Getting Rid of Varicose Veins: Treatment and Prevention
 By: by Amino Science
By: by Amino Science
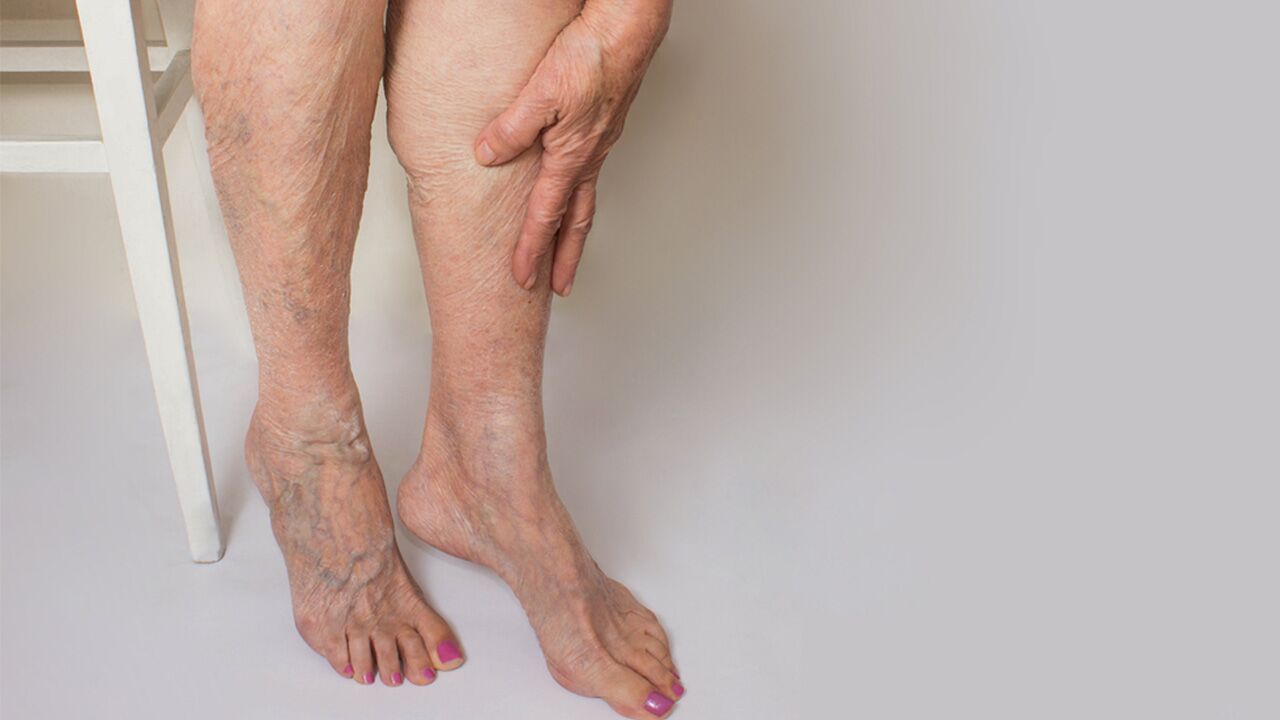
Varicose veins. If you have them, they probably need no further introduction. And if you do have varicose veins, you're not alone. According to the Society for Vascular Surgery, as many as 35% of people in the United States may be affected by the condition. But what causes these gnarled, enlarged, superficial veins, and what can you do about them? In this article, we're going to answer this question and discuss the various treatment options available for varicose veins as well as what you can do to help prevent them from occurring in the first place.
What Causes Varicose Veins?
As we just mentioned, varicose veins are twisted, engorged, superficial veins. While they can occur on various parts of the body, they're typically seen in the legs and feet. Unlike arteries, which are responsible for sending oxygen-rich blood out to the body, veins carry blood back to the heart to prepare it for reoxygenation by the lungs.
The veins work against gravity to pump blood through a series of small, one-way valves. If these valves malfunction, blood can begin to flow backward and collect in the veins. When this happens, it causes pooling of the blood, which then puts pressure on the vein walls, causing them to weaken and swell and form varicose veins.
Varicose Veins vs. Spider Veins
Although both varicose veins and spider veins have the same basic cause, they're not identical conditions. Varicose veins are large, bluish veins that can be felt right under the surface of the skin. By contrast, spider veins may be either red or blue. They also look like a spider's web or branches of a tree and are rarely larger than a millimeter in size.
In addition, while varicose veins are caused by leaky one-way valves, spider veins may have other vascular causes. And spider veins are little more than a cosmetic concern, whereas varicose veins can cause unpleasant symptoms and sometimes lead to complications.

Complications of Varicose Veins
Although varicose veins rarely cause serious issues, complications can and do occur. The most common of these are:
- Blood clots: Only a fraction of people with varicose veins develop blood clots, and these are usually self-limited and confined to the superficial veins. However, in about a quarter of cases, these superficial clots move to the deeper veins and cause a more serious condition called deep vein thrombosis. When blood clots enter the deep veins, they can sometimes travel to the lungs and cause a pulmonary embolism, which can lead to death.
- Ulcers: If the leg veins have difficulty pumping blood back to the heart, the blood can back up, which can put pressure on the skin and lead to an open sore. These venous ulcers typically occur on the lower leg, near the ankle, and require immediate medical attention.
- Bleeding: Because the walls of varicose veins are weak, they can occasionally rupture after even a minor trauma. Although varicose vein bleeding is usually insignificant, it can sometimes be profuse and require immediate care.
Risk Factors for Varicose Veins
While anyone can have varicose veins, certain individuals are at a greater risk of developing the condition. Factors that lead to a higher risk of varicose veins include:
- Family history: People with family members with varicose veins have a greater risk of developing the condition.
- Age: People over the age of 50 have a greater chance of developing varicose veins.
- Sex: Women are more likely to have varicose veins, likely due to fluctuations in female hormones, which are known to relax vein walls.
- Pregnancy: Women who are pregnant are more likely to develop varicose veins due to increased blood volume as well as the aforementioned hormonal changes.
- Weight: People who are overweight or obese have a higher chance of developing varicose veins.
- Activity: Standing or sitting for long periods of time leads to decreased blood flow and increases the risk of varicose veins.
Symptoms of Varicose Veins
Varicose veins often don't cause any symptoms. However, when symptoms do occur, they may include:
- Heaviness or aching in the legs
- Lower leg swelling
- Itching, burning, or throbbing in the legs
- Pain after prolonged sitting or standing
- Skin discoloration around the affected vein
Diagnosing Varicose Veins
After speaking with you about your history and symptoms, your health care provider will perform a physical exam that includes observing your legs for signs of swelling when you're standing. In addition, an ultrasound may be performed to evaluate your varicose veins and assess them for blood clots.
Varicose Vein Treatment
Treatment for varicose veins depends on several factors, including symptoms and cosmetic concerns. If no symptoms are present, and aggressive treatment is neither required nor desired, conservative therapy will probably be recommended.
Conservative Therapy
There are a variety of self-care strategies and lifestyle changes that can be implemented at home to help reduce the symptoms of varicose veins. These include:
- Regular exercise
- Weight loss (in those who are overweight)
- Avoidance of high heels, leg crossing, and tight legwear
- Increased fiber intake
- Limited salt intake
- Leg elevation
- Avoidance of prolonged sitting or standing
- Use of compression stockings
The first recommendation of many health care providers is to wear compression stockings, as these garments apply steady pressure to the legs and help the veins and muscles pump the blood more efficiently against gravity.
However, several natural supplements have also been shown to improve the symptoms of varicose veins. And one of the most extensively studied is horse chestnut.
A 2006 review of five clinical trials found that horse chestnut seed extract is both safe and effective in reducing lower leg edema and alleviating leg pain, heaviness, and itching in patients with both varicose veins and chronic venous insufficiency, a related condition.
Similarly, a 2002 study involving butcher's broom found the herb to be both safe and effective for the treatment of chronic venous insufficiency.
There's also evidence that flavonoids can help shrink varicose veins by improving blood circulation.
In fact, a 2016 study demonstrated that the flavonoid-based medical food micronized purified flavonoid fraction (MPFF) is effective in reducing vein diameter and pain and increasing blood flow in patients with varicose veins of the pelvis. And a 2017 study found that the same substance is effective in healing venous ulcers and reducing the symptoms of edema associated with chronic venous diseases.
Procedures
For patients who don't respond to conservative measures or who desire more aggressive treatment for cosmetic purposes, several procedures are available. These include:
- Sclerotherapy: This procedure uses injection of an irritant to collapse and seal varicose veins. Sclerotherapy can be used with both varicose veins and spider veins.
- Laser treatment: This noninvasive procedure uses bursts of light to fade smaller varicose veins and spider veins.
- Radiofrequency ablation: This procedure utilizes a catheter inserted through a small incision to deliver radiofrequency energy to the varicose vein until it collapses and seals shut.
- Ambulatory phlebectomy: This outpatient procedure can be used to remove smaller varicose veins through small punctures in the skin.
- Vein stripping: This procedure, which is performed on either an outpatient or inpatient basis, is used to tie off (ligate) and remove a varicose vein via one or more small incisions. Vein stripping is generally performed on the greater saphenous vein.
Varicose Vein Prevention
Although it’s not always possible to prevent varicose veins, getting plenty of exercise, maintaining a healthy weight, eating a diet rich in fiber and phytonutrients, and implementing the other self-care strategies and lifestyle changes detailed above can help you reduce your risk. Life, a patented essential amino acid supplement, can also help prevent varicose veins by supporting healthy blood flow and preserving heart strength and function. Learn more about this active aging supplement here.
But if you're already suffering from varicose veins and find that conservative treatment isn't working or your symptoms are getting worse—or if you're simply concerned about your appearance—don't hesitate to contact your health care provider to discuss additional treatment options.

Up to 25% off Amino
Shop NowTAGS: anti-aging conditions
Join the Community
Comments (0)
Most Craveable Recipes



 833-264-6620
833-264-6620



















