Pulmonary Embolism: How to Reduce Your Risk
 By: by Amino Science
By: by Amino Science
Pulmonary embolism (PE) occurs when a clump of material, most often a blood clot, gets wedged in an artery within your lungs. It can be life-threatening, but when the condition is diagnosed and treated promptly, the risk for it turning serious drops dramatically. Taking steps to prevent blood clots will help protect you against a pulmonary embolism and lower your risk of facing a medical emergency.
What Is Pulmonary Embolism?
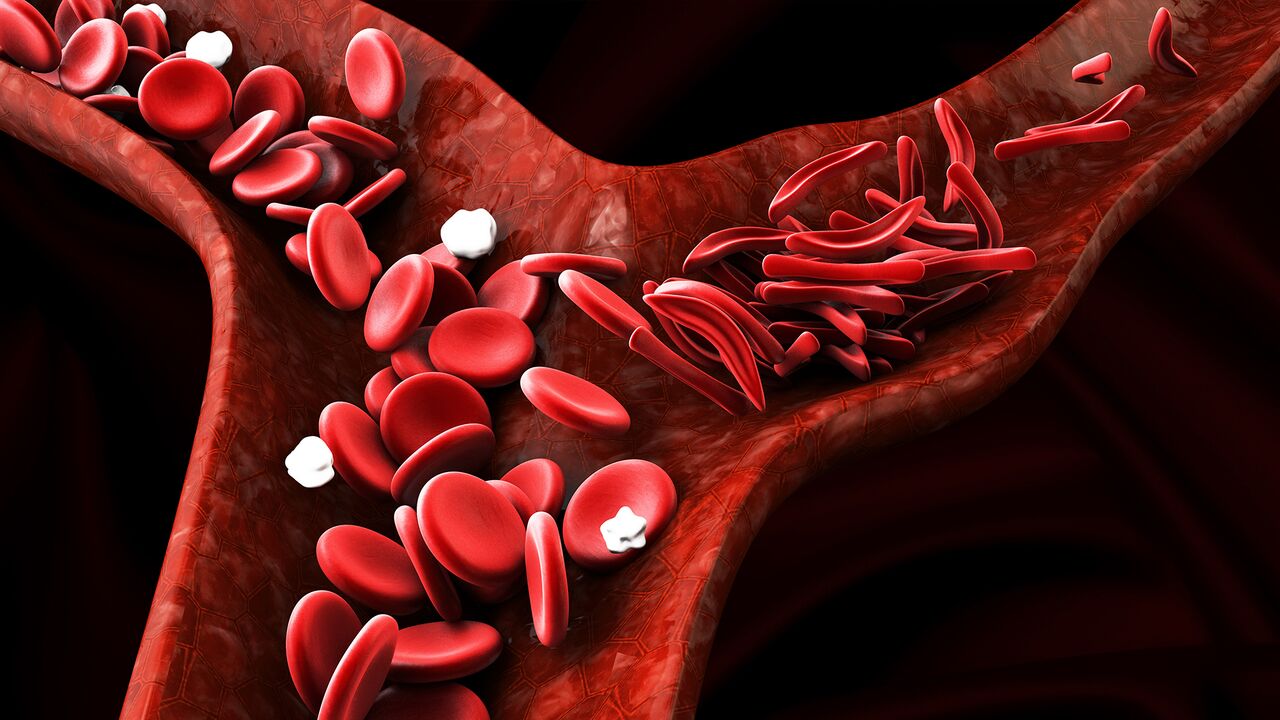
Pulmonary embolism occurs when one of your pulmonary arteries within your lungs becomes blocked, commonly from a blood clot. These clots most often originate in your legs, a condition known as deep vein thrombosis (DVT). When a blood clot travels from your legs (DVT) and gets lodged in your lungs (PE), it's a condition called venous thromboembolism, and it turns serious quickly as your blood’s oxygen levels drop drastically, putting your heart, lungs, and other organs in jeopardy. If you receive medical treatment promptly, your chance for survival improves greatly.
Blood clots are not the only cause of pulmonary embolism. Air bubbles, a piece of a tumor, collagen, or marrow fat from a broken bone can occasionally become stuck in a blood vessel and lead to blockage.
Pulmonary hypertension can also result from a pulmonary embolism. Your blood pressure spikes, endangering your lungs and heart. Without a clear path, your heart has to pump harder and faster to get blood through the vessels, raising your blood pressure. Your heart cannot sustain for very long at this rate, and will soon weaken and become damaged.
Pulmonary Embolism Symptoms
The symptoms of pulmonary embolism show up differently in each person because factors like clot size and existing lung damage can affect how symptoms appear and their severity. If you also suffer from pre-existing diseases that impact your heart and lungs, such as cardiovascular disease, your symptoms may be more intense.
Common pulmonary embolism signs include:
- Breathing complications: You may experience shortness of breath and difficulty catching your breath when exercising, along with increased heart rate and rapid breathing.
- Bloody cough: A dry hacking cough that brings up blood is common.
- Chest pain: You may feel a tightness in your chest that becomes more intense when you take a deep breath or cough, and does not improve. You may also have an increased heartbeat.
- Feeling faint: Due to changes in blood pressure, you may feel dizzy or lightheaded.
- Swelling of legs: You may have swelling below the knee in one or both legs.
- Skin changes: You may notice your coloring changing or a feeling of clamminess.
- Fever
- Sweating
If you are experiencing any of these common symptoms, it’s vital to seek immediate medical attention.
Pulmonary Embolism Risk Factors
Anyone can develop blood clots that lead to pulmonary embolism, but certain factors can put you at a higher risk.
1. Recent Surgery
Anytime you have surgery, your doctors will warn against blood clots following the procedure and will provide detailed instructions on how to prevent them. You may receive medication, as well as orders to get up and move around frequently during recovery.
2. Family and Medical History
Like many conditions, a family history of pulmonary embolism can up your chances of having it. If your relatives have blood clot issues, or if you have already experienced them earlier in your life, you may have a higher chance of pulmonary embolism occurring.
3. Obesity
Carrying excess weight puts you at a high risk for circulatory issues and the potential for blood clots forming. Obese females are particularly susceptible, and weight-loss efforts are important when trying to prevent pulmonary embolism from developing.
4. Bed Rest
If you are recovering from an illness, be it a heart attack or leg fracture, your health is compromised, or you’ve been ordered bed rest, clots are definitely a risk. Residents of nursing homes and hospitals are often at a higher risk when confined to a bed and not able to get up and move around to maintain healthy circulation.
5. Travel
We are often sitting for long periods of time during extended car rides or plane trips, cutting off proper circulation to parts of our bodies. Without standing, stretching, and walking around, blood can collect in the legs, and your chances of clotting and pulmonary embolisms can greatly increase.
6. Pregnancy
Carrying a child is a tough job in and of itself, but it can be dangerous if the position of your baby pinches off blood flow in your pelvis, slowing down circulation and causing blood to pool in your legs.
7. Smoking
Smoking and the harmful chemicals within tobacco smoke can damage the lining of your blood vessels, cause plaque to accumulate in your arteries, and weaken your heart and lungs, increasing your risk of clotting.
Suffering from other medical conditions such as atrial fibrillation, heart disease or heart failure, as well as the medications used to treat them, can up your risk for pulmonary embolism. Birth control pills are also a culprit for clots because the hormones within them increase the possibility of clot formation within a woman’s body.
Pulmonary Embolism Diagnosis and Treatment
Not an easy disease to treat, pulmonary embolism is diagnosed with the help of several different types of tests.
- Blood tests: Your physician will likely order a blood test for the clot-dissolving substance D dimer. High D dimer levels signal blood clots. A blood clot can lower your blood oxygen levels, so blood tests that measure carbon dioxide and oxygen levels in the blood are also typically administered. There are also blood tests that can check to see if you have a genetic clotting disorder.
- Chest X-ray: Used to photograph your heart and lungs, X-rays can't offer a PE diagnosis, but can help to rule out other conditions that present in the same way.
- Ultrasound: An ultrasonography uses sound waves to find blood clots in your thigh veins and behind the knees.
- Spiral CT scan: Spiraling around your body, the CT scan takes 3-D images to detect abnormalities in the arteries in your lungs.
- Pulmonary angiogram: The most accurate of the tests, a pulmonary angiogram takes a detailed picture of the blood flow in your lungs. It is potentially risky and usually given as a last resort. It can temporarily alter your heart rhythm, and the dye may cause further harm to the kidneys in those with impaired kidney function.
- MRI: Due to the expense, MRIs are typically only given to pregnant women, as radiation from other tests can harm the fetus, and to people with decreased kidney function who are at risk from the dyes used in other diagnostic tests.
Pulmonary embolism treatment may differ from one patient to the next. Whether you need to head to the hospital is the first decision your health care provider will make to ensure your health and life are not in jeopardy.
If you are not in an emergency situation and your vital signs are good, you may receive an at-home plan of action. If test results indicate that any of your organs are in distress or levels in the blood are concerning, you most likely will head to the hospital for needed medical care.
Pulmonary embolism treatment options include preventing the blood clot from getting larger and causing any further damage. Medications known as blood thinners, or anticoagulants, keep your blood from becoming thicker and adding to clot growth. You will be given regular blood tests to ensure these drugs are working properly, while not increasing your risk of bleeding.
Another type of treatment for pulmonary embolism is called thrombolytic therapy. These clot-busting drugs help dissolve the existing clot to open the space within your artery. If administered in time, permanent damage to the lungs, stroke, and cardiac arrest can hopefully be avoided.

Pulmonary Embolism Prevention
Preventing blood clots is key to stopping pulmonary embolisms before they happen. It is essential to follow your doctor’s orders when recovering from surgery or if you are restricted to bed for periods of time due to an illness. There are several methods of preventing blood clots, and you most likely will be prescribed one or more of them depending on your situation.
Medication
You may be given anticoagulants before and after surgery or if you are in the hospital for other lung or heart issues.
Walking
You may be told to get up and move around as soon as you can following a surgical procedure to keep blood flowing and everything working properly. It may seem counterintuitive to stand and walk after a procedure, but it can actually speed healing and prevent life-threatening issues from developing.
Compression Socks
These special types of socks apply a gentle pressure to the lower leg, allowing the blood to move freely and prevent pooling. These may be given to you following an operation, to prevent clots due to a current condition, or can be worn when traveling. A study showed airline travelers who wore compression stockings had less leg swelling or circulatory issues following the flight.
Compression Pump
This treatment uses thigh-high or calf-high cuffs that automatically inflate with air and deflate every few minutes to massage and squeeze the veins in your legs and improve blood flow.
Elevating Legs
Propping your legs up slightly, especially while sleeping, can prevent clots from forming in your lower extremities. Your doctor may suggest putting a pillow under your legs to support healthy circulation.
Traveling Tip
Your risk of developing blood clots while traveling is rare, but can go up the longer you travel. If you are at risk for blood clots, it’s important to:
- Keep hydrated: Drinking water frequently throughout the day is essential to preventing dehydration and upping your chances of blood clots. You will want to limit alcoholic beverages as well since they can add to dehydration.
- Flex your legs: While seated, rotate your ankles and flex your feet back and forth to help keep blood flowing.
- Get moving: While in the air, get out of your seat every hour if possible and walk up and down the aisle. If you’re on a road trip, pull over periodically to walk and stretch.
- Wear compression socks/stockings
Natural Prevention Methods
To help reduce your risk of pulmonary embolism, it’s important to eat a well-balanced diet, maintain a healthy weight, and stay active. Getting regular exercise is essential to maintaining healthy lungs, heart, and circulation. If you sit for long periods for work or travel, make sure you are taking breaks to get up and move around. In combination with following a healthy lifestyle and orders from your doctor, eating certain foods and supplements can also help prevent blood clots.
Salicylates
You may have heard of salicylic acid in relation to aspirin, since it is its active ingredient. Salicylates are the salt of salicylic acid and are found naturally in your food and in over-the-counter items. They contain anti-inflammatory and pain-relieving properties and can mimic the anticoagulation abilities of aspirin. Naturally occurring sources of salicylates include spices like thyme, ginger, cinnamon, turmeric, curry powder, and paprika. Honey, tea, pineapple juice, and white and red wine are drinks that include salicylates.
Vitamin E
Vitamin E has antioxidant and anticoagulant properties and can lessen the chance of life-threatening clots heading to your lungs. A study specifically targeting women found that supplementing with vitamin E reduced the risk of clots from forming in the legs, especially if predisposed to issues in the past.
Vitamin D and Omega-3s
You may think of healthy bones when discussing vitamin D, but it is also essential for preventing blood clots from forming. You can get vitamin D from your food, taking a supplement, or by stepping out into the sun for a short period of time.
You may also want to supplement with fish oil and omega-3 fatty acids. Eating herring, tuna, salmon, and anchovies can provide an excellent source of omega-3 fatty acids. The chance of blood clots forming and grouping can be decreased by incorporating omega-3 fatty acids into your diet.
Garlic
Three compounds in garlic (allicin, adenosine, and paraffinic sulfide) are thought to help prevent platelets from grouping together properly.
Chocolate
Chocolate has been said to have many health benefits, including aiding clot prevention. Dark chocolate has been found to affect clot accumulation. The flavanols found in cocoa help boost chocolate’s effect on keeping clots at bay. A study revealed that flavonoid-rich dark chocolate can help decrease the chance of platelets grouping and sticking to artery walls.
Amino Acids
Poor circulation has been tied to a lack of an adequate amount of nitric oxide, which is needed for your blood to move throughout your body efficiently. Nitric oxide is found in your body and can be obtained from foods and supplements. The amino acids citrulline and arginine help boost nitric oxide and expand vessels, allowing blood to flow freely. You can increase your nitric oxide levels and boost circulation by eating foods containing these amino acids.
You can find citrulline in beans, garlic, watermelon, salmon, chicken, cucumbers, eggs, tuna, and cantaloupe. Adding seafood, nuts, spinach, legumes, whole grains, and soy to your plate can give you good sources of arginine.
Another important amino acid is taurine, which increases the absorption of the vital minerals magnesium and potassium in the heart. This, in turn, helps to stabilize and regulate heart muscle contractions. Natural sources of taurine include shellfish, coldwater fish, eggs, dairy products, seaweed, and dark chicken meat.
You can enhance your diet with an expertly formulated amino acid supplement to ensure you are receiving a balanced amount of all the essentials. Life is an essential amino acid supplement designed to help prevent the natural decline of muscle and heart function that begins at around age 40. You can learn more about the science behind Life here.

Up to 25% off Amino
Shop NowTAGS: conditions natural cures
Join the Community
Comments (0)
Most Craveable Recipes



 833-264-6620
833-264-6620



















