By: by Amino Science
By: by Amino Science
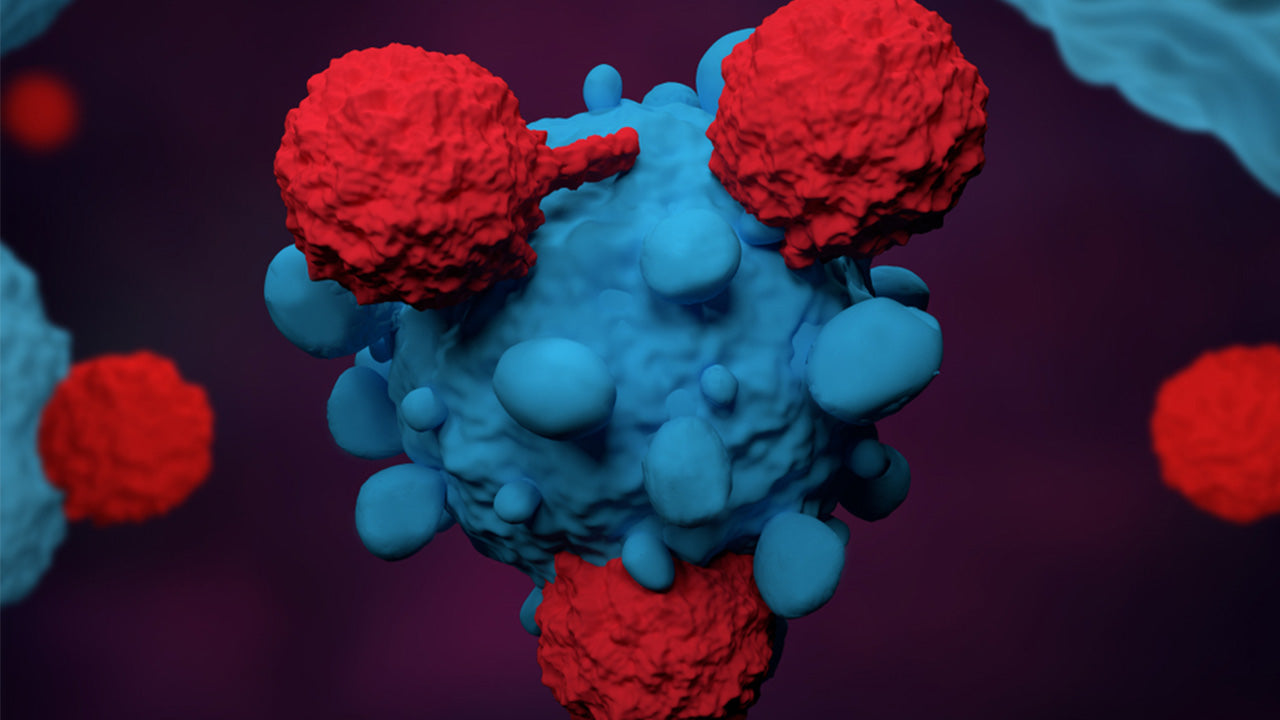
You may have heard vaguely about the importance of T-lymphocyte or T-cells in your immune system, but how do they function? And what do they have to do with amino acids? We break down the science so that if ever you hear your T-cells are too high or too low, you'll know what the doctor is talking about.
A lymphocyte is a type of white blood cell, and each white blood cell has a specific role to play in the body's immune function. Like all blood cells, T-lymphocytes come from haematopoietic stem cells, which are stem cells in our bone marrow. They work to fight infections and various types of cancer cells in an adaptive immune system, also referred to as an acquired immune system. Our adaptive immunity uses T-cells and B-cells (B-lymphocytes, also derived from bone marrow) to battle organisms and intracellular pathogens that slip through the frontlines of our bodies' defenses.
T-cells work in cell-mediated immunity. While we're born with other innate immune cells like dendritic cells, basophils, neutrophils, and macrophages (which are also deployed in emergency immune responses), T-cells and B-cells launch a more sophisticated and targeted attack.
Both T-cells and B-cells are specialized cells that we earn by surviving in our environments. These cells tend to live longer than innate immune cells, and they are also the cells that allow for vaccinations to work due to their ability to learn, adapt, and grow stronger.
B-cells mature in our bone marrow, whereas T-cells travel first to the thymus gland and become thymocytes, which is where they get their "T," and continue to mature and differentiate. Our thymus glands shrink as we age, making T-cell expansion more and more vital as we grow older.
Immunotherapy treatments for multiple forms of cancer, including cancers of the bloodstream like lymphoma and leukemia, rely on T-cells. T-cells are less likely than B-cells to mutate into liquid cancers like chronic lymphocytic leukemia or B-cell lymphoma, and T-cells can also be engineered into chimeric antigen receptors, able to identify specific proteins on tumor cell membranes for a surgical strike against cancer.
There are two major types of T-cells: helper T-cells, which stimulate B-cells to create antibodies, and killer T-cells, which mercilessly strike out any compromised or infected cell they find.
Taking advantage of this ability to target cells, researchers have developed anti-cancer drugs to enhance this form of autoimmunity against cancers like melanoma and lung cancer, disrupting the surface marker evasions these cells employ to sneak into the body and activating the surface receptors of T-cells to focus them on cancer elimination.
Further T-cell specifications break down into five types of T-cells.

Thymic, or T-cell activation, is closely linked to our amino acids. Most of our lymphocytes, including T-cells, move through the lymph nodes and other lymphatic organs like the tonsils and spleen, but they can't do so unaided. There are amino acids necessary for this immune response.
Glutamine is a nonessential hydrophilic amino acid that is coupled with naive T-cell activation and linked to the amino acid transporter ASCT2. Researchers have found that inflammatory T-cell responses rely on amino acid transporter ASCT2 and come with a rapid glutamine uptake. Though it's still not largely understood, it's nevertheless clear that glutamine plays a role in the immune response necessary to defeat deadly pathogens.
Methionine is an essential amino acid that researchers have identified as necessary for the synthesis of new proteins and muscle and for the methylation of RNA and DNA, which drives T-cell proliferation and differentiation. Essential amino acids are those our bodies cannot make independently, and so must be consumed in the proper amount via food sources or supplementation.
Again, the amino acid transporters that are tasked with the uptake of essential amino acids like leucine are attached to the development, maintenance, and activation of T-lymphocytes. This 2017 review looked at LAT1 (L-leucine transporter) along with ASCT2 (L-glutamine transporter) and GAT-1 (γ-aminobutyric acid transporter-1) and found that they are important for the fate decisions and determinations of memory T-cells and other lymphocytes. The researchers also suggested that manipulation of the amino acid transporter-mTORC1 axis could help manage inflammatory and autoimmune diseases tied to T-cell-based immune responses.
The best way to ensure you have enough of these amino acids helping out your T-cells is to supplement with a targeted essential amino acid supplement.
T- and B-lymphocytes work hand-in-hand to fight disease and infection, but sometimes they are forced out of order in circumstances of illness. Doctors can often use a blood count of overall lymphocyte content to determine whether or not there is something afflicting your immune system. If your lymphocyte count is too high or too low it could indicate the following diseases and disorders.
A low lymphocyte count is known as lymphocytopenia, and can arise if your body isn't producing sufficient lymphocytes, if the lymphocytes you do produce are being destroyed, or if they are trapped in places like your spleen or lymph nodes. With a lower lymphocyte count you are more at risk of developing infections, and that low count is often associated with the following conditions:
A high lymphocyte count, called lymphocytosis, is also an indication that your immune system is under attack from an overwhelming disease or illness, such as the following:

Without T-lymphocyte cells standing as the second line of defense against diseases, viruses, and cancer cells, our immune systems would collapse. Scientists are hard at work not only trying to understand the utilization pathways of these cells, but also striving to improve their numbers and recruit them in the battle to cure cancer. Closely tied to the movement and usage of our amino acids, T-cells are the special ops team keeping each of us alive.