How to Treat and Prevent Coronary Artery Disease
 By: by Amino Science
By: by Amino Science
Coronary artery disease, or coronary heart disease, affects millions of Americans. In fact, it’s the most prevalent type of heart disease and the leading cause of death in the United States. However, while this monstrous health problem is responsible for the deaths of one in four Americans each year, it’s also largely preventable. So read on to discover how you can treat and even prevent coronary artery disease.
What Is Coronary Artery Disease?
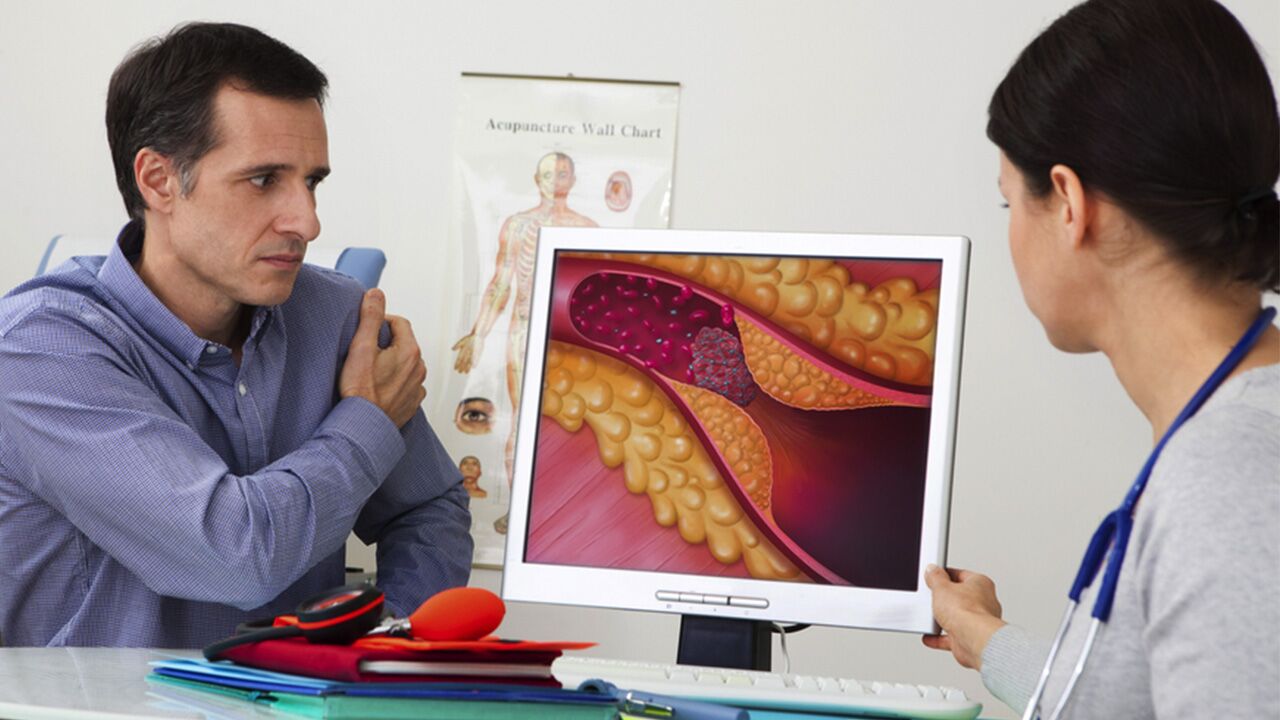
Coronary artery disease is the result of plaque buildup (atherosclerosis) in the blood vessels that supply blood to the heart. In people with this condition, plaque lines the walls of the coronary arteries until the flow of blood is restricted and the heart doesn’t get enough blood—a condition known as ischemia. This restriction of blood flow to the heart can eventually damage the heart muscle, reducing its ability to pump blood efficiently.
Because coronary artery disease develops over time, symptoms depend on the stage of the condition and may be nonexistent, mild, or severe. In the most extreme cases, plaque buildup can suddenly rupture, forming a blood clot when blood platelets attempt to repair the damage. If the blood flow in the artery becomes completely blocked by this process, a myocardial infarction, or heart attack, occurs.
In most people, symptoms of coronary artery disease don’t appear until later in life. However, children and teenagers may sometimes develop the condition as well.

Coronary Artery Disease Risk Factors
Coronary artery disease is associated with a host of risk factors, many of which can be reduced with lifestyle changes. Unfortunately, though, some factors can’t be changed. These include:
- Sex: According to the National Heart, Lung, and Blood Institute (NHLBI), men are more likely to develop obstructive coronary artery disease (narrowed arteries due to plaque), and women are more likely to develop nonobstructive coronary artery disease (arteries with plaque that doesn’t obstruct blood flow).
- Age: In men, the risk of developing coronary artery disease begins to increase after age 45. In women, the risk increases after menopause.
- Family history: People with a family history of coronary artery disease have a higher chance of developing the condition.
- Race: Coronary artery disease is the leading cause of death in most groups, regardless of race. However, for Asian Americans, Pacific Islanders, and American Indians, heart disease is second only to cancer.
Again, however, the vast majority of coronary artery disease risk factors are within our control. Some of these factors include:
- Smoking
- High cholesterol
- Sedentary lifestyle
- Elevated body mass index (BMI)
- High blood pressure
- Diabetes
- Chronic stress
- Sleep apnea
- Heavy alcohol use
Coronary Artery Disease Symptoms
As mentioned, the symptoms people experience with coronary artery disease depend on the stage of the disease. Sometimes the first symptoms noted are mild episodes of shortness of breath and chest pain (angina) with activity. But some people may not experience any symptoms until they have an episode of severe chest pain, or even a heart attack. And sometimes coronary artery disease causes no symptoms.
When this happens, it’s known as silent coronary artery disease. Unfortunately, this particular manifestation of coronary artery disease may not be diagnosed until it’s progressed to the point where a person begins to show signs of having a heart attack, heart failure, or irregular heartbeat (arrhythmia).
Acute signs of coronary artery disease, such as may occur during a heart attack, include:
- Shortness of breath
- Angina
- Cold sweats
- Dizziness
- Lightheadedness
- Neck pain
- Nausea
- Sleep disturbances
- Weakness
Symptoms of chronic coronary artery disease may include:
- Angina
- Anxiety
- Neck pain
- Fatigue
Diagnosing Coronary Artery Disease
Coronary artery disease is diagnosed based on personal and family history; risk factors; physical exam; blood tests to measure levels of certain fats, cholesterol, blood sugar, and proteins; and diagnostic procedures. Common tests performed in the diagnosis of coronary artery disease include:
- Chest x-ray: A chest x-ray may be the first test performed, as it’s able to identify overt abnormalities in the shape and size of the heart, lungs, and blood vessels.
- Electrocardiogram: An EKG (or ECG) is a painless procedure that’s also the most commonly used test to screen for heart problems. Used to record the electrical activity of the heart, an EKG can detect arrhythmias, current or previous heart attacks, and the likelihood of coronary artery disease.
- Echocardiogram: This ultrasound procedure, which is also referred to as an echo, may be recommended in the face of abnormal EKG results. The test uses sound waves to detect structural abnormalities in the heart.
- Stress test: A cardiac stress test uses either exercise or medication (that mimics exercise) to measure the heart’s response to stress. The test can identify abnormalities in blood pressure and heart rate and rhythm as well as symptoms such as shortness of breath and chest pain.
- Cardiac catheterization: This is an invasive procedure that may be performed if preliminary testing or symptoms lead your physician to suspect you have coronary artery disease. During the procedure, a flexible tube called a catheter is threaded to the heart, where dye is injected and an imaging procedure called a coronary angiography is performed to look for areas of blockage as the dye moves through the heart and its major vessels.
Treating Coronary Artery Disease
Treatment of coronary artery disease depends on several factors, including the severity of the disease, a person’s current health status, and whether they have any complicating health conditions. That being said, treatment may include:
- Lifestyle changes
- Medications
- Procedures
Lifestyle Changes
The same lifestyle changes recommended to prevent coronary artery disease are also used to help treat it. And for many people with only early signs of the condition, lifestyle changes may be all they need. Typical lifestyle changes recommended for the prevention and treatment of coronary artery disease include:
- Eating a heart healthy diet
- Quitting smoking
- Getting regular exercise
- Maintaining a healthy weight
- Managing stress
In fact, controlling the risk factors for coronary artery disease has even been shown to help reduce the risk of heart disease by more than 80%.
Medications
If lifestyle changes aren’t enough, your doctor may also recommend medication to help relieve symptoms, lower cholesterol or blood pressure, or prevent blood clots. Some of these medications include:
- Cholesterol-lowering drugs (statins)
- Antiplatelet drugs (aspirin)
- Beta blockers (metoprolol)
- Calcium channel blockers (diltiazem)
- Angiotensin-converting enzyme (ACE) inhibitors (lisinopril)
- Angiotensin II receptor blockers (ARBs) (valsartan)
Procedures
For people in the more severe stages of coronary artery disease, lifestyle changes and medication may still not be enough. In these cases, surgery will be required. This may take the form of a coronary angioplasty to widen a blocked artery by inflating a tiny balloon or placing a wire mesh tube known as a stent or a coronary artery bypass graft, which involves using healthy arteries from the chest wall or veins from the legs to bypass blocked coronary arteries.
How to Prevent Coronary Artery Disease
By far, the best way to treat coronary artery disease is to prevent it before it starts. And as we’ve just discussed, a few simple lifestyle changes can reduce your risk by more than 80%.
Along with stopping smoking (or avoiding secondhand smoke), losing weight, getting regular exercise, and working on reducing your stress with techniques like deep breathing, meditation, and yoga, there’s no better way to prevent coronary artery disease than eating a heart-healthy diet.
If you’re looking for ways to get the most benefits out of your diet, think about including plenty of:
- Lean proteins
- Green leafy vegetables
- Fatty fish
- Whole grains
- Olive oil
- Fruits
- Beans
- Nuts
Taking supplemental amino acids has also shown promising benefit for the prevention and treatment of coronary artery disease.
One study showed that nursing-home patients who had suffered from coronary artery disease or a femoral fracture received either 4 grams of essential amino acids twice a day for 8 weeks or a placebo made up of the same number of calories. Before and after the study researchers measured symptoms of depression, took a nutritional panel and amino acid profile, determined muscle strength with a hand grip test, and assessed daily activity levels and quality of life. Results indicate that elderly patients who took essential amino acids were less depressed, more physically active with greater muscle strength and nutritional status, and enjoyed improved quality of life.
On the heels of this research amino acid scientists developed a supplement called Life to help strengthen both heart and muscle health. You can find out more about Life here.
While certain coronary artery disease risk factors—such as family history, age, and sex—can’t be changed, the majority can be decreased, or even eliminated. So speak with your health care provider, find out what your risks are, and make changes as necessary. Your heart will thank you.


Up to 25% off Amino
Shop NowTAGS: conditions
Join the Community
Comments (0)
Most Craveable Recipes




 833-264-6620
833-264-6620



















