Sickle Cell Anemia: Cause, Symptoms and Treatment
 By: by Amino Science
By: by Amino Science
Millions of Americans have a condition called anemia in which they either don’t produce enough red blood cells or their red blood cells don’t function properly. Red blood cells carry oxygen, and the lack of properly functioning red blood cells leads to a lack of oxygen flow throughout the body, including to vital organs.
Anemia is very common, and there are multiple types of anemia. It can be brought on by a deficiency of iron in the diet, it can be due to an autoimmune condition like pernicious anemia, or it can be inherited, like sickle cell anemia. Sickle cell anemia, or sickle cell disease, affects millions of people worldwide and an estimated 100,000 Americans.
What Is Sickle Cell Anemia?
According to the American Society of Hemotology, between 70,000 and 100,000 Americans have sickle cell anemia (SCD). This blood disorder appears more commonly in certain ethnicities.
- African-Americans (1 in 12 carries a sickle cell gene)
- Hispanic-Americans from Central and South America
- People of Middle Eastern, Asian, Indian, and Mediterranean descent
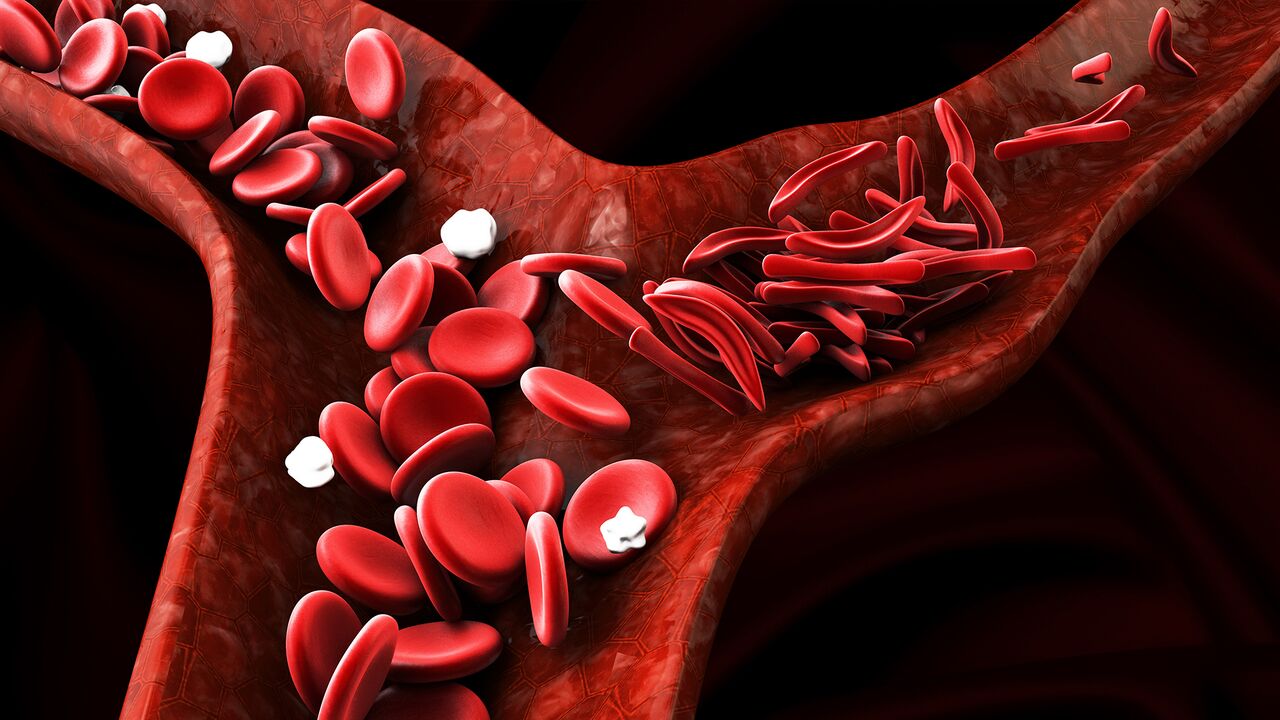
People with sickle cell anemia, or sickle cell disease, produce red blood cells like everyone else, but due to abnormal hemoglobin, their red blood cells do not function properly. Instead of healthy, round, red blood cells, their red blood cells are misshapen and take the form of a sickle, or crescent moon.
Normal red blood cells are flexible and flow throughout the body, easily carrying oxygen through blood vessels to organs and tissue. Sickle cells, however, cannot move so easily and often get stuck inside blood vessels and cause blockages. These blockages prevent blood and oxygen from getting to various parts of the body.
What Causes Sickle Cell Disease?
Sickle cell anemia is an inherited disease. According to the Centers for Disease Control and Prevention (CDC), an individual with sickle cell anemia inherited a hemoglobin gene called a sickle cell trait from his or her parents. Those who inherit the gene from only one parent may have sickle cell trait but usually do not develop sickle cell anemia. People who inherit the gene from both parents have a greater risk of developing sickle cell anemia.
If someone has inherited sickle cell trait but never develops sickle cell anemia, he or she can still pass the trait onto his or her own children. If you are unsure if you carry the sickle cell gene, you can take a blood test to check for the gene before having children.
Symptoms of Sickle Cell Disease
Signs of sickle cell disease typically don't originate until the first year of life because of the hemoglobin generated by the developing fetus. This fetal hemoglobin prevents red blood cells from sickling. After 5 months old, fetal hemoglobin is no longer produced in red blood cells, and sickling and symptoms begin.
The disorder frequently manifests as anemia, which is marked by a low number of red blood cells, frequent infections, and chronic pain. Other symptoms include:
- Fatigue
- Severe pain
- Swelling of the hands and feet
- Arthritis
- Leg ulcers
- Liver congestion
- Pooling of blood in the spleen
- Vision problems
- Bone and joint damage
Pulmonary hypertension (high blood pressure in the lungs) is a potential complication of sickle cell anemia that results in shortness of breath and fatigue. The condition can be fatal and requires immediate medical care. Because sickle cell disease can also trigger a stroke, symptoms such as numbness or weakness in the face or side of the body, visual troubles, or difficulty speaking should also be watched for.

What Is a Sickle Cell Crisis?
While it is common for sickle cell patients to experience episodes of pain, sometimes the pain becomes so severe that it is considered a sickle cell crisis. A sickle cell crisis, or a pain crisis, occurs when the sickled cells can’t pass through small blood vessels and end up creating a blockage. The blockage cuts off blood flow and oxygen to part of the body, creating a painful episode that can last from hours to days and can potentially cause organ damage, particularly in the spleen, kidneys, brain, and lungs.
A sickle cell crisis, as well as a lung infection, can induce acute chest syndrome that makes it difficult to breathe and incites chest pain and fever. Some episodes can be treated with pain medication or antibiotics, while others may be severe enough to warrant a trip to the emergency room.
Common sickle cell crisis symptoms include:
- Pain in the:
- Pain that is:
- Throbbing
- Stabbing
- Sharp
- Dull
- Headache
- Dizziness
- Extreme fatigue
- Weakness
Certain factors are thought to trigger a sickle cell crisis, such as dehydration. The CDC recommends sickle cell patients take the following precautions to help prevent a sickle cell crisis.
- Drink plenty of fluids
- Stay at a comfortable temperature, don’t let yourself get too hot or too cold
- Avoid high altitudes such as flying or mountain climbing
- Avoid low oxygen exposure such as intense exercise
Diagnosing Sickle Cell Anemia
According to the Mayo Clinic, all babies born in a United States hospital are automatically tested for the inherited sickle cell gene as part of a newborn screening. If the test is negative, then it is determined that the baby is not at risk for sickle cell anemia. If the test is positive, then further testing can be done to determine if the baby inherited two sickle cell genes, one from each parent, and the likelihood of developing sickle cell anemia.
If older children, teens, or adults were not tested as newborns and would like to be tested, a simple blood draw will determine if they have the sickle cell gene and if so, how many. If the results are positive, then the physician will likely refer the patient to a genetic counselor knowledgeable about sickle cell anemia, the chances of developing it, and the likelihood of passing it on to the patient’s children.
Treating Sickle Cell Anemia
Sickle cell anemia treatment takes many forms and is often dependent on the age of the patient. Exciting research is underway, as scientists are currently studying gene therapy in the hopes of being able to one day change or replace the gene responsible for the disease. Until then, common treatments include medications, vaccinations, blood transfusions, and bone marrow transplants.
Medications
A variety of medications may be used to treat sickle cell anemia. These include:
- Antibiotics: Children with sickle cell anemia are at a greater risk of life-threatening infections and may be prescribed antibiotics for the first few years of life.
- Pain relievers: Physicians may prescribe pain relievers to help alleviate the painful episodes associated with sickle cell anemia.
- Hydroxyurea (Droxia, Hydrea): This drug helps prevent the formation of sickle cells in newborns, decreases painful episodes, and may reduce the need for blood transfusions.
Vaccinations
Those with sickle cell anemia, particularly children, have a higher risk of severe bacterial and viral infections. In addition to the recommended vaccinations for newborns and children, additional vaccines may be suggested for children and adults with sickle cell anemia. These may include the pneumonia vaccine and an annual flu shot.
Blood Transfusions
A blood transfusion is sometimes used to help relieve symptoms for those with severe anemia. A blood transfusion involves a sickle cell anemia patient receiving blood from someone with healthy red blood cells. This increases the number of healthy red blood cells in the sickle cell patient and helps relieve their symptoms by boosting blood and oxygen flow throughout the body.
However, in addition to increasing the number of red blood cells, the level of iron in the sickle cell patient’s blood may also increase. Excess iron in the blood can be damaging to organs. Treatment to reduce iron levels may be necessary to keep the sickle cell patient at a healthy iron level.
Bone Marrow Transplants
A bone marrow or stem cell transplant may be recommended for those who have severe symptoms of sickle cell anemia. The sickle cell patient will first undergo radiation or chemotherapy to destroy bone marrow stem cells. Next, healthy stem cells are injected into the patient’s bloodstream to replace the bone marrow that has been damaged. Once in the bloodstream, the healthy stem cells should begin making new blood cells. Before a patient can have a bone marrow transplantation, a donor must be found who does not have sickle cell anemia. Siblings are often a match.
Amino Acids
In 2017, the American Journal of Healthy-System Pharmacy reported that the FDA approved the amino acid L-glutamine for the treatment of sickle cell anemia in patients 5 years and older. Amino acids are essentially the building blocks of a healthy body. They help the body form protein and make chemicals that are critical to healthy organ function, including brain function.
The FDA approved L-glutamine after a study showed that patients being treated with this amino acid experienced fewer episodes of sickle cell pain and had fewer hospitalizations than those treated with a placebo. Although L-glutamine has been shown to have positive effects for some sickle cell anemia patients, it’s best to take a balanced mixture of all essential amino acids to make sure that the blood concentration of amino acids is optimal. Patients thinking of using amino acids should consult their health care provider first, especially if there is an underlying condition like sickle cell anemia present.



 833-264-6620
833-264-6620


















