When It Comes to Early Treatment of Fatty Liver, Ultrasound Detection Could Be Key
 By: by Amino Science
By: by Amino Science

Experts estimate that approximately 100 million individuals in the United States meet the criteria for non-alcoholic fatty liver disease, though most of them don't know it. That's because the early stages of fatty liver are often asymptomatic, meaning that a person has no indication they do not have a healthy, normal liver until the disease has progressed into more advanced stages. A key element of reversing this trend is finding ways to incorporate screening for fatty liver into routine clinical practice. Of the methods currently available for detecting fatty liver, ultrasound stands out as a noninvasive assessment option that efficiently and reliably detects the disease.
What Is Fatty Liver?
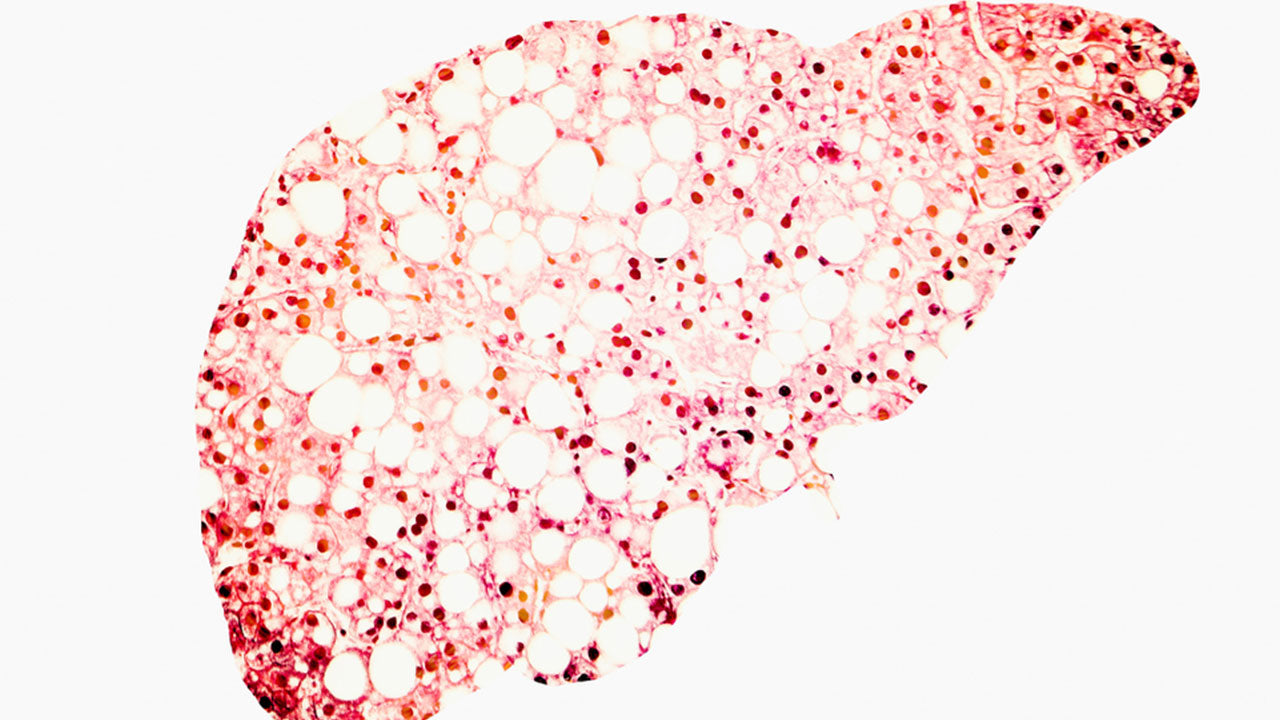
The liver, the largest internal organ, metabolizes nutrients and filters toxins from the bloodstream. It plays an especially active role not only in how your body digests fat, but also in how it produces and utilizes it. When the balance between those activities becomes skewed, fat builds up in the liver. As fat accumulates in the liver, it creates inflammation in the liver cells, which can lead to impaired liver function and scarring of liver tissue. If the disease is allowed to progress unchecked, it can ultimately progress to liver failure.
There are two primary types of fatty liver: alcoholic fatty liver disease (AFLD) and non-alcoholic fatty liver disease (NAFLD). The former refers to the development of fatty liver in individuals with high levels of alcohol use, and the latter refers to the disease when it develops without heavy alcohol consumption.
In the absence of excessive alcohol intake, the most common underlying cause of fatty liver is insulin resistance. A number of factors can impair the body's sensitivity to insulin, such as:
- Increased body weight
- Aging
- Family history of type 2 diabetes
- Large fat deposits in the abdominal area
If the body cannot appropriately detect the presence of insulin, then it increases its own insulin production. Rising levels of insulin can cause other issues such as:
- Increased blood pressure
- High triglyceride levels
- Accumulation of fat in the liver
Typically, individuals in the early stages of fatty liver disease have no perceptible symptoms. If the liver becomes sufficiently enlarged, they may begin to sense a mild ache or tenderness where it's located in the upper-right abdomen.
If individuals are able to address the insulin resistance that causes fat to build up in the liver, then it's typically possible to restore full liver health without any lasting serious consequences. However, if the condition is not detected, then it can progress to a more serious form of fatty liver—non-alcoholic steatohepatitis (NASH). This is the stage at which inflammation of the liver as well as liver fibrosis (scarring) occur. This form of fatty liver can then cause cirrhosis and even liver failure.
What Happens When Fatty Liver Progresses to Cirrhosis?
As touched on above, fatty liver usually causes no noticeable symptoms. However, once it progresses from NAFLD to NASH to cirrhosis, symptoms begin to appear. Cirrhosis demarcates the point at which liver scarring becomes quite severe. Hallmark symptoms of cirrhosis include:
- Weakness and fatigue
- Decreased appetite
- Weight loss
- Jaundice (yellowing of the eyes and skin)
- Itchiness
- Nosebleeds
- Spider veins (clusters of blood vessels that resemble spider webs)
- Confusion and difficulty focusing
- Ascites (abdominal pain and swelling)
- Edema (swelling of the legs)
- Gynecomastia
In most cases, cirrhosis develops because of a long-term viral hepatitis C infection or ongoing alcohol abuse. However, untreated NAFLD can also progress to cirrhosis.
If cirrhosis is not effectively treated, it progresses to end-stage liver disease, which will prove fatal if a liver transplant does not occur in time. While it's not possible to reverse the scarring that occurs, you can minimize its impact and prevent future scarring from taking place. The key to doing so is taking every possible opportunity to cleanse your liver and support its health and functioning. To learn more about managing a cirrhosis diagnosis, read this article.

For Early Detection of Fatty Liver, Ultrasound Could Be Key
Studies show that ultrasound images offer a reliable, efficient method for diagnosing fatty liver. According to a 2018 hospital-based, cross-sectional study published in the Journal of International Medical Research, ultrasound's "sensitivity and specificity in detecting moderate to severe fatty liver are comparable to those of histology
Preventing NAFLD from progressing to cirrhosis and even liver failure requires effective risk stratification and the development of strategic treatment plans. In order to do that, doctors need to evaluate:
- How much fat has accumulated in the liver
- Whether the liver is inflamed, and if so, to what degree
- Whether scarring is present, and if it is, how severe
Liver biopsy has historically been the preferred method for confirming a diagnosis of fatty liver and developing a treatment plan. However, non-invasive imaging methods like ultrasound allow doctors to screen individuals who do not yet show signs of liver disease, allowing those in the early stages of NAFLD to access treatment faster.
Both B-mode ultrasonography (US) as well as ultrasound elastography (USE) can be used for this purpose. Ultrasound elastography even allows doctors to evaluate degrees of inflammation and scarring, vital pieces of information relevant to disease progression and treatment selection.
Medical professionals have determined that imaging tests like liver ultrasound have multiple advantages over both liver biopsy and blood tests to measure serum biomarkers, such as:
- Non-invasiveness
- Evaluation of a greater volume of fat accumulation in the liver
- Less variability
- More quantitive data
Ultrasonography
Conventional ultrasonography (US) is widely available, affordable, and noninvasive. Because of this, it's common for US to be the first method used to clinically evaluate fatty liver, particularly when doctors want to screen for suspected NAFLD.
Key features found on ultrasound images that indicate fatty liver disease include:
- Hepatomegaly, meaning the liver is visibly enlarged
- Increased echogenicity, indicating the surface bouncing the echo can reflect increased sound waves
- Intrahepatic vascular blurring, referring to blurred images of blood vessels in the liver
Ultrasound Elastography
Ultrasound elastography (USE), like conventional ultrasound, is widely available and relatively inexpensive. It's attracted a high level of interest due to utility as a noninvasive method of assessing liver stiffness.
The theory supporting its use is that tissue stiffness can be used as a measure of the presence and degree of liver fibrosis, which in turn indicates how far the disease has progressed.
Currently available USE methods can be divided into two general groups: first, transient elastography, an ultrasound-based technique that does not rely on images and second, and elastography techniques that do use images.

Conventional liver ultrasound and ultrasound elastography can be seen as complementary screening measures as they provide different data points, all of which can be combined to form a diagnosis and treatment plan.
Research on the Use of Ultrasound to Detect Fatty Liver
The Journal of International Medical Research study cited earlier drew its findings from the analysis of 390 health histories, 226 from patients who were diagnosed with fatty liver after master health checkups and 164 who were not. The goal was to determine whether the diagnoses of fatty liver made using ultrasound findings correlated to laboratory blood test parameters for the disease. This, then, would show whether it's valuable to include ultrasound screening for fatty liver in routine health checkups.
Patients whose ultrasound examinations showed fatty liver were classified as cases and those whose ultrasounds did not were classified as controls. Diagnostic findings from blood tests—lipid profiles
The authors found that lipid, liver enzyme, and HbA1c levels were all substantially elevated for cases compared to controls. Overall, the findings were consistent with previous studies in that they showed NAFLD to be the most common cause of high blood levels of GPT and GOT. The authors note, too, that NAFLD should not be viewed as "an isolated or random event in metabolic syndrome," but instead treated as a component of the condition. Furthermore, they state that NAFLD should be regarded as a risk factor for the development of:
They note, too, that ultrasound can help to diagnose fatty liver in patients where it could otherwise be easily overlooked due to an absence of clinical markers that would raise suspicion. For instance, individuals from South Asian countries who develop fatty liver disease often maintain lower body mass indexes than those in European and American countries with the disease. This can cause the results of blood pressure tests to be misleading, as they may show normal levels despite the presence of increased liver fat. Ultrasound screening can be used for mass screening that will identify patients who might otherwise slip through the diagnostic cracks.
Because fatty liver disease tends to be asymptomatic, developing reliable screening methods to identify high-risk NAFLD patients is of paramount importance to managing the disease. Liver biopsy is reliable for diagnostic purposes, but impractical as a screening tool. Ultrasound, however, appears to be near-equal in terms of reliability and it's far better suited for screening purposes.
How to Prevent, or Treat, Fatty Liver Disease
At this time, no medications exist for the treatment of fatty liver disease. However, it can be both prevented and treated with lifestyle changes. Depending on the underlying cause of the disease as well as a person's overall health, doctors may recommend adjustments such as:
- Limiting alcohol consumption
- Eating more nutrient-rich foods and avoiding highly processed ones
- Increasing physical activity
For individuals at risk of developing NAFLD, as well as those with NAFLD, adopting a fatty liver diet will be a crucial part of an effective treatment plan. Unsurprisingly, a central tenet of this diet is limiting consumption of both saturated and trans fats. It also involves completely cutting out alcohol, limiting salt and sugar, eating plenty of high-fiber plant foods, like whole grains and legumes, and upping your intake of fruits and vegetables.
Experts recommend the following foods as ideal components of a fatty liver diet:
- Green vegetables: Broccoli, spinach, kale, and other green vegetables can help prevent liver fat buildup while supporting weight loss and enhancing your overall health.
- Fish: Salmon, trout, tuna, and sardines contain omega-3 fatty acids that can actually lower liver fat levels and decrease liver inflammation.
- Walnuts: Like fish, walnuts contain concentrated amounts of omega-3 fatty acids, which can improve your liver disease prognosis, liver function, and health.
- Dairy: Studies show that whey protein can protect liver cells from damage linked to NAFLD.
- Olive oil: This staple of the Mediterranean diet can lower liver enzyme levels and bodyweight, perhaps due to the omega-3 fatty acids it contains.
- Green tea: Research indicates green tea can enhance liver function and decrease liver fat storage.
- Coffee: This popular beverage can prevent liver damage associated with fatty liver disease as well as lower levels of liver enzymes.
- Tofu: Soy proteins found in tofu can reduce the accumulation of fat in the liver.
There's also some evidence to support the use of certain supplements, including vitamin E, to prevent or treat fatty liver disease. Studies indicate that milk thistle, which has anti-inflammatory and antioxidant properties, can have a positive effect on liver health. And turmeric, a potent antioxidant, can quell inflammation throughout the body, which can help to reduce your risk of liver disease as well as manage liver disease. To learn more about natural methods for detoxifying the liver, read this article.
Perhaps the most consequential choice you can make to protect or improve your liver health is to supplement with amino acids. According to the work of a team of scientists based in Kyoto, Japan, taking branched-chain amino acids (BCAAs) can slow, and potentially halt, the progression of chronic liver disease. After 11 weeks, blood samples showed that rats given BCAAs had liver enzyme levels that were 22% lower than the control group. The researchers also found that levels of the CTGF protein, which correlates to liver fibrosis, were an average of 75% higher in the control group. Even more significantly, markers that indicate rates of cell death, an enzyme called caspase 3 and a protein called albumin, were 100% and 80% higher in the control group.
Studies done with human subjects support the conclusion that amino acid supplements are an effective natural method for treating liver disease.

Key Takeaways About Fatty Liver Disease and Ultrasound
Non-alcoholic fatty liver disease (NAFLD) is becoming an ever more pressing public health challenge, in part due to the fact that it remains largely asymptomatic until the later stages of the disease, and the determinants of the disease have yet to be fully understood. Once the disease reaches the later stages, in which liver fibrosis progresses toward cirrhosis, severe complications can ensue. This makes identifying a noninvasive method for detecting fatty liver disease a top clinical priority. Ultrasound has many advantages as a method for screening the general population for fatty liver disease. It's efficient, widely available, and has been shown to be as accurate as biopsies, the gold standard for diagnosing liver disease.

Up to 25% off Amino
Shop NowTAGS: conditions liver
Join the Community
Comments (0)
Most Craveable Recipes



 833-264-6620
833-264-6620



















