What Is COPD and How Can Essential Amino Acids (and Other Remedies) Help?
 By: by Amino Science
By: by Amino Science

Chronic obstructive pulmonary disease (COPD) is the third leading cause of death in the United States, with almost 16 million Americans reporting the diagnosis and the Centers for Disease Control and Prevention (CDC) estimating that the total number may be much higher. COPD is also expected to become the third leading cause of death worldwide by 2020. While there’s currently no known cure, the symptoms of COPD can be managed and lung function even improved. However, before discussing the various treatments available for this chronic and sometimes debilitating condition, it might be helpful to first ask ourselves, what is COPD?
What Is COPD?
COPD refers to a group of progressive lung diseases—the most common of which are chronic bronchitis and emphysema—that make it difficult for you to take in the oxygen you need and breathe out the carbon dioxide you don't.
In the case of chronic bronchitis, the bronchial tubes become inflamed and less efficient in expelling mucus, which can result in your airways becoming clogged. This in turn may result in limited airflow that makes it harder to breathe.
With emphysema, the delicate air sacs of the lungs become damaged. When this occurs, the walls of the air sacs begin to expand, which causes them to weaken and eventually rupture. This not only decreases the amount of air the lungs can move but also causes them to grow in size.
This expansion of the lungs is why some people with emphysema develop a barrel chest in the later stages—their rib cages have actually widened to accommodate their chronically overinflated lungs.
What Causes COPD?
In the United States, tobacco smoke (from cigar, pipe, and cigarette smoking and secondhand smoke exposure) is the most common cause of COPD. Other risk factors include long-term exposure to environmental contaminants such as dust, air pollution, and chemicals in the home and workplace and genetic factors such as alpha-1 antitrypsin (AAT) deficiency.

Symptoms of COPD
COPD symptoms may progress for years before they become severe. In fact, in the early stages of the disease, symptoms may be so mild as to be easily dismissed. However, the earlier the disease is diagnosed, the more successful treatment will be. Therefore, it’s important to pay attention to these early warning signs:
- Intermittent mild cough
- Occasional shortness of breath
- Frequent throat clearing
As symptoms progress, you may also begin to notice the following:
- Increased shortness of breath
- Chronic cough
- Chest tightness
- Wheezing
- Frequent respiratory infections
Diagnosis of COPD
As soon as you begin to notice symptoms, you should make an appointment to speak with your health care provider. You and your provider will then be able to discuss your symptoms, your family and medical history, and any exposures you may have had.
Your provider may also order several tests to assist in diagnosing your condition. These include:
- Pulmonary function tests
- Chest x-ray
- Blood tests
Medical Treatment for COPD
If your health care provider determines your symptoms warrant a diagnosis of COPD, they may place you on bronchodilators, which are considered first-line treatment for COPD.
Bronchodilators work by relaxing the muscles around the airways, thus helping to widen the airways and make it easier to breathe. Depending on the severity of your symptoms, short- or long-acting bronchodilators may be prescribed.
As the name suggests, short-acting bronchodilators are designed to provide quick relief of symptoms, lasting from 3 to 6 hours. These types of bronchodilators are used in less severe cases of COPD and should be used only when needed.
Examples of short-acting bronchodilators include:
- Albuterol
- Levalbuterol
- Ipratropium
By contrast, long-acting bronchodilators are intended to control ongoing symptoms. With effects lasting up to 12 hours, these medications are designed for use in those with more severe forms of COPD.
Examples of long-acting bronchodilators include:
- Salmeterol
- Formoterol
- Tiotropium
In the most severe stages of COPD, you may develop low oxygen levels and may be prescribed oxygen therapy in the form of supplemental oxygen.
However, help for COPD is not limited to these conventional treatments. In fact, there are a host of additional therapies that show promise in easing the symptoms of COPD. And one of the most important available today is undoubtedly essential amino acids.
How Can Essential Amino Acids Help COPD?
One of the most common problems among people suffering from COPD is loss of skeletal muscle mass. This potentially debilitating byproduct of COPD can contribute to even greater COPD symptoms due to the effects of muscle loss on exercise tolerance.
While there are a number of reasons for this loss of muscle, including inflammation, loss of appetite, and decreased levels of physical activity, the extent of muscle wasting is directly related to mortality from COPD.
Essential amino acids are the most potent dietary stimulators of muscle protein synthesis (the process of building muscle), and supplementing with these building blocks of life has been shown to effectively combat muscle loss and help increase exercise tolerance.
For example, in a recent study, patients with moderate to severe COPD were given either a free essential amino acid mixture (composed of separate amino acids, as opposed to the strings of amino acids found in complete proteins) or a similar mixture of both essential and nonessential amino acids in the same profile as that found in whey protein.
The results showed that subjects who ingested the free essential amino acids had a net protein gain that was an astounding 49% higher than those who consumed amino acids that were included as part of a complete protein.
Another study showed that COPD patients treated with essential amino acids had significant increases in fat-free mass (lean body mass minus remaining fat), muscle strength, and oxygen saturation.
In yet another study, it was demonstrated that a combination of the antioxidant coenzyme Q10 (CoQ10) and the amino acid creatine resulted in increased lean body mass and exercise tolerance and decreased shortness of breath and COPD exacerbations.
Finally, patients treated with N-acetyl cysteine (NAC), the precursor to the amino acid cysteine and, by extension, the potent antioxidant glutathione, have been shown in studies to have significantly and consistently fewer exacerbations of both chronic bronchitis and COPD.
Clearly, the use of essential amino acids may prove beneficial to those suffering from COPD. We recommend a balanced formula of essential amino acids, such as Life. However, even further benefits may be obtained by incorporating the following additional natural remedies into your management regimen.
Nine More Natural Remedies to Help Manage Your COPD Symptoms
1. Quit Smoking
If you’ve been diagnosed with COPD—and even if you haven’t—the first thing you need to do is quit smoking (if you smoke) and avoid secondhand exposure to anyone else's cigar, pipe, or cigarette smoke.
While this may be admittedly easier said than done, tobacco smoke is the leading cause of COPD in the United States, and continued smoking will only lead to worsening of symptoms.
2. Practice Your Breathing
According to the American Academy of Family Physicians (AAFP), patients with COPD who practice breathing exercises experience greater improvements in exercise capacity than those who receive standard treatment only.
Although some pulmonary rehabilitation programs offer breathing exercises that make use of breathing devices, there’s one exercise you can practice on your own that’s been proven to decrease shortness of breath: pursed lip breathing.
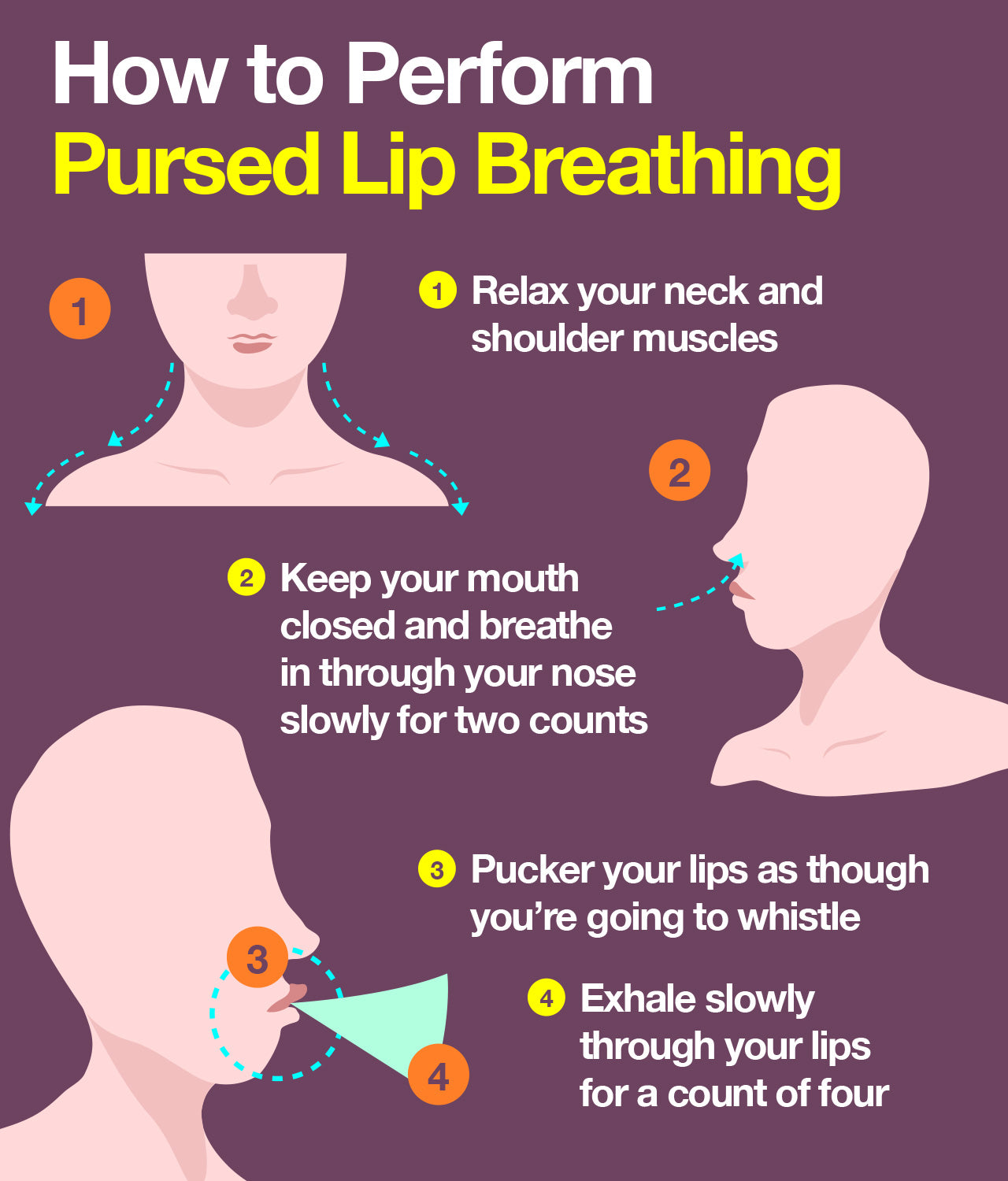
Practicing this technique daily can result in:
- Improved breathing patterns
- Decreased shortness of breath
- General relaxation
3. Add Vitamin D and Antioxidants
People with COPD often suffer from vitamin D deficiency, which is associated with increased susceptibility to lung infections. A recent meta-analysis also demonstrated that low levels of vitamin D are associated with higher risk and greater severity of COPD.
Low levels of vitamins C and E have also been associated with increased levels of wheezing, mucus, and shortness of breath.
One recent study also showed that vitamin C reduces the risk of developing COPD regardless of smoking history. And another study conducted by researchers at Cornell University and Brigham and Women's Hospital showed that regular, long-term use of vitamin E by women may help reduce their risk of developing COPD.
4. Avoid Mucus-Producing (and Thickening) Foods
Many of us may not be aware that certain foods actually contribute to the body’s production of mucus and others cause existing mucus to become thicker, both of which may lead to issues in people suffering from symptoms of COPD. Some examples of these foods are:
- Red meat
- Dairy products
- Eggs
- Potatoes
- Corn products
- Pasta
- Sweets
By contrast, there are also foods that contribute to lower levels of mucus. Some examples of these foods are:
- Salmon
- Pumpkin seeds
- Pineapple
- Grapefruit
- Honey
- Ginger
- Garlic
- Cayenne pepper
5. Stay Hydrated
In addition to using food to help manage mucus production, it’s especially important for people with COPD to stay well hydrated. This is because proper hydration helps the body thin mucus, which not only makes breathing easier but also helps prevent respiratory infections. In fact, health care providers generally recommend that people diagnosed with COPD drink 8 to 12 glasses of water a day.
6. Manage Stress
The challenge of living with COPD can often lead to stress. This may be noticed in the form of depression due to the inability to participate in certain activities or anxiety from sudden symptom flare-ups.
And in what can become a vicious cycle, mental health issues have also been shown to increase COPD exacerbations. For example, one study showed that depression and anxiety contributed significantly to hospital readmission rates in elderly patients with COPD.
However, people with COPD who practice meditation have reported an improved sense of well-being and better mood. This has also been borne out by clinical studies.
In fact, one study showed that a program of qigong promoted functional capacity and quality of life in older adults with COPD. Another study also demonstrated positive impacts on the emotional health of participants.
7. Try Essential Oils
Eucalyptus oil, derived from the leaves of the eucalyptus tree, has a long history of benefits to the respiratory system. Not only is it known to open the lungs' airways, but it can also reduce mucus production and break up existing mucus so that it’s easier to expel.
In a rather interesting study, cineole, the main component of eucalyptus oil, was shown to reduce COPD exacerbations and shortness of breath and improve lung function and health status.
And in a more recent study, patients receiving oral cineole 600 milligrams a day improved their breathing difficulties by an impressive 42.8% compared with the control group.
8. Avoid Chemicals
As stated earlier, long-term chemical exposure has been linked to the development of COPD. To reduce your chances of developing the disease or experiencing progression of current symptoms, try to avoid the use of chemicals in and around the home. These types of products may include:
- Cleaning products
- Herbicides and pesticides
- Paints and varnishes
Instead, look for safer natural alternatives that will do the job just as well but not expose your sensitive lung tissue to toxic chemical fumes.
9. Keep Your Home’s Temperature Optimized
High indoor air temperatures have been associated with flare-ups of COPD symptoms. In fact, a recent study by researchers at Johns Hopkins University found that higher indoor air temperatures resulted in increased levels of breathlessness, cough, and sputum scores and increased rescue inhaler use.
As we've seen, whether you’re seeking to reduce your chances of developing COPD or already have the condition and are interested in slowing its progression, you have a number of options.
And even though the many complexities of this disease mean we still have a way to go before a cure can be declared, the combination of early diagnosis and optimal medical care via a variety of treatments, including essential amino acids, can help ensure a better quality of life and more successful outcome.


Up to 25% off Amino
Shop NowTAGS: conditions natural cures
Join the Community
Comments (0)
Most Craveable Recipes



 833-264-6620
833-264-6620



















