Breaking Out in Hives? Let’s Get Some Hives Relief!
 By: by Amino Science
By: by Amino Science
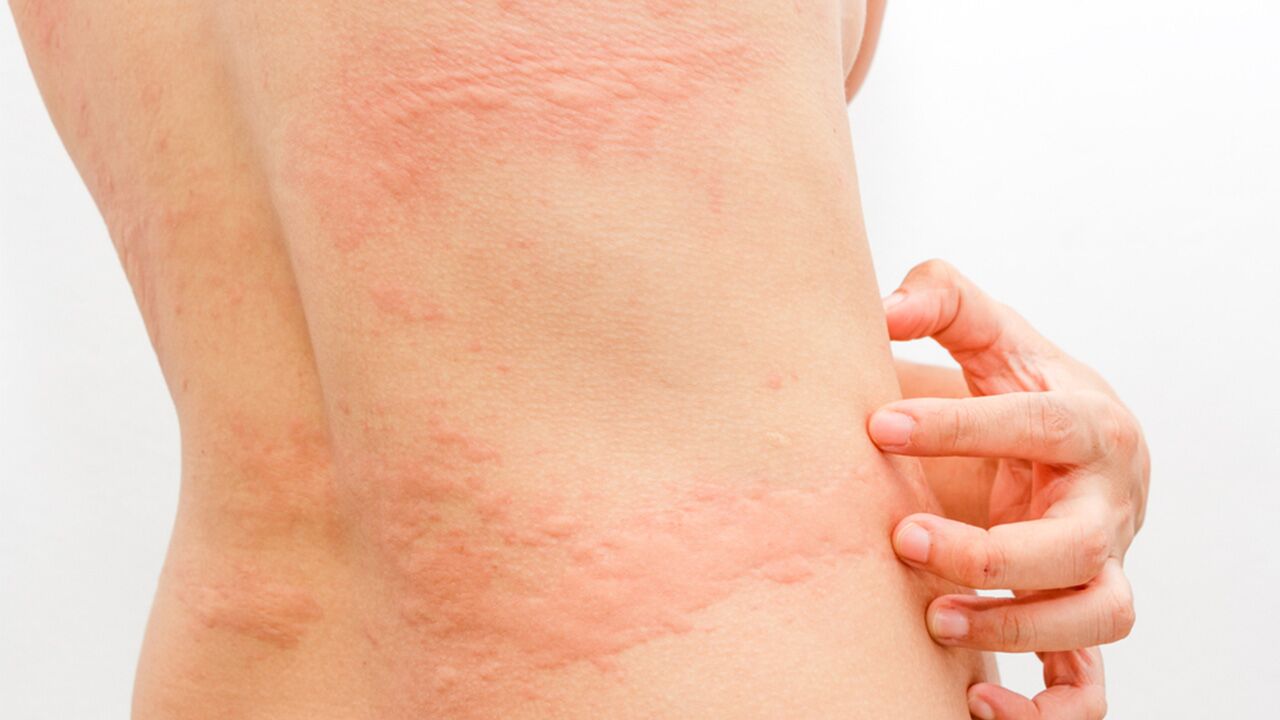
Many people experience hives, or urticaria, at some point in their lives. Thankfully, most cases are relatively mild and go away on their own. However, we realize that’s probably not much comfort when an episode of hives is accompanied by irritating symptoms like itching, burning, or stinging. So if you’re in need of a little extra help to get you over the hump, read on to discover some simple ways you can find hives relief.
What Are Hives and What Causes Them?
Hives are red bumps, or welts, that appear on the skin in reaction to histamine—a chemical released by the immune system in response to allergens, injury, or even stress. Hives may appear tiny and pale, but they can also become quite large and red and coalesce into areas called plaques. But large or small, you can always tell whether it’s hives or something else by simply pressing the center of a welt. If it turns white, you have hives.
Hives may appear suddenly and disappear a few minutes later, or they can last for hours, weeks, or months. In the majority of cases, though, hives fade within 24 hours. Moreover, episodes that last up to 6 weeks are known as acute urticaria, while those lasting more than 6 weeks are known as chronic urticaria.
Hives can have any number of different triggers, but some of the most common causes include:
- Foods: Many foods can trigger hives in people with sensitivities. Some of the best known of these triggers include shellfish, peanuts, tree nuts, eggs, citrus fruits, and milk.
- Insect bites and stings: Some people are prone to allergic reactions from the bites and stings of various insects, including mosquitoes, fleas, and spiders.
- Medications: Many medications are known to cause hives, including antibiotics like penicillin as well as aspirin, ibuprofen, codeine, and blood pressure medications.
- Allergies: Any substance that provokes an allergic reaction can cause hives as well. Some of the most common culprits are poison ivy, pollen, animal dander, and latex.
- Infections: Hives can occur with both viral and bacterial infections, including colds and strep throat. Urticaria associated with infections tends to affect children more often than adults.
- Medical conditions: Hives may be associated with autoimmune disorders, such as lupus and Hashimoto’s thyroiditis, as well as certain types of cancer, including lymphoma.
Hives can also happen in response to heat, cold, scratching, exercise, stress, skin pressure, inflammation of the blood vessels (vasculitis), or even sun exposure. Sometimes, however, the cause of hives can’t be readily identified. When this frustrating situation occurs, a diagnosis of chronic idiopathic urticaria is made.
Symptoms of Hives
Urticaria is generally one of the easiest skin conditions to identify. But if you’re unsure whether you’re experiencing hives or something else, keep an eye out for these common symptoms:
- Red or flesh-colored welts
- Raised areas that vary in shape and size
- Welts that occur alone or in patches
- Itching
- Burning
- Stinging
- Flare-ups that occur after specific triggers
While these symptoms usually don’t require medical treatment, hives can sometimes be severe and require immediate medical attention. Symptoms to watch out for include:
- Severe itching
- Lip, tongue, or eyelid swelling
- Dizziness
- Difficulty breathing
If you experience any of these warning signs, don’t hesitate to seek emergency care right away.
Conventional Treatment for Hives
As mentioned, most cases of hives are mild and disappear on their own, but sometimes symptoms are persistent or more severe and require treatment. Conventional therapy for hives generally consists of over-the-counter (OTC) and prescription drugs, including:
- Anti-itch medications: The most common treatment for hives is OTC antihistamines—medications that block the production of histamine and help reduce itching, swelling, and other allergy symptoms.
- Anti-inflammatory drugs: People experiencing chronic hives may be prescribed anti-inflammatory drugs called leukotriene modifiers to use in conjunction with antihistamines. However, if this combination isn’t successful, a short course of an oral corticosteroid such as prednisone may be required.
- Immune system modulators: In patients with chronic urticaria whose symptoms don’t respond to any of the above treatments, medications designed to suppress the immune system may be recommended.
Natural Remedies for Hives Relief
If you’re like the vast majority of people who develop hives, you may be able to avoid medications altogether and find hives relief in the form of natural home remedies. And some of the best remedies to help soothe your skin and get rid of hives are:
- Cold compresses: Grab a bag of frozen peas or some ice, wrap in a towel, and apply to the affected area for up to 10 minutes at a time to help reduce inflammation.
- Oatmeal baths and paste: Add some finely ground oatmeal, known as colloidal oatmeal, to a cool bath to help relieve itching. Alternatively—for hives affecting only a small area—you can make a paste of colloidal oatmeal and water and apply it to the affected area.
- Baking soda baths and paste: Another great anti-itch product you probably have on hand is baking soda. Like oatmeal, you can add a couple of handfuls to a cool bath or make a paste using a little water.
- Proper skin care: Stay away from substances that can be irritating to the skin, including perfumes, fragranced skin products, and harsh soaps.
- Astringents: Like cold water, astringents such as calamine lotion and witch hazel can help calm the inflammation and itch of urticaria by reducing blood flow to the skin.
- Aloe vera: The juice of the aloe vera plant has been used for centuries to treat a variety of skin ailments. If you have an aloe plant at home, try rubbing the juice from one of the leaves on your hives, or look for a product certified by the International Aloe Science Council for quality and purity. But whatever route you choose, be sure to do a skin test first to make sure you’re not allergic to the juice. After all, you don’t want to add insult to injury!
- Supplements: The antioxidant flavonoid quercetin acts as a natural antihistamine and anti-inflammatory. In fact, a recent study demonstrated that quercetin is more effective at fighting allergies than some prescription medications—with little to no side effects. Other supplements that have shown some efficacy in treating and preventing hives include vitamins B12, C, and D, anti-inflammatory amino acids, as well as omega-3 fatty acids.
As alluded to earlier, episodes of urticaria usually follow a pattern, and finding that pattern can help reduce or even eliminate symptoms. For example, some people break out in hives when they wear tight-fitting clothing. If this describes you, try wearing loose-fitting clothing instead. Or maybe you develop hives when you’re under stress or eat shellfish. If this sounds familiar, try some deep breathing exercises or meditation to reduce your stress level and skip the shellfish.
Even if you’re one of the unlucky few who’ve been diagnosed with chronic idiopathic urticaria, there might still be a trigger lurking about that you and your health care professional simply haven’t landed on. So keep your eyes open and make a note every time you break out in hives. With a little time and perseverance, you might just discover what’s triggering your episodes.


Up to 25% off Amino
Shop NowTAGS: conditions natural cures
Join the Community
Comments (0)
Most Craveable Recipes


 833-264-6620
833-264-6620



















