MRSA (Staph) Infection: What You Need to Know
 By: by Amino Science
By: by Amino Science

Methicillin-resistant Staphylococcus aureus (MRSA) is a type of staph bacteria that is resistant to several antibiotics and can cause skin infections, lung infections such as pneumonia, and other health issues. If not treated, MRSA infections can enter critical territory as sepsis, an often fatal reaction to severe infection. In hospitals, nursing homes and other health care settings, MRSA bacteria can trigger serious health problems, such as bloodstream infections, respiratory illnesses, and wound infections.
What Is MRSA
MRSA, a contagious bacterial infection, resists the common antibiotics methicillin, amoxicillin, penicillin, and oxacillin, which makes it difficult to combat. It’s such a resistant bacteria, it’s been labeled a superbug.
MRSA infection often starts out as a seemingly harmless skin sore, pimple, or boil. A staph infection can be mild, but if not treated properly can also be accompanied by serious complications such as:
- Blood poisoning (septicemia)
- Bone infection (osteomyelitis)
- Lung infection (pneumonia)
- Heart valve infection (endocarditis)
- Septic bursitis (tiny fluid-filled sacs under the skin)
- Urinary tract infection
According to a recent Centers for Disease Control and Prevention (CDC) report, more than 119,000 Americans contracted a Staphylococcus aureus (staph) infection in 2017 and close to 20,000 died.
The majority (an estimated 86%) of invasive MRSA infections are acquired in health care settings. This can be explained by the fact that three-quarters of staph infections in hospital ICUs are resistant to the antibiotic methicillin. While hospital-acquired MRSA, or HA-MRSA, is the most common type of MRSA, community-acquired MRSA, or CA-MRSA, cases are on the rise. Germ-killing soaps, hand sanitizers, and ointments have been found to considerably reduce MRSA cases in health care facilities.
The same CDC report shows that HA-MRSA rates decreased 17.1% each year from 2005-2012, but those drops tapered off between 2013 and 2016. CA-MRSA only went down 6.9% each year from 2005-2016 and rates have increased 3.9% from 2012-2017.
MRSA Infection
According to the CDC, anyone can contract MRSA on the body from contact with an infected wound or personal items that have come into contact with infected skin. The risk of MRSA infection is greater when among crowds, with skin-to-skin contact, and when sharing equipment or supplies. People who recently received inpatient medical care, as well as athletes, daycare attendees, school students, and military personnel living in barracks are at higher risk of MSRA than other individuals.
MRSA Causes
Strains of bacterium that have, due to antibiotic overuse, learned to withstand antibiotics, become resistant to these weapons of choice. Highly contagious, MRSA is spread through skin-to-skin contact and from person to object to person. The bacteria can survive for quite a while on many different surfaces and objects, like door handles, floors, sinks, taps, cleaning equipment, and fabric.
Researchers investigated how long resistant staph could survive on five materials used frequently in a hospital setting: 100% smooth cotton (clothing); 100% cotton terry (towels and washcloths); 60% cotton, 40% polyester blend (scrub suits, lab coats, and clothing); 100% polyester (drapes and clothing); and 100% polypropylene plastic (splash aprons).
They injected fabric swatches with 10,000 to 100,000 colony-forming units (CFU) of the MRSA microorganism and examined MRSA survival daily. Results showed that S. aureus survived on:
- Cotton for 4 to 21 days
- Terry for 2 to 14 days
- Polyester blend for 1 to 3 days
- Polyester for 1 to 40 days
- Polypropylene for 40 to greater than 51 days
Findings show that extensive contact control and painstaking disinfection protocols are necessary to keep MRSA from spreading.
MRSA Symptoms
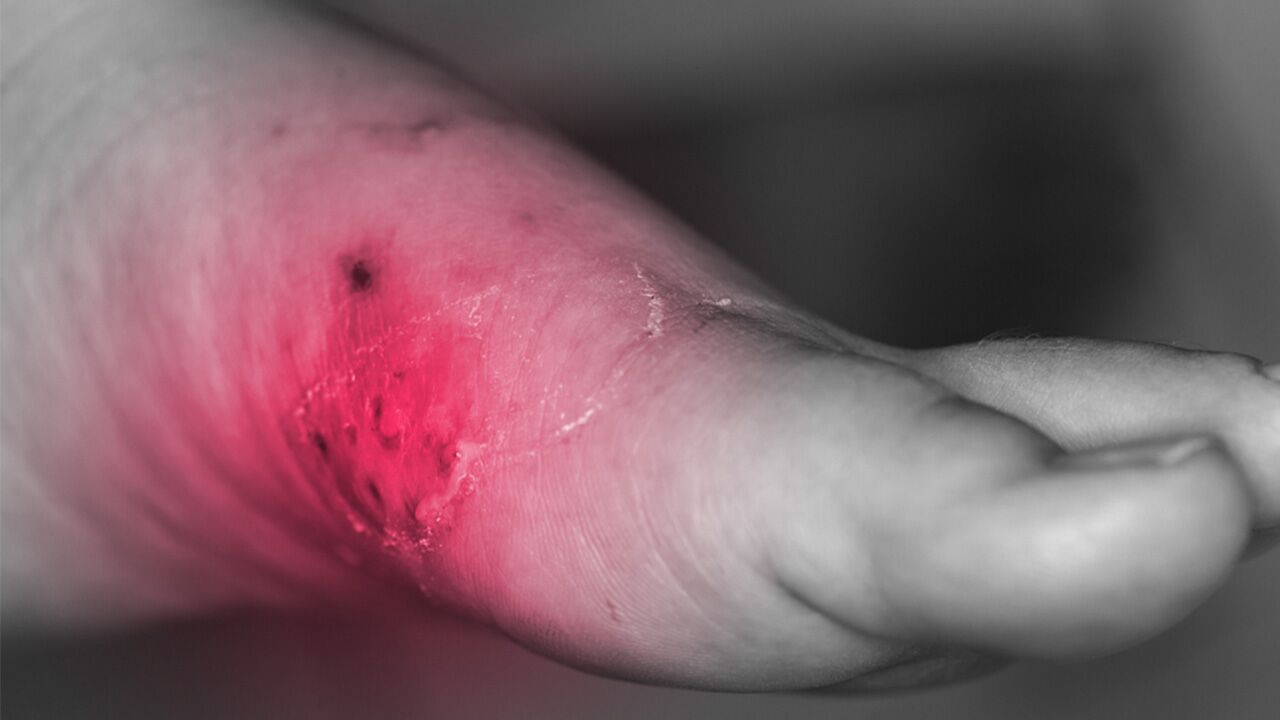
MRSA skin infections may be mistaken for spider bites or other forms of skin irritation. Most staph-related skin infections, including MRSA, look like a red bump or infected patch of skin that appears swollen, painful, warm, and full of pus or drainage. The infection might also instigate a fever.

MRSA Treatment
If you notice any signs of MRSA, such as a skin sore or boil, cover the area with a bandage until a health care provider visit can be arranged. Be sure to have everyone around you wash their hands, and contact your doctor. The latter is especially critical if indications of an MRSA skin infection are accompanied by a fever. Catching infections early on and getting care quickly can reduce the severity. People who suspect that they have an infection should not try to treat it themselves.
Once MRSA is diagnosed, treatment will vary depending on the kind of infection, the location of the infection, the severity of the symptoms, and the kind of antibiotics to which the particular strain of MRSA responds. To manage MRSA infections, clinicians may perform pus drainage from the lesion, culture and susceptibility testing of the drained material, wound care and hygiene, and antimicrobial therapy (for cases of possible cellulitis without abscess). Possible medications for MRSA skin and soft tissue infections may include clindamycin; tetracycline drugs, such as doxycycline and minocycline; trimethoprim and sulfamethoxazole; rifampin; and linezolid.
Preventing the Spread of MRSA
You can take various steps to minimize your risk of MRSA infection:
- Maintain good hand and body hygiene by washing hands frequently and your body regularly, especially after exercise.
- Clean and cover cuts, scrapes, and wounds until healed.
- Discourage sharing of personal items, including towels and razors.
- Seek advice and care as soon as possible if there is a suspected infection.
Patients should cover their wounds and keep them covered with sterile, dry bandages until they are healed. Health care professionals will offer instructions on caring for surgical wounds properly. The pus from infected wounds can act as a carrier of MRSA, so it is important to keep the wound covered so that the infection does not spread to others. Discard all used bandages and tape in the trash.
People affected by MRSA, as well as family, friends, associates, colleagues, and others in close contact, should wash their hands often with soap and water or use an alcohol-based hand rub. This is especially critical if someone changes the bandage or touches the infected wound.
It is also important not to share personal items, such as towels, washcloths, razors, or clothing. Wash and dry infected sheets, towels, and clothes, and be sure to wash your hands after touching contaminated fabrics.
To explore the prevention of MRSA infections in institutional settings, the Department of Health and Human Services funded a study called the REDUCE MRSA trial to test three MRSA prevention methods:
- Giving germicidal ointment and soap to all patients in the intensive care unit
- Giving these items just to MRSA patients
- Providing basic care
The study determined that germ-killing soap and ointment helped protect ICU patients more effectively than the other strategies. This methodology can be employed with all patients in intensive care units to cut the number of infections in the bloodstream by as much as 44%. In addition, it can contribute to the decrease of MRSA in intensive care units.
As Carolyn M. Clancy, M.D., director of the Agency for Healthcare Research and Quality (AHRQ), explained, “Patients in the ICU are already very sick, and the last thing they need to deal with is a preventable infection. This research has the potential to influence clinical practice significantly and create a safer environment where patients can heal without harm.”
To help boost overall wellness, a safeguard against all types of infection, consider taking a daily amino acid supplement.

Up to 25% off Amino
Shop NowTAGS: conditions
Join the Community
Comments (0)
Most Craveable Recipes



 833-264-6620
833-264-6620



















