, and ischemia (a restriction in blood supply to the tissues).
Suture techniques can be employed to take ischemia into consideration, like the vertical mattress suture (discussed in further detail below). Identifying and removing any foreign bodies from the wound and employing tetanus shots can help reduce the risk of damaging infections.

Suture Materials
Once the area has been cleaned and prepared, your health care provider has a choice of suture materials, many of which have pros and cons depending on the area that needs repair. Here's a quick overview of those options.
Absorbable Sutures
-
Catgut: These sutures are derived from cattle or sheep vessel linings (intima) and can retain tensile strength for up to 2 weeks of skin closure. Follow-ups for suture removal are usually recommended within the first week once natural healing has taken hold.
-
Polyglactin 910 (Vicryl): This is a synthetic suture that is braided and lubricated with improved tensile and knot strength over catgut. It's considered best for subcutaneous sutures.
-
Vicryl Rapide: A fast-absorbing suture that is favored for skin closure as it will "fall off" within 7 to 10 days without requiring suture removal. It's particularly useful for sutures that need to be placed under casts rather than employing nonabsorbable sutures.
-
Poliglecaprone 25 (Monocryl): A monofilament that provides easier handling and pliability, best used in cases of facial lacerations and subcuticular running sutures (more on suture types below).
-
Polyglycolic acid (Dexon): The first absorbable synthetic suture made of a braided polymer. It has since been improved upon to reduce snagging and binding when wet.
-
Polydioxanone (PDS): With more tensile strength than Vicryl, this monofilament may help reduce infection potential with a lower friction coefficient than Vicryl.
Nonabsorbable Sutures
-
Silk: A natural product, silk has the lowest tensile strength among nonabsorbable stitching materials. It is now rarely used due to the availability of superior materials.
-
Nylon (Dermalon, Ethilon): The original synthetic suture, nylon has high tensile strength, low cost, minimal tissue irritation, and excellent elasticity.
-
Polypropylene (Surgilene, Prolene): A synthetic plastic suture with high tensile strength much like nylon. Its plasticity allows it to expand to allow for wound swelling. It comes in blue coloring that is useful for visibility during removal.
-
Polybutester (Novafil): A synthetic copolymer monofilament with greater elasticity than polypropylene or nylon, which leads to lower amounts of scarring.
The type of suture material selected depends on many factors, including the location of the laceration, the likelihood of infection, the potential for wound dehiscence, and whether a follow-up appointment for removal is viable.

How to Suture a Wound: Techniques
The name of the game when it comes to wound healing is skin closure, and yet there are several ways to sew up a laceration. Here are some of the leading suturing techniques.
-
Percutaneous skin closure: This is the simple interrupted suture frequently used in emergency medicine on uncomplicated wounds like, say, cutting yourself so badly with a kitchen knife that it requires a trip to the ER. The tip of the needle penetrates the skin's surface, loops evenly with the opposite side of the wound and as widely/deeply as required by the size and location of the laceration. The suture continues for as many stitches as are required to fully cover the wound edges.
-
Dermal closure: The dermal or buried suture is meant to hold the wound closed just below the dermal-epidermal divide and is used when wounds are so deep that closing the layer overtop the wound would leave "dead space" open underneath. This wound requires absorbable sutures and the knot needs to be buried deep so it won't interfere with healing on the top of the skin surface. This stitch is perfectly suited for thoroughly cleaned wounds, but the higher the risk of contamination, the higher the risk of infection.
-
Running suture: Best for the rapid closure of long wounds, the running suture evenly distributes tension and is a variation of the simple interrupted suture.
-
Subcuticular running suture: Often used on facial lacerations to minimize scarring, it involves running a continuous stitch in the dermis, and then closing the outer edges of the wound with adhesive tape.
-
Vertical mattress: For wound edges that are at risk of folding into the wound, the vertical mattress technique (also known as the vertical Donati stitch) closes both the deeper layers and the surface layer of the wound at once.
-
Horizontal mattress: A horizontal mattress suture everts the stitch (turns it upside-down like a series of saddles that run under the wound). Wound eversion allows the tension of the suture to be placed farther away from the primary closure point.
Wound Closure Aftercare
Wound healing is primarily done by the body's own regeneration mechanisms, the reformation of collagen and the reknitting of the skin on a cellular level. However, there are ways you can improve the healing process: the first is by never attempting self-suture unless you're in extremely dire circumstances (stranded during an emergency perhaps), and the second is by embracing the following tips.
-
Amino acid supplements: Healing means tissue rebuilding, and tissue cannot be rebuilt without all nine of the essential amino acids (EAAs). Increasing your protein food intake, consuming protein shakes, or even better, taking a fully balanced EAA supplement helps you heal a sutured wound faster.
-
Proper dressing and bathing: Antibiotic ointments and gentle cleaning of the area help reduce the risk of infection and inflammation. Follow the doctor's instructions on when and how to wash and dress your wound.
-
Tetanus prophylaxis: This is the fancy name for a tetanus shot. It helps boost your immune system's defense while you're in a vulnerable state of healing.
-
Antibiotics: A doctor may prescribe preventative antibiotics to take in the initial healing phase, again to lower the risk of infection as much as possible, and especially in cases like wounds resulting from an animal bite or cut from a dirty or rusty object.
-
Anti-inflammatories: To reduce the pain felt at the wound site, over-the-counter or natural anti-inflammatories may be beneficial.
Take Care
Be sure to attend any follow-up appointments and to adhere to all wound care advice given by your doctor, as it could mean the difference between a quick recovery and a life-threatening infection. Beyond that, boost your nutritional intake with amino acid foods and supplements to supply the building blocks needed to synthesize new tissue, and enjoy a speedy recovery.
 By: by Amino Science
By: by Amino Science